Working Group 2 - Chapter 8: Human Health - (AR4-WG2-8)
Original at: http://www.ipcc.ch/publications_and_data/ar4/wg2/en/ch8.html
Main AR4 Index | Working Group WG2 Index | Table of Contents | Authors | Executive Summary | Annotated Text | References | Reviewer Comments
With the exception of Chapter and Section headings, all coloured text has been inserted by AccessIPCC. The non-coloured text is the IPCC original.
A number of emails from the Climate Research Unit (CRU) of the University of East Anglia were published on the Internet in November 2009. This has provided a window into the world of climate science.
We have identified a number of key individuals involved in the emails whom we have designated as Persons of Concern [PoC]; a Journal in which a PoC has published has been designated as a Journal of Concern [JoC].
This is not to suggest that we believe such papers are necessarily flawed, but rather that, as Joseph Alcamo noted at Bali in October 2009, "as policymakers and the public begin to grasp the multi-billion dollar price tag for mitigating and adapting to climate change, we should expect a sharper questioning of the science behind climate policy".
References occur in a list at the end of each chapter. Citations are within the normal text of sections and paragraphs.
| Tag | Explanation | Where Used | References | Citations |
|---|---|---|---|---|
| PoC |
Person of Concern Key individual involved in CRU emails as defined in this spreadsheet. |
References, Citations, IPCC Roles | 1 | - |
| JoC |
Journal of Concern A Journal which has published articles by one or more PoCs (Person of Concern) |
References, Citations | 48 | 54 |
| MoS |
Model or Simulation Reference appears to be a model or simulation, not observation or experiment |
References, Citations | 54 | 57 |
| NPR |
Non Peer Reviewed Reference has no Journal or no Volume or no Pages or it has Editors. |
References, Citations | 141 | 130 |
| SRC |
Self Reference Concern Author of a chapter containing references to own work. |
References, Citations, IPCC Roles | 59 | 68 |
| ARC |
Paper authored or co-authored by person who is also in list of Authors of another chapter. |
References, Citations | 43 | 44 |
| 2007 |
Paper dated 2007, when IPCC policy stated cutoff was December 2005 |
References, Citations | 9 | 8 |
| Ambiguous |
The short inline citation matched with more than one reference; however, AccessIPCC will link to the first reference found. |
Citations | - | 15 |
| NotFound |
The short inline citation was not matched with any reference. Believed to be caused by typing errors. |
Citations | - | 2 |
| Clean |
The reference was probably peer reviewed. |
References, Citations | 289 | 314 |
Coordinating Lead Authors:
Ulisses Confalonieri (Brazil) [SRC:1], Bettina Menne (WHO Regional Office for Europe/Germany) [SRC:9],
| Concern | Occurrence |
|---|---|
| SRC >= 5 | 1 |
| SRC 1-4 | 1 |
| Potentially Biased Authors | 2 |
Lead Authors:
Rais Akhtar (India) [SRC:2], Kristie L. Ebi (USA) [SRC:13], Maria Hauengue (Mozambique), R. Sari Kovats (UK), Boris Revich (Russia) [SRC:1], Alistair Woodward (New Zealand) [SRC:7],
| Concern | Occurrence |
|---|---|
| SRC >= 5 | 2 |
| SRC 1-4 | 2 |
| Potentially Biased Authors | 4 |
| Impartial Authors | 2 |
Contributing Authors:
Tarakegn Abeku (Ethiopia) [SRC:2], Mozaharul Alam (Bangladesh), Paul Beggs (Australia) [SRC:3], Bernard Clot (Switzerland) [SRC:1], Chris Furgal (Canada) [SRC:4], Simon Hales (New Zealand) [SRC:11], Guy Hutton (UK), Sirajul Islam (Bangladesh), Tord Kjellstrom (New Zealand/Sweden) [SRC:1], Nancy Lewis (USA), Anil Markandya (UK), Glenn McGregor (New Zealand) [SRC:2], Kirk R. Smith (USA) [SRC:3], Christina Tirado (Spain), Madeleine Thomson (UK) [SRC:6], Tanja Wolf (WHO Regional Office for Europe/Germany),
| Concern | Occurrence |
|---|---|
| SRC >= 5 | 2 |
| SRC 1-4 | 7 |
| Potentially Biased Authors | 9 |
| Impartial Authors | 7 |
Review Editors:
Susanna Curto (Argentina), Anthony McMichael (Australia) [SRC:12],
| Concern | Occurrence |
|---|---|
| SRC >= 5 | 1 |
| Potentially Biased Authors | 1 |
| Impartial Authors | 1 |
This chapter should be cited as:
Confalonieri, U., B. Menne, R. Akhtar, K.L. Ebi, M. Hauengue, R.S. Kovats, B. Revich and A. Woodward, 2007: Human health. Climate Change 2007: Impacts, Adaptation and Vulnerability. Contribution of Working Group II to the Fourth Assessment Report of the Intergovernmental Panel on Climate Change, M.L. Parry, O.F. Canziani, J.P. Palutikof, P.J. van der Linden and C.E. Hanson, Eds., Cambridge University Press, Cambridge, UK, 391-431.
Executive summary
Climate change currently contributes to the global burden of disease and premature deaths (very high confidence).
Human beings are exposed to climate change through changing weather patterns (temperature, precipitation, sea-level rise and more frequent extreme events) and indirectly through changes in water, air and food quality and changes in ecosystems, agriculture, industry and settlements and the economy. At this early stage the effects are small but are projected to progressively increase in all countries and regions. [ 8.4.1 ]
Emerging evidence of climate change effects on human health shows that climate change has:
- altered the distribution of some infectious disease vectors (medium confidence) [ 8.2.8 ];
- altered the seasonal distribution of some allergenic pollen species (high confidence) [ 8.2.7 ];
- increased heatwave-related deaths (medium confidence) [ 8.2.1 ].
Projected trends in climate-change-related exposures of importance to human health will:
- increase malnutrition and consequent disorders, including those relating to child growth and development (high confidence) [ 8.2.3 , 8.4.1 ];
- increase the number of people suffering from death, disease and injury from heatwaves, floods, storms, fires and droughts (high confidence) [ 8.2.2 , 8.4.1 ];
- continue to change the range of some infectious disease vectors (high confidence) [ 8.2 , 8.4 ];
- have mixed effects on malaria; in some places the geographical range will contract, elsewhere the geographical range will expand and the transmission season may be changed (very high confidence) [ 8.4.1.2 ];
- increase the burden of diarrhoeal diseases (medium confidence) [ 8.2 , 8.4 ];
- increase cardio-respiratory morbidity and mortality associated with ground-level ozone (high confidence) [ 8.2.6 , 8.4.1.4 ];
- increase the number of people at risk of dengue (low confidence) [ 8.2.8 , 8.4.1 ];
- bring some benefits to health, including fewer deaths from cold, although it is expected that these will be outweighed by the negative effects of rising temperatures worldwide, especially in developing countries (high confidence) [ 8.2.1 , 8.4.1 ].
Adaptive capacity needs to be improved everywhere; impacts of recent hurricanes and heatwaves show that even high-income countries are not well prepared to cope with extreme weather events (high confidence). [ 8.2.1 , 8.2.2 ]
Adverse health impacts will be greatest in low-income countries. Those at greater risk include, in all countries, the urban poor, the elderly and children, traditional societies, subsistence farmers, and coastal populations (high confidence). [ 8.1.1 , 8.4.2 , 8.6.1.3 , 8.7 ]
Economic development is an important component of adaptation, but on its own will not insulate the world’s population from disease and injury due to climate change (very high confidence).
Critically important will be the manner in which economic growth occurs, the distribution of the benefits of growth, and factors that directly shape the health of populations, such as education, health care, and public-health infrastructure. [ 8.3.2 ]
8.1 Introduction
This chapter describes the observed and projected health impacts of climate change, current and future populations at risk, and the strategies, policies and measures that have been and can be taken to reduce impacts. The chapter reviews the knowledge that has emerged since the Third Assessment Report (TAR) ( McMichael et al., 2001 [NPR, SRC] ). Published research continues to focus on effects in high-income countries, and there remain important gaps in information for the more vulnerable populations in low- and middle-income countries.
8.1.1 State of health in the world
Health includes physical, social and psychological well-being. Population health is a primary goal of sustainable development. Human beings are exposed to climate change through changing weather patterns (for example more intense and frequent extreme events) and indirectly though changes in water, air, food quality and quantity, ecosystems, agriculture, livelihoods and infrastructure ( Figure 8.1 ). These direct and indirect exposures can cause death, disability and suffering. Ill-health increases vulnerability and reduces the capacity of individuals and groups to adapt to climate change. Populations with high rates of disease and debility cope less successfully with stresses of all kinds, including those related to climate change.
In many respects, population health has improved remarkably over the last 50 years. For instance, average life expectancy at birth has increased worldwide since the 1950 s ( WHO, 2003b [NPR, MoS] , 2004b ). However, improvement is not apparent everywhere, and substantial inequalities in health persist within and between countries ( (Casas-Zamora and Ibrahim, 2004; ) McMichael et al., 2004 [Ambiguous] ;( Marmot, 2005; ) People’s Health Movement et al., 2005 ). In parts of Africa, life expectancy has fallen in the last 20 years, largely as a consequence of HIV/AIDS; in some countries more than 20% of the adult population is infected ( UNDP, 2005 [NPR] ). Globally, child mortality decreased from 147 to 80 deaths per 1,000 live births from 1970 to 2002 ( WHO, 2002b [NPR] ). Reductions were largest in countries in the World Health Organization (WHO) regions of the Eastern Mediterranean, South-East Asia and Latin America. In sixteen countries (fourteen of which are in Africa), current levels of under-five mortality are higher than those observed in 1990 ( (Anand and Barnighausen, 2004 ) ). The Millennium Development Goal (MDG) of reducing under-five mortality rates by two-thirds by 2015 is unlikely to be reached in these countries.
Non-communicable diseases, such as heart disease, diabetes, stroke and cancer, account for nearly half of the global burden of disease (at all ages) and the burden is growing fastest in low- and middle-income countries ( Mascie-Taylor and Karim, 2003 [JoC] ). Communicable diseases are still a serious threat to public health in many parts of the world ( WHO, 2003a [NPR] ) despite immunisation programmes and many other measures that have improved the control of once-common human infections. Almost 2 million deaths a year, mostly in young children, are caused by diarrhoeal diseases and other conditions that are attributable to unsafe water and lack of basic sanitation ( Ezzati et al., 2003 [MoS] ). Malaria, another common disease whose geographical range may be affected by climate change, causes around 1 million child deaths annually ( WHO, 2003b [NPR, MoS] ). Worldwide, 840 million people were under-nourished in 1998 - 2000 ( FAO, 2002 [NPR] ). Progress in overcoming hunger is very uneven. Based on current trends, only Latin America and the Caribbean will achieve the MDG target of halving the proportion of people who are hungry by 2015 ( FAO, 2005 [NPR] ; UN, 2006a [NPR] ).
8.1.2 Findings from the Third Assessment Report
The main findings of the IPCC TAR ( McMichael et al., 2001 [NPR, SRC] ) were as follows.
- An increase in the frequency or intensity of heatwaves will increase the risk of mortality and morbidity, principally in older age groups and among the urban poor.
- Any regional increases in climate extremes (e.g., storms, floods, cyclones, droughts) associated with climate change would cause deaths and injuries, population displacement, and adverse effects on food production, freshwater availability and quality, and would increase the risks of infectious disease, particularly in low-income countries.
- In some settings, the impacts of climate change may cause social disruption, economic decline, and displacement of populations. The health impacts associated with such socio-economic dislocation and population displacement are substantial.
- Changes in climate, including changes in climate variability, would affect many vector-borne infections. Populations at the margins of the current distribution of diseases might be particularly affected.
- Climate change represents an additional pressure on the world’s food supply system and is expected to increase yields at higher latitudes and decrease yields at lower latitudes. This would increase the number of undernourished people in the low-income world, unless there was a major redistribution of food around the world.
- Assuming that current emission levels continue, air quality in many large urban areas will deteriorate. Increases in exposure to ozone and other air pollutants (e.g., particulates) could increase morbidity and mortality.
8.1.3 Key developments since the Third Assessment Report
Overall, research over the last 6 years has provided new evidence to expand the findings of the TAR. Empirical research has further quantified the health effects of heatwaves (see Section 8.2.1 ). There has been little additional research on the health effects of other extreme weather events. The early effects of climate change on health-relevant exposures have been investigated in the context of changes in air quality and plant and animal phenology (see Chapter 1 and Sections 8.2.7 and 8.2.8 ). There has been research on a wider range of health issues, including food safety and water-related infections. The contribution made by climate change to the overall burden of disease has been estimated (see Section 8.4.1 ( McMichael, 2004 [Ambiguous] ). Several countries have conducted health-impact assessments of climate change; either as part of a multi-sectoral study or as a stand-alone project (see Tables 8.1 , 8.3 and 8.4 ). These provide more detailed information on population vulnerability to climate change (see Section 8.4.2 ). The effect of climate has been studied in the context of other social and environmental determinants of health outcomes ( McMichael et al., 2003a [NPR, SRC] ; Izmerov et al., 2005 [NPR, SRC] ). Little advancement has been made in the development of climate–health impact models that project future health effects. Climate change is now an issue of concern for health policy in many countries. Some adaptation measures specific to climate variability have been developed and implemented within and beyond the health sector (see Section 8.6 ). Many challenges remain for climate- and health-impact and adaptation research. The most important of these is the limited capacity for research and adaptation in low- and middle-income countries.
8.1.4 Methods used and gaps in knowledge
The evidence for the current sensitivity of population health to weather and climate is based on five main types of empirical study:
- health impacts of individual extreme events (e.g., heatwaves, floods, storms, droughts, extreme cold);
- spatial studies where climate is an explanatory variable in the distribution of the disease or the disease vector;
- temporal studies assessing the health effects of interannual climate variability, of short-term (daily, weekly) changes in temperature or rainfall, and of longer-term (decadal) changes in the context of detecting early effects of climate change;
- experimental laboratory and field studies of vector, pathogen, or plant (allergen) biology;
- intervention studies that investigate the effectiveness of public-health measures to protect people from climate hazards.
This assessment of the potential future health impacts of climate change is conducted in the context of:
- limited region-specific projections of changes in exposures of importance to human health;
- the consideration of multiple, interacting and multi-causal health outcomes;
- the difficulty of attributing health outcomes to climate or climate change per se;
- the difficulty of generalising health outcomes from one setting to another, when many diseases (such as malaria) have important local transmission dynamics that cannot easily be represented in simple relationships;
- limited inclusion of different developmental scenarios in health projections;
- the difficulty in identifying climate-related thresholds for population health;
- limited understanding of the extent, rate, limiting forces and major drivers of adaptation of human populations to a changing climate.
Table 8.1. National health impact assessments of climate change published since the TAR.
| Country | Key findings | Adaptation recommendations |
|---|---|---|
|
Australia (McMichael et al., 2003b) |
Increase in heatwave-related deaths; drowning from floods; diarrhoeal disease in indigenous communities; potential change in the geographical range of dengue and malaria; likely increase in environmental refugees from Pacific islands. |
Not considered. |
|
Bolivia (Programa Nacional de Cambios Climaticos Componente Salud et al., 2000) |
Intensification of malaria and leishmaniasis transmission. Indigenous populations may be most affected by increases in infectious diseases. |
Not considered. |
|
Bhutan (National Environment Commission et al., 2006) |
Loss of life from frequent flash floods; glacier lake outburst floods; landslides; hunger and malnutrition; spread of vector-borne diseases into higher elevations; loss of water resources; risk of water-borne diseases. |
Ensure safe drinking water; regular vector control and vaccination programmes; monitor air and drinking water quality; establishment of emergency medical services. |
|
Canada (Riedel, 2004) |
Increase in heatwave-related deaths; increase in air pollution-related diseases; spread of vector- and rodent-borne diseases; increased problems with contamination of both domestic and imported shellfish; increase in allergic disorders; impacts on particular populations in northern Canada. |
Monitoring for emerging infectious diseases; emergency management plans; early warning systems; land-use regulations; upgrading water and wastewater treatment facilities; measures for reducing the heat-island effect. |
|
Finland (Hassi and Rytkonen, 2005) |
Small increase in heat-related mortality; changes in phenological phases and increased risk of allergic disorders; small reduction in winter mortality. |
Awareness-building and training of medical doctors. |
|
Germany (Zebisch et al., 2005) |
Observed excess deaths from heatwaves; changing ranges in tick-borne encephalitis; impacts on health care. |
Increase information to the population; early warning; emergency planning and cooling of buildings; insurance and reserve funds. |
|
India (Ministry of Environment and Forest and Government of India, 2004) |
Increase in communicable diseases. Malaria projected to move to higher latitudes and altitudes in India. |
Surveillance systems; vector control measures; public education. |
|
Japan (Koike, 2006) |
Increased risk of heat-related emergency visits, Japanese cedar pollen disease patients, food poisoning; and sleep disturbance. |
Heat-related emergency visit surveillance. |
|
The Netherlands (Bresser, 2006) |
Increase in heat-related mortality, air pollutants; risk of Lyme disease, food poisoning and allergic disorders. |
Not considered. |
|
New Zealand (Woodward et al., 2001) |
Increases in enteric infections (food poisoning); changes in some allergic conditions; injuries from more intense floods and storms; a small increase in heat-related deaths. |
Systems to ensure food quality; information to population and health care providers; flood protection; vector control. |
|
Panama (Autoridad Nacional del Ambiente, 2000) |
Increase of vector-borne and other infectious diseases; health problems due to high ozone levels in urban areas; increase in malnutrition. |
Not considered. |
|
Portugal (Casimiro and Calheiros, 2002; Calheiros and Casimiro, 2006) |
Increase in heat-related deaths and malaria (Tables 8.2 , 8.3 ), food- and water-borne diseases, West Nile fever, Lyme disease and Mediterranean spotted fever; a reduction in leishmaniasis risk in some areas. |
Address thermal comfort; education and information as well as early warning for hot periods; and early detection of infectious diseases. |
|
Spain (Moreno, 2005) |
Increase in heat-related mortality and air pollutants; potential change of ranges of vector- and rodent-borne diseases. |
Awareness-raising; early warning systems for heatwaves; surveillance and monitoring; review of health policies. |
|
Tajikistan (Kaumov and Muchmadeliev, 2002) |
Increase in heat-related deaths. |
Not considered. |
|
Switzerland (Thommen Dombois and Braun-Fahrlaender, 2004) |
Increase of heat-related mortality; changes in zoonoses; increase in cases of tick-borne encephalitis. |
Heat information, early warning; greenhouse gas emissions reduction strategies to reduce secondary air pollutants; setting up a working group on climate and health. |
|
United Kingdom (Department of Health and Expert Group on Climate Change and Health in the UK, 2001) |
Health impacts of increased flood events; increased risk of heatwave-related mortality; and increased ozone-related exposure. |
Awareness-raising. |
8.2 Current sensitivity and vulnerability
Systematic reviews of empirical studies provide the best evidence for the relationship between health and weather or climate factors, but such formal reviews are rare. In this section, we assess the current state of knowledge of the associations between weather/climate factors and health outcome(s) for the population(s) concerned, either directly or through multiple pathways, as outlined in Figure 8.1 . The figure shows not only the pathways by which health can be affected by climate change, but also shows the concurrent direct-acting and modifying (conditioning) influences of environmental, social and health-system factors.
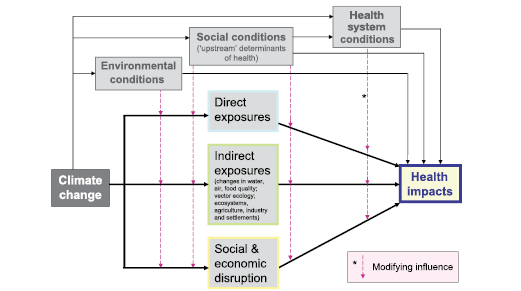
Figure 8.1. Schematic diagram of pathways by which climate change affects health, and concurrent direct-acting and modifying (conditioning) influences of environmental, social and health-system factors.
Published evidence so far indicates that:
- climate change is affecting the seasonality of some allergenic species (see Chapter 1 ) as well as the seasonal activity and distribution of some disease vectors (see Section 8.2.8 );
- climate plays an important role in the seasonal pattern or temporal distribution of malaria, dengue, tick-borne diseases, cholera and some other diarrhoeal diseases (see Sections 8.2.5 and 8.2.8 );
- heatwaves and flooding can have severe and long-lasting effects.
8.2.1 Heat and cold health effects
The effects of environmental temperature have been studied in the context of single episodes of sustained extreme temperatures (by definition, heatwaves and cold-waves) and as population responses to the range of ambient temperatures (ecological time-series studies).
8.2.1.1 Heatwaves
Hot days, hot nights and heatwaves have become more frequent ( IPCC, 2007a [NPR, 2007] ). Heatwaves are associated with marked short-term increases in mortality ( Box 8.1 ). There has been more research on heatwaves and health since the TAR in North America ( (Basu and Samet, 2002 ) ), Europe ( Koppe et al., 2004 [NPR, SRC] ) and East Asia ( (Qiu et al., 2002; ) ( Ando et al., 2004; ) ( Choi et al., 2005; ) Kabuto et al., 2005 [ARC] ).
A variable proportion of the deaths occurring during heatwaves are due to short-term mortality displacement ( (Hajat et al., 2005; ) ( Kysely, 2005 ) ). Research indicates that this proportion depends on the severity of the heatwave and the health status of the population affected ( (Hemon and Jougla, 2004; ) ( Hajat et al., 2005 ) ). The heatwave in 2003 was so severe that short-term mortality displacement contributed very little to the total heatwave mortality ( (Le Tertre et al., 2006 ) ).
Eighteen heatwaves were reported in India between 1980 and 1998, with a heatwave in 1988 affecting ten states and causing 1,300 deaths ( (De and Mukhopadhyay, 1998; ) Mohanty and Panda, 2003 [NPR] ;( de et al., 2004 ) ). Heatwaves in Orissa, India, in 1998, 1999 and 2000 caused an estimated 2,000, 91 and 29 deaths, respectively ( Mohanty and Panda, 2003 [NPR] ) and heatwaves in 2003 in Andhra Pradesh, India, caused more than 3000 deaths (Government of Andhra Pradesh, 2004 ). Heatwaves in South Asia are associated with high mortality in rural populations, and among the elderly and outdoor workers ( (Chaudhury et al., 2000 ) ) (see Section 8.2.9 ). The mortality figures probably refer to reported deaths from heatstroke and are therefore an underestimate of the total impact of these events.
Box 8.1. The European heatwave 2003: impacts and adaptation
In August 2003, a heatwave in France caused more than 14,800 deaths ( Figure 8.2 ). Belgium, the Czech Republic, Germany, Italy, Portugal, Spain, Switzerland, the Netherlands and the UK all reported excess mortality during the heatwave period, with total deaths in the range of 35,000 ( (Hemon and Jougla, 2004; ) ( Martinez-Navarro et al., 2004; ) ( Michelozzi et al., 2004; ) ( Vandentorren et al., 2004; ) ( Conti et al., 2005; ) ( Grize et al., 2005; ) Johnson et al., 2005 [SRC] ). In France, around 60% of the heatwave deaths occurred in persons aged 75 and over ( (Hemon and Jougla, 2004 ) ). Other harmful exposures were also caused or exacerbated by the extreme weather, such as outdoor air pollutants (tropospheric ozone and particulate matter) ( EEA, 2003 [NPR] ), and pollution from forest fires.
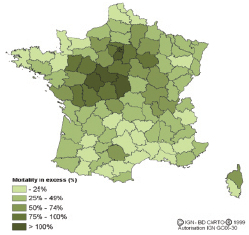
Figure 8.2. (a) The distribution of excess mortality in France from 1 to 15 August 2003, by region, compared with the previous three years ( INVS, 2003 [NPR] ); (b) the increase in daily mortality in Paris during the heatwave in early August ( Vandentorren and Empereur-Bissonnet, 2005 [NPR] ).
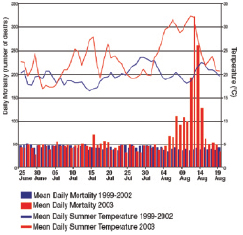
A French parliamentary inquiry concluded that the health impact was ‘unforeseen’, surveillance for heatwave deaths was inadequate, and the limited public-health response was due to a lack of experts, limited strength of public-health agencies, and poor exchange of information between public organisations ( (Lagadec, 2004; ) Sénat, 2004 ).
In 2004, the French authorities implemented local and national action plans that included heat health-warning systems, health and environmental surveillance, re-evaluation of care of the elderly, and structural improvements to residential institutions (such as adding a cool room) ( Laaidi et al., 2004 [NPR] ; Michelon et al., 2005 [NPR] ). Across Europe, many other governments (local and national) have implemented heat health-prevention plans ( (Michelozzi et al., 2005; ) WHO Regional Office for Europe, 2006 ).
Since the observed higher frequency of heatwaves is likely to have occurred due to human influence on the climate system ( Hegerl et al., 2007 [NPR, ARC, 2007] ), the excess deaths of the 2003 heatwave in Europe are likely to be linked to climate change.
8.2.1.2 Cold-waves
Cold-waves continue to be a problem in northern latitudes, where very low temperatures can be reached in a few hours and extend over long periods. Accidental cold exposure occurs mainly outdoors, among socially deprived people (alcoholics, the homeless), workers, and the elderly in temperate and cold climates ( (Ranhoff, 2000 ) ). Living in cold environments in polar regions is associated with a range of chronic conditions in the non-indigenous population ( Sorogin et al, 1993 [NPR] ) as well as with acute risk from frostbite and hypothermia ( Hassi et al., 2005 [Ambiguous] ). In countries with populations well adapted to cold conditions, cold-waves can still cause substantial increases in mortality if electricity or heating systems fail. Cold-waves also affect health in warmer climates, such as in South-East Asia ( EM-DAT, 2006 [NPR] ).
The sensitivity of a population to temperature extremes changes over decadal time-scales ( Honda et al., 1998 [MoS, ARC] ). There is some indication that populations in the USA became less sensitive to high temperatures over the period 1964 to 1988 (as measured imprecisely by population- and period-specific thresholds in the mortality response) ( (Davis et al., 2002, ) 2003, 2004 ). Heat-related mortality has declined since the 1970 s in South Carolina, USA, and south Finland, but this trend was less clear for the south of England ( (Donaldson et al., 2003 ) ). Cold-related mortality in European populations has also declined since the 1950 s ( (Kunst et al., 1991; ) ( Lerchl, 1998; ) ( Carson et al., 2006 ) ). Cold days, cold nights and frost days have become rarer, but explain only a small part of this reduction in winter mortality; as improved home heating, better general health and improved prevention and treatment of winter infections have played a more significant role ( (Carson et al., 2006 ) ). In general, population sensitivity to cold weather is greater in temperate countries with mild winters, as populations are less well-adapted to cold (Eurowinter Group, 1997; ( Healy, 2003 ) ).
8.2.1.3 Estimates of heat and cold effects
Methods for the quantification of heat and cold effects have seen rapid development ( (Braga et al., 2002; ) Curriero et al., 2002 [ARC] ; Armstrong et al., 2004 [SRC] ), including the identification of medical, social, environmental and other factors that modify the temperature–mortality relationship ( (Basu and Samet, 2002; ) Koppe et al., 2004 [NPR, SRC] ). Local factors, such as climate, topography, heat-island magnitude, income, and the proportion of elderly people, are important in determining the underlying temperature–mortality relationship in a population ( Curriero et al., 2002 [ARC] ;( Hajat, 2006 ) ). High temperatures contribute to about 0.5 - 2% of annual mortality in older age groups in Europe ( (Pattenden et al., 2003; ) ( Hajat et al., 2006 ) ), although large uncertainty remains in quantifying this burden in terms of years of life lost.
8.2.2 Wind, storms and floods
Floods are low-probability, high-impact events that can overwhelm physical infrastructure, human resilience and social organisation. Floods are the most frequent natural weather disaster ( EM-DAT, 2006 [NPR] ). Floods result from the interaction of rainfall, surface runoff, evaporation, wind, sea level and local topography. In inland areas, flood regimes vary substantially depending on catchment size, topography and climate. Water management practices, urbanisation, intensified land use and forestry can substantially alter the risks of floods ( EEA, 2005 [NPR] ). Windstorms are often associated with floods.
Major storm and flood disasters have occurred in the last two decades. In 2003, 130 million people were affected by floods in China ( EM-DAT, 2006 [NPR] ). In 1999, 30,000 died from storms followed by floods and landslides in Venezuela. In 2000 / 2001, 1,813 died in floods in Mozambique ( IFRC, 2002 [NPR] ; Guha-Sapir et al., 2004 [NPR] ). Improved structural and non-structural measures, particularly improved warnings, have decreased mortality from floods and storm surges in the last 30 years ( EEA, 2005 [NPR] ); however, the impact of weather disasters in terms of social and health effects is still considerable and is unequally distributed (see Box 8.2 ). Flood health impacts range from deaths, injuries, infectious diseases and toxic contamination, to mental health problems ( (Greenough et al., 2001; ) ( Ahern et al., 2005 ) ).
Box 8.2. Gender and natural disasters
Men and women are affected differently in all phases of a disaster, from exposure to risk and risk perception; to preparedness behaviour, warning communication and response; physical, psychological, social and economic impacts; emergency response; and ultimately to recovery and reconstruction ( Fothergill, 1998 [NPR] ). Natural disasters have been shown to result in increased domestic violence against, and post-traumatic stress disorders in, women ( (Anderson and Manuel, 1994; ) ( Garrison et al., 1995; ) Wilson et al., 1998 [NPR] ; Ariyabandu and Wickramasinghe, 2003 [NPR] ;( Galea et al., 2005 ) ). Women make an important contribution to disaster reduction, often informally through participating in disaster management and acting as agents of social change. Their resilience and their networks are critical in household and community recovery (Enarson and Morrow, 1998 [NotFound] ; Ariyabandu and Wickramasinghe, 2003 [NPR] ). After the 1999 Orissa cyclone, most of the relief efforts were targeted at or through women, giving them control over resources. Women received the relief kits, including house-building grants and loans, resulting in improved self-esteem and social status ( Briceño, 2002 [NPR] ). Similarly, following a disastrous 1992 flood in Pakistan in the Sarghoda district, women were involved in the reconstruction design and were given joint ownership of the homes, promoting their empowerment.
In terms of deaths and populations affected, floods and tropical cyclones have the greatest impact in South Asia and Latin America ( Guha-Sapir et al., 2004 [NPR] ;( Schultz et al., 2005 ) ). Deaths recorded in disaster databases are from drowning and severe injuries. Deaths from unsafe or unhealthy conditions following the extreme event are also a health consequence, but such information is rarely included in disaster statistics ( (Combs et al., 1998; ) ( Jonkman and Kelman, 2005 ) ). Drowning by storm surge is the major killer in coastal storms where there are large numbers of deaths. An assessment of surges in the past 100 years found that major events were confined to a limited number of regions, with many events occurring in the Bay of Bengal, particularly Bangladesh ( Nicholls, 2003 [NPR, ARC] ).
Populations with poor sanitation infrastructure and high burdens of infectious disease often experience increased rates of diarrhoeal diseases after flood events. Increases in cholera ( (Sur et al., 2000; ) ( Gabastou et al., 2002 ) ), cryptosporidiosis ( (Katsumata et al., 1998 ) ) and typhoid fever ( (Vollaard et al., 2004 ) ) have been reported in low- and middle-income countries. Flood-related increases in diarrhoeal disease have also been reported in India ( (Mondal et al., 2001 ) ), Brazil ( (Heller et al., 2003 ) ) and Bangladesh ( (Kunii et al., 2002; ) ( Schwartz et al., 2006 ) ). The floods in Mozambique in 2001 were estimated to have caused over 8,000 additional cases and 447 deaths from diarrhoeal disease in the following months ( Cairncross and Alvarinho, 2006 [NPR, MoS, ARC] ).
The risk of infectious disease following flooding in high-income countries is generally low, although increases in respiratory and diarrhoeal diseases have been reported after floods ( (Miettinen et al., 2001; ) ( Reacher et al., 2004; ) ( Wade et al., 2004 ) ). An important exception was the impact of Hurricanes Katrina and Rita in the USA in 2005, where contamination of water supplies with faecal bacteria led to many cases of diarrhoeal illness and some deaths ( (CDC, 2005; ) ( Manuel, 2006 ) ).
Flooding may lead to contamination of waters with dangerous chemicals, heavy metals or other hazardous substances, from storage or from chemicals already in the environment (e.g., pesticides). Chemical contamination following Hurricane Katrina in the USA included oil spills from refineries and storage tanks, pesticides, metals and hazardous waste ( (Manuel, 2006 ) ). Concentrations of most contaminants were within acceptable short-term levels, except for lead and volatile organic compounds (VOCs) in some areas ( (Pardue et al., 2005 ) ). There are also health risks associated with long-term contamination of soil and sediment ( (Manuel, 2006 ) ); however, there is little published evidence demonstrating a causal effect of chemical contamination on the pattern of morbidity and mortality following flooding events ( (Euripidou and Murray, 2004; ) ( Ahern et al., 2005 ) ). Increases in population density and accelerating industrial development in areas subject to natural disasters increase the probability of future disasters and the potential for mass human exposure to hazardous materials released during disasters ( (Young et al., 2004 ) ).
There is increasing evidence of the importance of mental disorders as an impact of disasters ( (Mollica et al., 2004; ) ( Ahern et al., 2005 ) ). Prolonged impairment resulting from common mental disorders (anxiety and depression) may be considerable. Studies in both low- and high-income countries indicate that the mental-health aspect of flood-related impacts has been insufficiently investigated ( (Ko et al., 1999; ) ( Ohl and Tapsell, 2000; ) ( Bokszczanin, 2002; ) ( Tapsell et al., 2002; ) Assan-arigkornchai et al., 2004; ( Norris et al., 2004; ) ( North et al., 2004; ) ( Ahern et al., 2005; ) ( Kohn et al., 2005; ) ( Maltais et al., 2005 ) ). A systematic review of post-traumatic stress disorder in high-income countries found a small but significant effect following disasters ( (Galea et al., 2005 ) ). There is also evidence of medium- to long-term impacts on behavioural disorders in young children ( (Durkin et al., 1993; ) ( Becht et al., 1998; ) ( Bokszczanin, 2000, ) 2002 ).
Vulnerability to weather disasters depends on the attributes of the person at risk (including where they live, age, income, education and disability) and on broader social and environmental factors (level of disaster preparedness, health sector responses and environmental degradation) ( Blaikie et al., 1994 [NPR] ; Menne, 2000 [NPR, SRC] ; Olmos, 2001 [NPR] ; Adger et al., 2005 [JoC, ARC] ; Few and Matthies, 2006 [NPR, MoS] ). Poorer communities, particularly slum dwellers, are more likely to live in flood-prone areas. In the USA, lower-income groups were most affected by Hurricane Katrina, and low-income schools had twice the risk of being flooded compared with the reference group ( (Guidry and Margolis, 2005 ) ).
High-density populations in low-lying coastal regions experience a high health burden from weather disasters, such as settlements along the North Sea coast in north-west Europe, the Seychelles, parts of Micronesia, the Gulf Coast of the USA and Mexico, the Nile Delta, the Gulf of Guinea, and the Bay of Bengal (see Chapter 6 ). Environmentally degraded areas are particularly vulnerable to tropical cyclones and coastal flooding under current climate conditions.
8.2.3 Drought, nutrition and food security
The causal chains through which climate variability and extreme weather influence human nutrition are complex and involve different pathways (regional water scarcity, salinisation of agricultural lands, destruction of crops through flood events, disruption of food logistics through disasters, and increased burden of plant infectious diseases or pests) (see Chapter 5 ). Both acute and chronic nutritional problems are associated with climate variability and change. The effects of drought on health include deaths, malnutrition (undernutrition, protein-energy malnutrition and/or micronutrient deficiencies), infectious diseases and respiratory diseases ( Menne and Bertollini, 2000 [SRC] ).
Drought diminishes dietary diversity and reduces overall food consumption, and may therefore lead to micronutrient deficiencies. In Gujarat, India, during a drought in the year 2000, diets were found to be deficient in energy and several vitamins. In this population, serious effects of drought on anthropometric indices may have been prevented by public-health measures ( (Hari Kumar et al., 2005 ) ). A study in southern Africa suggests that HIV/AIDS amplifies the effect of drought on nutrition ( (Mason et al., 2005 ) ). Malnutrition increases the risk both of acquiring and of dying from an infectious disease. A study in Bangladesh found that drought and lack of food were associated with an increased risk of mortality from a diarrhoeal illness ( Aziz et al., 1990 [NPR, ARC] ).
Drought and the consequent loss of livelihoods is also a major trigger for population movements, particularly rural to urban migration. Population displacement can lead to increases in communicable diseases and poor nutritional status resulting from overcrowding, and a lack of safe water, food and shelter ( (Choudhury and Bhuiya, 1993; ) Menne and Bertollini, 2000 [SRC] ;( del Ninno and Lundberg, 2005 ) ). Recently, rural to urban migration has been implicated as a driver of HIV transmission ( (White, 2003; ) ( Coffee et al., 2005 ) ). Farmers in Australia also appear to be at increased risk of suicide during periods of drought ( (Nicholls et al., 2005 ) ). The range of health impacts associated with a drought event in Brazil are described in Box 8.3 .
Box 8.3. Drought in the Amazon
In the dry season of 2005, an intense drought affected the western and central part of the Amazon region, especially Bolivia, Peru and Brazil. In Brazil alone, 280,000 to 300,000 people were affected (see, e.g., Folha, 2006; Socioambiental, 2006 ). The drought was unusual because it was not caused by an El Niño event, but was linked to a circulation pattern powered by warm seas in the Atlantic – the same phenomenon responsible for the intense Atlantic hurricane season ( CPTEC, 2005 [NPR] ). There were increased risks to health due to water scarcity, food shortages and smoke from forest fires. Most affected were rural dwellers and riverine traditional subsistence farmers with limited spare resources to mobilise in an emergency. The local and national governments in Brazil provided financial assistance for the provision of safe drinking water, food supplies, medicines and transportation to thousands of people isolated in their communities due to rivers drying up (World Bank, 2005 [NPR] ).
8.2.3.1 Drought and infectious disease
Countries within the ‘Meningitis Belt’ in semi-arid sub-Saharan Africa experience the highest endemicity and epidemic frequency of meningococcal meningitis in Africa, although other areas in the Rift Valley, the Great Lakes, and southern Africa are also affected. The spatial distribution, intensity and seasonality of meningococcal (epidemic) meningitis appear to be strongly linked to climatic and environmental factors, particularly drought, although the causal mechanism is not clearly understood ( Molesworth et al., 2001 [NPR, SRC] , 2002a, b, 2003 ). Climate plays an important part in the interannual variability in transmission, including the timing of the seasonal onset of the disease ( Molesworth et al., 2001 [NPR, SRC] ;( Sultan et al., 2005 ) ). The geographical distribution of meningitis has expanded in West Africa in recent years, which may be attributable to environmental change driven by both changes in land use and regional climate change ( Molesworth et al., 2003 [SRC] ).
The transmission of some mosquito-borne diseases is affected by drought events. During droughts, mosquito activity is reduced and, as a consequence, the population of non-immune persons increases. When the drought breaks, there is a much larger proportion of susceptible hosts to become infected, thus potentially increasing transmission ( (Bouma and Dye, 1997; ) Woodruff et al., 2002 [MoS, SRC] ). In other areas, droughts may favour increases in mosquito populations due to reductions in mosquito predators ( (Chase and Knight, 2003 ) ). Other drought-related factors that may result in a short-term increase in the risk for infectious disease outbreaks include stagnation and contamination of drainage canals and small rivers. In the long term, the incidence of mosquito-borne diseases such as malaria decreases because the mosquito vector lacks the necessary humidity and water for breeding. The northern limit of Plasmodium falciparum malaria in Africa is the Sahel, where rainfall is an important limiting factor in disease transmission ( (Ndiaye et al., 2001 ) ). Malaria has decreased in association with long-term decreases in annual rainfall in Senegal and Niger ( (Mouchet et al., 1996; ) ( Julvez et al., 1997 ) ). Drought events are also associated with dust storms and respiratory health effects (see Section 8.2.6 ). Droughts are also associated with water scarcity; the risks of water-washed diseases are addressed in Section 8.2.5 .
8.2.4 Food safety
Several studies have confirmed and quantified the effects of high temperatures on common forms of food poisoning, such as salmonellosis ( (D’Souza et al., 2004; ) Kovats et al., 2004 [SRC] ;( Fleury et al., 2006 ) ). These studies found an approximately linear increase in reported cases with each degree increase in weekly or monthly temperature. Temperature is much less important for the transmission of Campylobacter ( Kovats et al., 2005 [Ambiguous] ;( Louis et al., 2005; ) ( Tam et al., 2006 ) ).
Contact between food and pest species, especially flies, rodents and cockroaches, is also temperature-sensitive. Fly activity is largely driven by temperature rather than by biotic factors ( Goulson et al., 2005 [MoS] ). In temperate countries, warmer weather and milder winters are likely to increase the abundance of flies and other pest species during the summer months, with the pests appearing earlier in spring.
Harmful algal blooms (HABs) (see Chapter 1 , Section 1.3.4.2 ) produce toxins that can cause human diseases, mainly via consumption of contaminated shellfish. Warmer seas may thus contribute to increased cases of human shellfish and reef-fish poisoning (ciguatera) and poleward expansions of these disease distributions ( (Kohler and Kohler, 1992; ) ( Lehane and Lewis, 2000; ) ( Hall et al., 2002; ) ( Hunter, 2003; ) Korenberg, 2004 [NPR] ). For example, sea-surface temperatures influence the growth of Gambierdiscus spp., which is associated with reports of ciguatera in French Polynesia ( (Chateau-Degat et al., 2005 ) ). No further assessments of the impact of climate change on shellfish poisoning have been carried out since the TAR.
Vibrio parahaemolyticus and Vibrio vulnificus are responsible for non-viral infections related to shellfish consumption in the USA, Japan and South-East Asia ( (Wittmann and Flick, 1995; ) ( Tuyet et al., 2002 ) ). Abundance is dependent on the salinity and temperature of the coastal water. A large outbreak in 2004 due to the consumption of contaminated oysters (V. parahaemolyticus) was linked to atypically high temperatures in Alaskan coastal waters ( (McLaughlin et al., 2005 ) ).
Another example of the implications that climate change can have for food safety is the methylation of mercury and its subsequent uptake by fish and human beings, as observed in the Faroe Islands ( (Booth and Zeller, 2005; ) McMichael et al., 2006 [MoS, SRC] ).
8.2.5 Water and disease
Climate-change-related alterations in rainfall, surface water availability and water quality could affect the burden of water-related diseases (see Chapter 3 ). Water-related diseases can be classified by route of transmission, thus distinguishing between water-borne (ingested) and water-washed diseases (caused by lack of hygiene). There are four main considerations to take into account when evaluating the relationship between health outcomes and exposure to changes in rainfall, water availability and quality:
- linkages between water availability, household access to improved water, and the health burden due to diarrhoeal diseases;
- the role of extreme rainfall (intense rainfall or drought) in facilitating water-borne outbreaks of diseases through piped water supplies or surface water;
- effects of temperature and runoff on microbiological and chemical contamination of coastal, recreational and surface waters;
- direct effects of temperature on the incidence of diarrhoeal disease.
Access to safe water remains an extremely important global health issue. More than 2 billion people live in the dry regions of the world and suffer disproportionately from malnutrition, infant mortality and diseases related to contaminated or insufficient water ( WHO, 2005 [NPR] ). A small and unquantified proportion of this burden can be attributed to climate variability or climate extremes. The effect of water scarcity on food availability and malnutrition is discussed in Section 8.2.3 , and the effect of rainfall on outbreaks of mosquito-borne and rodent-borne disease is discussed in Section 8.2.8 .
Childhood mortality due to diarrhoea in low-income countries, especially in sub-Saharan Africa, remains high despite improvements in care and the use of oral rehydration therapy ( Kosek et al., 2003 [MoS] ). Children may survive the acute illness but may later die due to persistent diarrhoea or malnutrition. Children in poor rural and urban slum areas are at high risk of diarrhoeal disease mortality and morbidity. Several studies have shown that transmission of enteric pathogens is higher during the rainy season ( (Nchito et al., 1998; ) ( Kang et al., 2001 ) ). Drainage and storm water management is important in low-income urban communities, as blocked drains are one of the causes of increased disease transmission ( (Parkinson and Butler, 2005 ) ).
Climate extremes cause both physical and managerial stresses on water supply systems (see Chapters 3 and 7 ), although well-managed public water supply systems should be able to cope with climate extremes ( Nicholls, 2003 [NPR, ARC] ; Wilby et al., 2005 [ARC] ). Reductions in rainfall lead to low river flows, reducing effluent dilution and leading to increased pathogen loading. This could represent an increased challenge to water-treatment plants. During the dry summer of 2003, low flows of rivers in the Netherlands resulted in apparent changes in water quality ( (Senhorst and Zwolsman, 2005 ) ).
Extreme rainfall and runoff events may increase the total microbial load in watercourses and drinking-water reservoirs ( (Kistemann et al., 2002 ) ), although the linkage to cases of human disease is less certain ( (Schwartz and Levin, 1999; ) Aramini et al., 2000 [NPR] ;( Schwartz et al., 2000; ) Lim et al., 2002 [NPR] ). A study in the USA found an association between extreme rainfall events and monthly reports of outbreaks of water-borne disease ( Curriero et al., 2001 [ARC] ). The seasonal contamination of surface water in early spring in North America and Europe may explain some of the seasonality in sporadic cases of water-borne diseases such as cryptosporidiosis and campylobacteriosis ( (Clark et al., 2003; ) ( Lake et al., 2005 ) ). The marked seasonality of cholera outbreaks in the Amazon is associated with low river flow in the dry season ( (Gerolomo and Penna, 1999 ) ), probably due to pathogen concentrations in pools.
Higher temperature was found to be strongly associated with increased episodes of diarrhoeal disease in adults and children in Peru ( Checkley et al., 2000 [ARC] ; Speelmon et al., 2000 [ARC] ; Checkley et al., 2004 [ARC] ;( Lama et al., 2004 ) ). Associations between monthly temperature and diarrhoeal episodes have also been reported in the Pacific islands, Australia and Israel ( Singh et al., 2001 [SRC] ; McMichael et al., 2003b [NPR, SRC] ;( Vasilev, 2003 ) ).
Although there is evidence that the bimodal seasonal pattern of cholera in Bangladesh is correlated with sea-surface temperatures in the Bay of Bengal and with seasonal plankton abundance (a possible environmental reservoir of the cholera pathogen, Vibrio cholerae) ( Colwell, 1996 [JoC] ;( Bouma and Pascual, 2001 ) ), winter peaks in disease further inland are not associated with sea-surface temperatures ( (Bouma and Pascual, 2001 ) ). In many countries cholera transmission is primarily associated with poor sanitation. The effect of sea-surface temperatures in cholera transmission has been most studied in the Bay of Bengal ( Pascual et al., 2000 [JoC, ARC] ; Lipp et al., 2002 [MoS] ; Rodo et al., 2002 [JoC, ARC] ; Koelle et al., 2005 [JoC, MoS, ARC] ). In sub-Saharan Africa, cholera outbreaks are often associated with flood events and faecal contamination of the water supplies.
8.2.6 Air quality and disease
Weather at all time scales determines the development, transport, dispersion and deposition of air pollutants, with the passage of fronts, cyclonic and anticyclonic systems and their associated air masses being of particular importance. Air-pollution episodes are often associated with stationary or slowly migrating anticyclonic or high pressure systems, which reduce pollution dispersion and diffusion ( (Schichtel and Husar, 2001; ) ( Rao et al., 2003 ) ). Airflow along the flanks of anticyclonic systems can transport ozone precursors, creating the conditions for an ozone event ( (Lennartson and Schwartz, 1999; ) Scott and Diab, 2000 [MoS] ; Yarnal et al., 2001 [JoC] ;( Tanner and Law, 2002 ) ). Certain weather patterns enhance the development of the urban heat island, the intensity of which may be important for secondary chemical reactions within the urban atmosphere, leading to elevated levels of some pollutants ( Morris and Simmonds, 2000 [JoC] ;( Junk et al., 2003; ) ( Jonsson et al., 2004 ) ).
8.2.6.1 Ground-level ozone
Ground-level ozone is both naturally occurring and, as the primary constituent of urban smog, is also a secondary pollutant formed through photochemical reactions involving nitrogen oxides and volatile organic compounds in the presence of bright sunshine with high temperatures. In urban areas, transport vehicles are the key sources of nitrogen oxides and volatile organic compounds. Temperature, wind, solar radiation, atmospheric moisture, venting and mixing affect both the emissions of ozone precursors and the production of ozone ( (Nilsson et al., 2001a, ) b; ( Mott et al., 2005 ) ). Because ozone formation depends on sunlight, concentrations are typically highest during the summer months, although not all cities have shown seasonality in ozone concentrations ( (Bates, 2005 ) ). Concentrations of ground-level ozone are increasing in most regions ( (Wu and Chan, 2001; ) ( Chen et al., 2004 ) ).
Exposure to elevated concentrations of ozone is associated with increased hospital admissions for pneumonia, chronic obstructive pulmonary disease, asthma, allergic rhinitis and other respiratory diseases, and with premature mortality (e.g., ( Mudway and Kelly, 2000; ) ( Gryparis et al., 2004; ) ( Bell et al., 2005, ) 2006; ( Ito et al., 2005; ) ( Levy et al., 2005 ) ). Outdoor ozone concentrations, activity patterns and housing characteristics, such as the extent of insulation, are the primary determinants of ozone exposure ( (Suh et al., 2000; ) ( Levy et al., 2005 ) ). Although a considerable amount is known about the health effects of ozone in Europe and North America, few studies have been conducted in other regions.
8.2.6.2 Effects of weather on concentrations of other air pollutants
Concentrations of air pollutants in general, and fine particulate matter (PM) in particular, may change in response to climate change because their formation depends, in part, on temperature and humidity. Air-pollution concentrations are the result of interactions between variations in the physical and dynamic properties of the atmosphere on time-scales from hours to days, atmospheric circulation features, wind, topography and energy use ( McGregor, 1999 [NPR, SRC] ; Hartley and Robinson, 2000 [JoC] ;( Pal Arya, 2000 ) ). Some air pollutants demonstrate weather-related seasonal cycles ( (Alvarez et al., 2000; ) ( Kassomenos et al., 2001; ) ( Hazenkamp-von Arx et al., 2003; ) ( Nagendra and Khare, 2003; ) ( Eiguren-Fernandez et al., 2004 ) ). Some locations, such as Mexico City and Los Angeles, are predisposed to poor air quality because local weather patterns are conducive to chemical reactions leading to the transformation of emissions, and because the topography restricts the dispersion of pollutants ( (Rappengluck et al., 2000; ) Kossmann and Sturman, 2004 [JoC] ).
Evidence for the health impacts of PM is stronger than that for ozone. PM is known to affect morbidity and mortality (e.g., ( Ibald-Mulli et al., 2002; ) ( Pope et al., 2002; ) ( Kappos et al., 2004; ) ( Dominici et al., 2006 ) ), so increasing concentrations would have significant negative health impacts.
8.2.6.3 Air pollutants from forest fires
In some regions, changes in temperature and precipitation are projected to increase the frequency and severity of fire events (see Chapter 5 ). Forest and bush fires cause burns, damage from smoke inhalation and other injuries. Large fires are also accompanied by an increased number of patients seeking emergency services ( (Hoyt and Gerhart, 2004 ) ). Toxic gaseous and particulate air pollutants are released into the atmosphere, which can significantly contribute to acute and chronic illnesses of the respiratory system, particularly in children, including pneumonia, upper respiratory diseases, asthma and chronic obstructive pulmonary diseases ( WHO, 2002a [NPR] ;( Bowman and Johnston, 2005; ) Moore et al., 2006 [MoS] ). For example, the 1997 Indonesia fires increased hospital admissions and mortality from cardiovascular and respiratory diseases, and negatively affected activities of daily living in South-East Asia ( (Sastry, 2002; ) ( Frankenberg et al., 2005; ) ( Mott et al., 2005 ) ). Pollutants from forest fires can affect air quality for thousands of kilometres ( (Sapkota et al., 2005 ) ).
Windblown dust originating in desert regions of Africa, Mongolia, Central Asia and China can affect air quality and population health in remote areas. When compared with non-dust weather conditions, dust can carry large concentrations of respirable particles, trace elements that can affect human health, fungal spores and bacteria ( (Claiborn et al., 2000; ) ( Fan et al., 2002; ) ( Shinn et al., 2003; ) ( Cook et al., 2005; ) ( Prospero et al., 2005; ) ( Xie et al., 2005; ) ( Kellogg and Griffin, 2006 ) ). However, recent studies have not found statistically significant associations between Asian dust storms and hospital admissions in Canada and Taiwan ( (Chen and Tang, 2005; ) ( Yang et al., 2005a; ) ( Bennett et al., 2006 ) ). Evidence suggests that local mortality, particularly from cardiovascular and respiratory diseases, is increased in the days following a dust storm ( (Kwon et al., 2002; ) ( Chen et al., 2004 ) ).
8.2.6.4 Long-range transport of air pollutants
Changes in wind patterns and increased desertification may increase the long-range transport of air pollutants. Under certain atmospheric circulation conditions, the transport of pollutants, including aerosols, carbon monoxide, ozone, desert dust, mould spores and pesticides, may occur over large distances and over time-scales typically of 4-6 days, which can lead to adverse health impacts ( (Gangoiti et al., 2001; ) Stohl et al., 2001 [MoS] ;( Buchanan et al., 2002; ) ( Chan et al., 2002; ) ( Martin et al., 2002; ) ( Ryall et al., 2002; ) ( Ansmann et al., 2003; ) ( He et al., 2003; ) Helmis et al., 2003 [JoC, MoS] ;( Moore et al., 2003; ) ( Shinn et al., 2003; ) ( Unsworth et al., 2003; ) ( Kato et al., 2004; ) ( Liang et al., 2004; ) ( Tu et al., 2004 ) ). Sources of such pollutants include biomass burning, as well as industrial and mobile sources ( Murano et al., 2000 [MoS] ;( Koe et al., 2001; ) ( Jaffe et al., 2003, ) 2004; ( Moore et al., 2003 ) ).
8.2.7 Aeroallergens and disease
Climate change has caused an earlier onset of the spring pollen season in the Northern Hemisphere (see Chapter 1 , Section 1.3.7.4 ( D’Amato et al., 2002; ) ( Weber, 2002; ) Beggs, 2004 [MoS, SRC] ). It is reasonable to conclude that allergenic diseases caused by pollen, such as allergic rhinitis, have experienced some concomitant change in seasonality ( (Emberlin et al., 2002; ) ( Burr et al., 2003 ) ). There is limited evidence that the length of the pollen season has also increased for some species. Although there are suggestions that the abundance of a few species of air-borne pollens has increased due to climate change, it is unclear whether the allergenic content of these pollen types has changed (pollen content remaining the same or increasing would imply increased exposure) ( Huynen and Menne, 2003 [NPR, SRC] ; Beggs and Bambrick, 2005 [SRC] ). Few studies show patterns of increasing exposure for allergenic mould spores or bacteria ( (Corden et al., 2003; ) ( Harrison et al., 2005 ) ). Changes in the spatial distribution of natural vegetation, such as the introduction of new aeroallergens into an area, increases sensitisation ( (Voltolini et al., 2000; ) Asero, 2002 [MoS] ). The introduction of new invasive plant species with highly allergenic pollen, in particular ragweed (Ambrosia artemisiifolia), presents important health risks; ragweed is spreading in several parts of the world ( (Rybnicek and Jaeger, 2001; ) Huynen and Menne, 2003 [NPR, SRC] ; Taramarcaz et al., 2005 [SRC] ;( Cecchi et al., 2006 ) ). Several laboratory studies show that increasing CO2 concentrations and temperatures increase ragweed pollen production and prolong the ragweed pollen season ( (Wan et al., 2002; ) ( Wayne et al., 2002; ) ( Singer et al., 2005; ) Ziska et al., 2005 [JoC] ;( Rogers et al., 2006a ) ) and increase some plant metabolites that can affect human health ( Ziska et al., 2005 [JoC] ; Mohan et al., 2006 [JoC] ).
8.2.8 Vector-borne, rodent-borne and other infectious diseases
Vector-borne diseases (VBD) are infections transmitted by the bite of infected arthropod species, such as mosquitoes, ticks, triatomine bugs, sandflies and blackflies. VBDs are among the most well-studied of the diseases associated with climate change, due to their widespread occurrence and sensitivity to climatic factors. There is some evidence of climate-change-related shifts in the distribution of tick vectors of disease, of some (non-malarial) mosquito vectors in Europe and North America, and in the phenology of bird reservoirs of pathogens (see Chapter 1 and Box 8.4 ).
Box 8.4. Climate change, migratory birds and infectious diseases
Several species of wild birds can act as biological or mechanical carriers of human pathogens as well as of vectors of infectious agents ( (Olsen et al., 1995; ) ( Klich et al., 1996; ) Gylfe et al., 2000 [JoC] ;( Friend et al., 2001; ) ( Pereira et al., 2001; ) ( Broman et al., 2002; ) ( Moore et al., 2002; ) ( Niskanen et al., 2003; ) ( Rappole and Hubalek, 2003; ) ( Reed et al., 2003; ) ( Fallacara et al., 2004; ) ( Hubalek, 2004; ) ( Krauss et al., 2004 ) ). Many of these birds are migratory species that seasonally fly long distances through different continents ( de Graaf and Rappole, 1995 [NPR] ;( Webster et al., 2002b ) ). Climate change has been implicated in changes in the migratory and reproductive phenology (advancement in breeding and migration dates) of several bird species, their abundance and population dynamics, as well as a northward expansion of their geographical range in Europe ( Sillett et al., 2000 [JoC] ; Barbraud and Weimerskirch, 2001 [JoC] ; Parmesan and Yohe, 2003 [JoC, ARC] ;( Brommer, 2004; ) ( Visser et al., 2004; ) Both and Visser, 2005 [JoC] ). Two possible consequences of these phenological changes in birds to the dispersion of pathogens and their vectors are:
1. shifts in the geographical distribution of the vectors and pathogens due to altered distributions or changed migratory patterns of bird populations;
2. changes in the life cycles of bird-associated pathogens due to the mistiming between bird breeding and the breeding of vectors, such as mosquitoes. One example is the transmission of St. Louis encephalitis virus, which depends on meteorological triggers (e.g., precipitation) to bring the pathogen, vector and host (nestlings) cycles into synchrony, allowing an overlap that initiates and facilitates the cycling necessary for virus amplification between mosquitoes and wild birds ( Day, 2001 [MoS] ).
Northern or altitudinal shifts in tick distribution have been observed in Sweden ( Lindgren and Talleklint, 2000 [NPR] ;( Lindgren and Gustafson, 2001 ) ) and Canada ( (Barker and Lindsay, 2000 ) ), and altitudinal shifts have been observed in the Czech Republic ( (Daniel et al., 2004 ) ). Geographical changes in tick-borne infections have been observed in Denmark ( (Skarphedinsson et al., 2005 ) ). Climate change alone is unlikely to explain recent increases in the incidence of tick-borne diseases in Europe or North America. There is considerable spatial heterogeneity in the degree of increase of tick-borne encephalitis, for example, within regions of Europe likely to have experienced similar levels of climate change ( Patz, 2002 [JoC, ARC] ;( Randolph, 2004; ) ( Sumilo et al., 2006 ) ). Other explanations cannot be ruled out, e.g., human impacts on the landscape, increasing both the habitat and wildlife hosts of ticks, and changes in human behaviour that may increase human contact with infected ticks ( (Randolph, 2001 ) ).
In north-eastern North America, there is evidence of recent micro-evolutionary (genetic) responses of the mosquito species Wyeomyia smithii to increased average land surface temperatures and earlier arrival of spring in the past two decades ( Bradshaw and Holzapfel, 2001 [JoC] ). Although not a vector of human disease, this species is closely related to important arbovirus vector species that may be undergoing similar evolutionary changes.
Cutaneous leishmaniasis has been reported in dogs (reservoir hosts) further north in Europe, although the possibility of previous under-reporting cannot be excluded ( Lindgren and Naucke, 2006 [NPR] ). Changes in the geographical distribution of the sandfly vector have been reported in southern Europe ( (Aransay et al., 2004; ) ( Afonso et al., 2005 ) ). However, no study has investigated the causes of these changes. The re-emergence of kala-azar (visceral leishmaniasis) in cities of the semi-arid Brazilian north-eastern region in the early 1980 s and 1990 s was caused by rural–urban migration of subsistence farmers who had lost their crops due to prolonged droughts ( (Franke et al., 2002; ) Confalonieri, 2003 [SRC] ).
8.2.8.1 Dengue
Dengue is the world’s most important vector-borne viral disease. Several studies have reported associations between spatial ( Hales et al., 2002 [MoS, SRC] ), temporal ( Hales et al., 1999 [SRC] ;( Corwin et al., 2001; ) ( Gagnon et al., 2001 ) ) or spatiotemporal patterns of dengue and climate ( Hales et al., 1999 [SRC] ;( Corwin et al., 2001; ) ( Gagnon et al., 2001; ) Cazelles et al., 2005 [SRC] ). However, these reported associations are not entirely consistent, possibly reflecting the complexity of climatic effects on transmission, and/or the presence of competing factors ( Cummings, 2004 [JoC] ). While high rainfall or high temperature can lead to an increase in transmission, studies have shown that drought can also be a cause if household water storage increases the number of suitable mosquito breeding sites ( (Pontes et al., 2000; ) ( Depradine and Lovell, 2004; ) ( Guang et al., 2005 ) ).
Climate-based (temperature, rainfall, cloud cover) density maps of the main dengue vector Stegomyia (previously called Aedes) aegypti are a good match with the observed disease distribution ( (Hopp and Foley, 2003 ) ). The model of vector abundance has good agreement with the distribution of reported cases of dengue in Colombia, Haiti, Honduras, Indonesia, Thailand and Vietnam ( (Hopp and Foley, 2003 ) ). Approximately one-third of the world’s population lives in regions where the climate is suitable for dengue transmission ( Hales et al., 2002 [MoS, SRC] ;( Rogers et al., 2006b ) ).
8.2.8.2 Malaria
The spatial distribution, intensity of transmission, and seasonality of malaria is influenced by climate in sub-Saharan Africa; socio-economic development has had only limited impact on curtailing disease distribution ( (Hay et al., 2002a; ) ( Craig et al., 2004 ) ).
Rainfall can be a limiting factor for mosquito populations and there is some evidence of reductions in transmission associated with decadal decreases in rainfall. Interannual malaria variability is climate-related in specific eco-epidemiological zones ( (Julvez et al., 1992; ) ( Ndiaye et al., 2001; ) ( Singh and Sharma, 2002; ) ( Bouma, 2003; ) Thomson et al., 2005 [SRC] ). A systematic review of studies of the El Niño-Southern Oscillation (ENSO) and malaria concluded that the impact of El Niño on the risk of malaria epidemics is well established in parts of southern Asia and South America ( (Kovats et al., 2003 ) ). Evidence of the predictability of unusually high or low malaria anomalies from both sea-surface temperature ( Thomson et al., 2005 [SRC] ) and multi-model ensemble seasonal climate forecasts in Botswana ( Thomson et al., 2006 [JoC, MoS, SRC] ) supports the practical and routine use of seasonal forecasts for malaria control in southern Africa (DaSilva et al., 2004 ).
The effects of observed climate change on the geographical distribution of malaria and its transmission intensity in highland regions remains controversial. Analyses of time-series data in some sites in East Africa indicate that malaria incidence has increased in the apparent absence of climate trends ( (Hay et al., 2002a, ) b; ( Shanks et al., 2002 ) ). The proposed driving forces behind the malaria resurgence include drug resistance of the malaria parasite and a decrease in vector control activities. However, the validity of this conclusion has been questioned because it may have resulted from inappropriate use of the climatic data ( Patz, 2002 [JoC, ARC] ). Analysis of updated temperature data for these regions has found a significant warming trend since the end of the 1970 s, with the magnitude of the change affecting transmission potential ( Pascual et al., 2006 [JoC, ARC] ). In southern Africa, long-term trends for malaria were not significantly associated with climate, although seasonal changes in case numbers were significantly associated with a number of climatic variables ( (Craig et al., 2004 ) ). Drug resistance and HIV infection were associated with long-term malaria trends in the same area ( (Craig et al., 2004 ) ).
A number of further studies have reported associations between interannual variability in temperature and malaria transmission in the African highlands. An analysis of de-trended time-series malaria data in Madagascar indicated that minimum temperature at the start of the transmission season, corresponding to the months when the human–vector contact is greatest, accounts for most of the variability between years ( (Bouma, 2003 ) ). In highland areas of Kenya, malaria admissions have been associated with rainfall and unusually high maximum temperatures 3-4 months previously ( Githeko and Ndegwa, 2001 [MoS, ARC] ). An analysis of malaria morbidity data for the period from the late 1980 s until the early 1990 s from 50 sites across Ethiopia found that epidemics were associated with high minimum temperatures in the preceding months ( Abeku et al., 2003 [SRC] ). An analysis of data from seven highland sites in East Africa reported that short-term climate variability played a more important role than long-term trends in initiating malaria epidemics ( Zhou et al., 2004 [JoC, ARC] , 2005 ), although the method used to test this hypothesis has been challenged ( (Hay et al., 2005b ) ).
There is no clear evidence that malaria has been affected by climate change in South America ( (Benitez et al., 2004 ) ) (see Chapter 1 ) or in continental regions of the Russian Federation ( Semenov et al., 2002 [ARC] ). The attribution of changes in human diseases to climate change must first take into account the considerable changes in reporting, surveillance, disease control measures, population changes, and other factors such as land-use change ( Kovats et al., 2001 [SRC] ;( Rogers and Randolph, 2006 ) ).
Despite the known causal links between climate and malaria transmission dynamics, there is still much uncertainty about the potential impact of climate change on malaria at local and global scales (see also Section 8.4.1 ) because of the paucity of concurrent detailed historical observations of climate and malaria, the complexity of malaria disease dynamics, and the importance of non-climatic factors, including socio-economic development, immunity and drug resistance, in determining infection and infection outcomes. Given the large populations living in highland areas of East Africa, the limitations of the analyses conducted, and the significant health risks of epidemic malaria, further research is warranted.
8.2.8.3 Other infectious diseases
Recent investigations of plague foci in North America and Asia with respect to the relationships between climatic variables, human disease cases ( Enscore et al., 2002 [MoS] ) and animal reservoirs ( (Stapp et al., 2004; ) Stenseth, 2006 [JoC] ) have suggested that temporal variations in plague risk can be estimated by monitoring key climatic variables.
There is good evidence that diseases transmitted by rodents sometimes increase during heavy rainfall and flooding because of altered patterns of human–pathogen–rodent contact. There have been reports of flood-associated outbreaks of leptospirosis (Weil’s diseases) from a wide range of countries in Central and South America and South Asia ( (Ko et al., 1999; ) ( Vanasco et al., 2002; ) Confalonieri, 2003 [SRC] ;( Ahern et al., 2005 ) ). Risk factors for leptospirosis for peri-urban populations in low-income countries include flooding of open sewers and streets during the rainy season ( (Sarkar et al., 2002 ) ).
Cases of hantavirus pulmonary syndrome (HPS) were first reported in Central America (Panama) in 2000, and a suggested cause was the increase in peri-domestic rodents following increased rainfall and flooding in surrounding areas ( (Bayard et al., 2000 ) ), although this requires further investigation. There are climate-related differences in hantavirus dynamics between northern and central Europe ( (Vapalahti et al., 2003; ) Pejoch and Kriz, 2006 [NPR] ).
The distribution and emergence of other infectious diseases have been affected by weather and climate variability. ENSO-driven bush fires and drought, as well as land-use and land-cover changes, have caused extensive changes in the habitat of some bat species that are the natural reservoirs for the Nipah virus. The bats were driven to farms to find food (fruits), consequently shedding virus and causing an epidemic in Malaysia and neighbouring countries ( Chua et al., 2000 [JoC] ).
The distribution of schistosomiasis, a water-related parasitic disease with aquatic snails as intermediate hosts, may be affected by climatic factors. In one area of Brazil, the length of the dry season and human population density were the most important factors limiting schistosomiasis distribution and abundance ( (Bavia et al., 1999 ) ). Over a larger area, there was an inverse association between prevalence rates and the length of the dry period ( (Bavia et al., 2001 ) ). Recent studies in China indicate that the increased incidence of schistosomiasis over the past decade may in part reflect the recent warming trend. The critical ‘freeze line’ limits the survival of the intermediate host (Oncomelania water snails) and hence limits the transmission of the parasite Schistosoma japonicum. The freeze line has moved northwards, putting an additional 20.7 million people at risk of schistosomiasis ( (Yang et al., 2005b ) ).
8.2.9 Occupational health
Changes in climate have implications for occupational health and safety. Heat stress due to high temperature and humidity is an occupational hazard that can lead to death or chronic ill-health from the after-effects of heatstroke ( (Wyndham, 1965; ) Afanas’eva et al., 1997 [NPR] ;( Adelakun et al., 1999 ) ). Both outdoor and indoor workers are at risk of heatstroke ( Leithead and Lind, 1964 [NPR] ;( Samarasinghe, 2001; ) ( Shanks and Papworth, 2001 ) ). The occupations most at risk of heatstroke, based on data from the USA, include construction and agriculture/forestry/fishing work ( (Adelakun et al., 1999; ) ( Krake et al., 2003 ) ). Acclimatisation in tropical environments does not eliminate the risk, as evidenced by the occurrence of heatstroke in metal workers in Bangladesh ( (Ahasan et al., 1999 ) ) and rickshaw pullers in South Asia ( OCHA, 2003 [NPR] ). Several of the heatstroke deaths reported in the 2003 and 2006 heatwaves in Paris were associated with occupational exposure (Senat, 2004 )
Hot working environments are not just a question of comfort, but a concern for health protection and the ability to perform work tasks. Working in hot environments increases the risk of diminished ability to carry out physical tasks ( Kerslake, 1972 [NPR] ), diminishes mental task ability ( (Ramsey, 1995 ) ), increases accident risk ( (Ramsey et al., 1983 ) ) and, if prolonged, may lead to heat exhaustion or heatstroke ( Hales and Richards, 1987 [NPR] ) (see Section 8.5 ).
8.2.10 Ultraviolet radiation and health
Solar ultraviolet radiation (UVR) exposure causes a range of health impacts. Globally, excessive solar UVR exposure has caused the loss of approximately 1.5 million disability-adjusted life years (DALYs) (0.1% of the total global burden of disease) and 60,000 premature deaths in the year 2000 . The greatest burdens result from UVR-induced cortical cataracts, cutaneous malignant melanoma, and sunburn (although the latter estimates are highly uncertain due to the paucity of data) ( Prüss-Üstün et al., 2006 [NPR] ). UVR exposure may weaken the immune response to certain vaccinations, which would reduce their effectiveness. However, there are also important health benefits: exposure to radiation in the ultraviolet B frequency band is required for the production of vitamin D in the body. Lack of sun exposure may lead to osteomalacia (rickets) and other disorders caused by vitamin D deficiencies.
Climate change will alter human exposure to UVR exposure in several ways, although the balance of effects is difficult to predict and will vary depending on location and present exposure to UVR. Greenhouse-induced cooling of the stratosphere is expected to prolong the effect of ozone-depleting gases, which will increase levels of UVR reaching some parts of the Earth’s surface ( Beggs, 2005 [SRC] ; IPCC/TEAP, 2005 ). Climate change will alter the distribution of clouds which will, in turn, affect UVR levels at the surface. Higher ambient temperatures will influence clothing choices and time spent outdoors, potentially increasing UVR exposure in some regions and decreasing it in others. If immune function is impaired and vaccine efficacy is reduced, the effects of climate-related shifts in infections may be greater than would occur in the absence of high UVR levels ( (Zwander, 2002; ) ( de Gruijl et al., 2003; ) ( Holick, 2004; ) ( Gallagher and Lee, 2006; ) Samanek et al., 2006 [MoS, SRC] ).
8.3 Assumptions about future trends
The impacts of developmental, climatic and environmental scenarios on population health are important for health-system planning processes. Also, future trends in health are relevant to climate change because the health of populations is an important element of adaptive capacity.
8.3.1 Health in scenarios
The use of scenarios to explore future effects of climate change on population health is at an early stage of development (see Section 8.4.1 ). Published scenarios describe possible future pathways based on observed trends or explicit storylines, and have been developed for a variety of purposes, including the Millennium Ecosystem Assessment (Millennium Ecosystem Assessment, 2005 [MoS, ARC] ), the IPCC Special Report on Emissions Scenarios (SRES, Nakićenović and Swart, 2000 [Ambiguous] ), GEO3 ( UNEP, 2002 [NPR] ) and the World Water Report (United Nations World Water Assessment Programme, 2003; Ebi and Gamble, 2005 [MoS, SRC] ). Examples of the many possible futures that have been described include possible changes in the patterns of infectious diseases, medical technology, and health and social inequalities ( Olshansky et al., 1998 [JoC, MoS] ; IPCC, 2000 [NPR] ; Martens and Hilderink, 2001 [NPR] ; Martens and Huynen, 2003 [MoS] ). Infectious diseases could become more prominent if public-health systems unravel, or if new pathogens arise that are resistant to our current methods of disease control, leading to falling life expectancies and reduced economic productivity ( (Barrett et al., 1998 ) ). An age of expanded medical technology could result from increased economic growth and improvements in technology, which may to some extent offset deteriorations in the physical and social environment, but at the risk of widening current health inequalities ( Martens and Hilderink, 2001 [NPR] ). Alternatively, an age of sustained health could result from more wide-ranging investment in social and medical services, leading to a reduction in the incidence of disease, benefiting most segments of the population.
Common to these scenarios is a view that major risks to health will remain unless the poorest countries share in the growth and development experienced by richer parts of the world. It is envisaged also that greater mobility and more rapid spread of ideas and technology worldwide will bring a mix of positive and negative effects on health, and that a deliberate focus on sustainability will be required to reduce the impacts of human activity on climate, water and food resources ( (Goklany, 2002 ) ).
8.3.2 Future vulnerability to climate change
The health of populations is an important element of adaptive capacity. Where there is a heavy burden of disease and disability, the effects of climate change are likely to be more severe than otherwise. For example, in Africa and Asia the future course of the HIV/AIDS epidemic will significantly influence how well populations can cope with challenges such as the spread of climate-related infections (vector- or water-borne), food shortages, and increased frequency of storms, floods and droughts ( (Dixon et al., 2002 ) ).
The total number of people at risk, the age structure of the population, and the density of settlement are important variables in any projections of the effects of climate change. Many populations will age appreciably in the next 50 years. This is relevant to climate change because the elderly are more vulnerable than younger age groups to injury resulting from weather extremes such as heatwaves, storms and floods. It is assumed (with a high degree of confidence) that over the course of the 21st century the population will grow substantially in many of the poorest countries of the world, while numbers will remain much the same, or decline, in the high-income countries. The world population will increase from its current 6.4 billion to somewhat below 9 billion by the middle of the century ( Lutz et al., 2000 [JoC] ), but regional patterns will vary widely. For example, the population density of Europe is projected to fall from 32 to 27 people/km2, while that of Africa could rise from 26 to 60 people/km2 ( Cohen, 2003 [JoC] ). Currently, 70% of all episodes of clinical Plasmodium falciparum malaria worldwide occur in Africa, and that fraction will rise substantially in the future (World Bank et al., 2004 [NPR] ). Also relevant to considerations of the impacts of climate change is urbanisation, because the effects of higher temperatures and altered patterns of rainfall are strongly modified by the local environment. For instance, during hot weather, temperatures tend to be higher in built-up areas, due to the urban heat-island effect. Almost all the growth in population in the next 50 years is expected to occur in cities (and in particular, cities in poor countries) ( Cohen, 2003 [JoC] ). These trends in population dominate calculations of the possible consequences of climate change. These are two examples: projections of the numbers of people affected by coastal flooding and the spread of malaria are more sensitive to assumptions about future population trajectories than to the choice of climate-change model ( Nicholls, 2004 [JoC, ARC] ; van Lieshout et al., 2004 [JoC] ).
For much of the world’s population, the ability to lead a healthy life is limited by the direct and indirect effects of poverty (World Bank et al., 2004 [NPR] ). Although the percentage of people living on less than US$1/day has decreased in Asia and Latin America since 1990, in the sub-Saharan region 46% of the population is now living on less than US$1/day and little improvement is expected in the short and medium term. Poverty levels in Europe and Central Asia show few signs of improvement (World Bank, 2004 [NPR] ; World Bank et al., 2004 [NPR] ). Economic growth in the richest regions has outstripped advances in other parts of the world, meaning that global disparities in income have increased in the last 20 years (UNEP and WCMC, 2002 [NotFound] ).
In the future, vulnerability to climate will depend not only on the extent of socio-economic change, but also on how evenly the benefits and costs are distributed, and the manner in which change occurs ( (McKee and Suhrcke, 2005 ) ). Economic growth is double-sided. Growth entails social change, and while this change may be wealth-creating, it may also, in the short term at least, cause significant social stress and environmental damage. Rapid urbanisation (leading to plummeting population health) in western Europe in the 19th century, and extensive land clearance (causing widespread ecological damage) in South America and South-East Asia in the 20th century, are two examples of negative consequences of rapid economic growth ( (Szreter, 2004 ) ). Social disorder, conflict, and lack of effective civic institutions will also increase vulnerability to health risks resulting from climate change.
Health services provide a buffer against the hazards of climate variability and change. For instance, access to cheap, effective anti-malarials, insecticide-treated bed nets and indoor spray programmes will be important for future trends in malaria. Emergency medical services have a role (although not a predominant one) in limiting excess mortality due to heatwaves and other extreme climate events.
There are other determinants of vulnerability that relate to particular threats, or particular settings. Heatwaves, for example, are exacerbated by the urban heat-island effect, so that impacts of high temperatures will be modified by the size and design of future cities ( Meehl and Tebaldi, 2004 [JoC, ARC] ). The consequences of changes in food production due to climate change will depend on access to international markets and the conditions of trade. If these conditions exclude or penalise poor countries, then the risks of disease and ill-health due to malnutrition will be much higher than if a more inclusive economic order is achieved. Changes in land-use practices for the production of biofuels in place of grain and other food crops will have benefits for greenhouse gas emissions reductions, but the way in which the fuels are burnt is also important (see Section 8.7.1 ).
8.4 Key future impacts and vulnerabilities
The impacts of climate change have been projected for a limited range of health determinants and outcomes for which the epidemiologic evidence base is well developed. The studies reviewed in Section 8.4.1 used quantitative and qualitative approaches to project the incidence and geographical range of health outcomes under different climate and socio-economic scenarios. Section 8.4.2 assesses the possible consequences of climate-change-related health impacts on particularly vulnerable populations and regions in the next few decades
Overall, climate change is projected to have some health benefits, including reduced cold-related mortality, reductions in some pollutant-related mortality, and restricted distribution of diseases where temperatures or rainfall exceed upper thresholds for vectors or parasites. However, the balance of impacts will be overwhelmingly negative (see Section 8.7 ). Most projections suggest modest changes in the burden of climate-sensitive health outcomes over the next few decades, with larger increases beginning mid-century. The balance of positive and negative health impacts will vary from one location to another and will alter over time as temperatures continue to rise.
8.4.1 Projections of climate-change-related health impacts
Projections of climate-change-related health impacts use different approaches to classify the risk of climate-sensitive health determinants and outcomes. For malaria and dengue, results from projections are commonly presented as maps of potential shifts in distribution. Health-impact models are typically based on climatic constraints on the development of the vector and/or parasite, and include limited population projections and non-climate assumptions. However, there are important differences between disease risk (on the basis of climatic and entomological considerations) and experienced morbidity and mortality. Although large portions of Europe and the USA may be at potential risk for malaria based on the distribution of competent disease vectors, locally acquired cases have been virtually eliminated, in part due to vector- and disease-control activities. Projections for other health outcomes often estimate populations-at-risk or person-months at risk.
Economic scenarios cannot be directly related to disease burdens because the relationships between gross domestic product (GDP) and burdens of climate-sensitive diseases are confounded by social, environmental and climate factors ( Arnell et al., 2004 [JoC, ARC] ; van Lieshout et al., 2004 [JoC] ; Pitcher et al., 2007 [NPR, SRC, 2007] ). The assumption that increasing per capita income will improve population health ignores the fact that health is determined by factors other than income alone; that good population health in itself is a critical input into economic growth and long-term economic development; and that persistent challenges to development are a reality in many countries, with continuing high burdens from relatively easy-to-control diseases ( (Goklany, 2002; ) Pitcher et al., 2007 [NPR, SRC, 2007] ).
8.4.1.1 Global burden of disease study
The World Health Organization conducted a regional and global comparative risk assessment to quantify the amount of premature morbidity and mortality due to a range of risk factors, including climate change, and to estimate the benefit of interventions to remove or reduce these risk factors. In the year 2000, climate change is estimated to have caused the loss of over 150,000 lives and 5,500,000 DALYs (0.3% of deaths and 0.4% of DALYs, respectively) ( Campbell-Lendrum et al., 2003 [NPR] ; Ezzati et al., 2004 [NPR] ; McMichael, 2004 [Ambiguous] ). The assessment also addressed how much of the future burden of climate change could be avoided by stabilising greenhouse gas emissions ( Campbell-Lendrum et al., 2003 [NPR] ). The health outcomes included were chosen based on known sensitivity to climate variation, predicted future importance, and availability of quantitative global models (or the feasibility of constructing them):
- episodes of diarrhoeal disease,
- cases of Plasmodium falciparum malaria,
- fatal accidental injuries in coastal floods and inland floods/landslides,
- the non-availability of recommended daily calorie intake (as an indicator for the prevalence of malnutrition).
Limited adjustments for adaptation were included in the estimates.
The projected relative risks attributable to climate change in 2030 vary by health outcome and region, and are largely negative, with most of the projected disease burden being due to increases in diarrhoeal disease and malnutrition, primarily in low-income populations already experiencing a large burden of disease ( Campbell-Lendrum et al., 2003 [NPR] ; McMichael, 2004 [Ambiguous] ). Absolute disease burdens depend on assumptions of population growth, future baseline disease incidence and the extent of adaptation.
The analyses suggest that climate change will bring some health benefits, such as lower cold-related mortality and greater crop yields in temperate zones, but these benefits will be greatly outweighed by increased rates of other diseases, particularly infectious diseases and malnutrition in low-income countries. A proportional increase in cardiovascular disease mortality attributable to climate extremes is projected in tropical regions, and a small benefit in temperate regions. Climate change is projected to increase the burden of diarrhoeal diseases in low-income regions by approximately 2 to 5% in 2020 . Countries with an annual GDP per capita of US$6,000 or more are assumed to have no additional risk of diarrhoea. Coastal flooding is projected to result in a large proportional mortality increase under unmitigated emissions; however, this is applied to a low burden of disease, so the aggregate impact is small. The relative risk is projected to increase as much in high- as in low-income countries. Large changes are projected in the risk of Plasmodium falciparum malaria in countries at the edge of the current distribution, with relative changes being much smaller in areas that are currently highly endemic for malaria ( McMichael et al., 2004 [Ambiguous] ;( Haines et al., 2006 ) ).
8.4.1.2 Malaria, dengue and other infectious diseases
Studies published since the TAR support previous projections that climate change could alter the incidence and geographical range of malaria. The magnitude of the projected effect may be smaller than that reported in the TAR, partly because of advances in categorising risk. There is greater confidence in projected changes in the geographical range of vectors than in changes in disease incidence because of uncertainties about trends in factors other than climate that influence human cases and deaths, including the status of the public-health infrastructure.
Table 8.2 summarises studies that project the impact of climate change on the incidence and geographical range of malaria, dengue fever and other infectious diseases. Models with incomplete parameterisation of biological relationships between temperature, vector and parasite often over-emphasise relative changes in risk, even when the absolute risk is small. Several modelling studies used the SRES climate scenarios, a few applied population scenarios, and none incorporated economic scenarios. Few studies incorporate adequate assumptions about adaptive capacity. The main approaches used are inclusion of current ‘control capacity‘ in the observed climate–health function ( Rogers and Randolph, 2000 [JoC, MoS] ; Hales et al., 2002 [MoS, SRC] ) and categorisation of the model output by adaptive capacity, thereby separating the effects of climate change from the effects of improvements in public health ( van Lieshout et al., 2004 [JoC] ).
Malaria is a complex disease to model and all published models have limited parameterisation of some of the key factors that influence the geographical range and intensity of malaria transmission. Given this limitation, models project that, particularly in Africa, climate change will be associated with geographical expansions of the areas suitable for stable Plasmodium falciparum malaria in some regions and with contractions in other regions ( (Tanser et al., 2003; ) Thomas et al., 2004 [MoS] ; van Lieshout et al., 2004 [JoC] ; Ebi et al., 2005 [Ambiguous] ). Projections also suggest that some regions will experience a longer season of transmission. This may be as important as geographical expansion for the attributable disease burden. Although an increase in months per year of transmission does not directly translate into an increase in malaria burden ( (Reiter et al., 2004 ) ), it would have important implications for vector control.
Few models project the impact of climate change on malaria outside Africa. An assessment in Portugal projected an increase in the number of days per year suitable for malaria transmission; however, the risk of actual transmission would be low or negligible if infected vectors are not present ( Casimiro et al., 2006 [ARC] ). Some central Asian areas are projected to be at increased risk of malaria, and areas in Central America and around the Amazon are projected to experience reductions in transmission due to decreases in rainfall ( van Lieshout et al., 2004 [JoC] ). An assessment in India projected shifts in the geographical range and duration of the transmission window for Plasmodium falciparum and P. vivax malaria ( (Bhattacharya et al., 2006 ) ). An assessment in Australia based on climatic suitability for the main anopheline vectors projected a likely southward expansion of habitat, although the future risk of endemicity would remain low due to the capacity to respond ( McMichael et al., 2003a [NPR, SRC] ).
Dengue is an important climate-sensitive disease that is largely confined to urban areas. Expansions of vector species that can carry dengue are projected for parts of Australia and New Zealand ( Hales et al., 2002 [MoS, SRC] ; Woodruff, 2005 [NPR, ARC] ). An empirical model based on vapour pressure projected increases in latitudinal distribution. It was estimated that, in the 2080 s, 5-6 billion people would be at risk of dengue as a result of climate change and population increase, compared with 3.5 billion people if the climate remained unchanged ( Hales et al., 2002 [MoS, SRC] ).
The projected impacts of climate change on other vector-borne diseases, including tick-borne encephalitis and Lyme disease, are discussed in the chapters dealing with Europe ( Chapter 12 ) and North America ( Chapter 14 ).
Table 8.2. Projected impacts of climate change on malaria, dengue fever and other infectious diseases.
| Health effect | Metric | Model | Climate scenario, with time slices | Temperature increase and baseline | Population projections and other assumptions | Main results | Reference |
|---|---|---|---|---|---|---|---|
| Malaria, global and regional | Population at risk in areas where climate conditions are suitable for malaria transmission | Biological model, calibrated from laboratory and field data, for falciparum malaria | HadCM3, driven by SRES A1FI, A2, B1, and B2 scenarios. 2020s, 2050s, 2080s | SRES population scenarios; current malaria control status used as an indicator of adaptive capacity | Estimates of the additional population at risk for >1 month transmission range from >220 million (A1FI) to >400 million (A2) when climate and population growth are included. The global estimates are severely reduced if transmission risk for more than 3 consecutive months per year is considered, with a net reduction in the global population at risk under the A2 and B1 scenarios. | van Lieshout et al., 2004 | |
| Malaria, Africa | Person-months at risk for stable falciparum transmission | MARA/ARMAa model of climate suitability for stable falciparum transmission | HadCM3, driven by SRES A1FI, A2a, and B1 scenarios. 2020s, 2050s, 2080s | 1.1 to 1.3°C in 2020s; 1.9 to 3.0°C in 2050s; 2.6 to 5.3°C in 2080s | Estimates based on 1995 population | By 2100, 16 to 28% increase in person-months of exposure across all scenarios, including a 5 to 7% increase in (mainly altitudinal) distribution, with limited latitudinal expansion. Countries with large areas that are close to the climatic thresholds for transmission show large potential increases across all scenarios. | Tanser et al., 2003 |
| Malaria, Africa | Map of climate suitability for stable falciparum transmission [minimum 4 months suitable per year] | MARA/ARMAa model of climate suitability for stable falciparum transmission | HadCM2 ensemble mean with medium-high emissions. 2020s, 2050s, 2080s | Climate factors only (monthly mean and minimum temperature, and monthly precipitation) | Decreased transmission in 2020s in south-east Africa. By 2050s and 2080s, localised increases in highland and upland areas, and decreases around Sahel and south central Africa. | Thomas et al., 2004 | |
| Malaria, Zimbabwe, Africa | Climate suitability for transmission | MARA/ARMAa model of climate suitability for stable falciparum transmission | 16 climate projections from COSMIC. Climate sensitivities of 1.4 and 4.5°C; equivalent CO2 of 350 and 750 ppm 2100 | None | Highlands become more suitable for transmission. The lowlands and regions with low precipitation show varying degrees of change, depending on climate sensitivity, emissions scenario and GCM. | Ebi et al., 2005 | |
| Malaria, Britain | Probability of malaria transmission | Statistical multivariate regression, based on historic distributions, land cover, agricultural factors and climate determinants | 1 to 2.5°C average temperature increase 2050s | 1 to 2.5°C average temperature increase | None. No changes in land cover or agricultural factors. | Increase in risk of local malaria transmission of 8 to 15%; highly unlikely that indigenous malaria will be re-established. | Kuhn et al., 2002 |
| Malaria, Portugal | Percentage days per year with favourable temperature for disease transmission | Transmission risk based on published thresholds | PROMES for 2040s and HadRM2 for 2090s | Average annual temperature increase of 3.3°C in 2040s and 5.8°C in 2090s, compared with 1981-1990 and 2006-2036, respectively | Some assumptions about vector distribution and/or introduction | Significant increase in the number of days suitable for survival of malaria vectors; however, if no infected vectors are present, then the risk is very low for vivax and negligible for falciparum malaria. | Casimiro and Calheiros, 2002 |
| Malaria, Australia | Geographical area suitable/unsuitable for maintenance of vector | Empirical-statistical model (CLIMEX) based on current distribution, relative abundance, and seasonal phenology of main malaria vector | CSIROMk2 and ECHAM4 driven by SRES B1, A1B, and A1FI emissions scenarios 2020, 2050 | 0.4 to 2.0°C annual average temperature increase in the 2030s, and 1.0 to 6.0°C in the 2070s, relative to 1990 (CSIRO) | Assumes adaptive capacity; used Australian population projections | ‘Malaria receptive zone‘ expands southward to include some regional towns by 2050s. Absolute risk of reintroduction very low. | McMichael et al., 2003b |
Table 8.2. Continued.
| Health effect | Metric | Model | Climate scenario, with time slices | Temperature increase and baseline | Population projections and other assumptions | Main results | Reference |
|---|---|---|---|---|---|---|---|
| Malaria, India, all states | Climate suitability for falciparum and vivax malaria transmission | Temperature transmission windows based on observed associations between temperature and malaria cases | HadRM2 driven by IS92a emissions scenario | 2 to 4°C increase compared with current climate | None | By 2050s, geographical range projected to shift away from central regions towards south-western and northern states. The duration of the transmis-sion window is likely to widen in northern and western states and shorten in southern states. | Bhattacharya et al., 2006 |
| Dengue, global | Population at risk | Statistical model based on vapour pressure. Baseline number of people at risk is 1.5 billion. | ECHAM4, HadCM2, CCSR/NIES, CGCMA2, and CGCMA1 driven by IS92a emissions scenarios | Population growth based on region-specific projections | By 2085, with both population growth and climate change, global population at risk 5 to 6 billion; with climate change only, global population at risk 3.5 billion. | Hales et al., 2002 | |
| Dengue, New Zealand | Map of vector ‘hotspots‘; dengue currently not present in New Zealand | Threshold model based on rainfall and temperature | DARLAM GCM driven by A2 and B2 emissions scenarios 2050, 2100 | None | Potential risk of dengue outbreaks in some regions under the current climate. Climate change projected to increase risk of dengue in more regions. | de Wet et al., 2001 | |
| Dengue, Australia | Map of regions climatically suitable for dengue transmission | Empirical model (Hales et al., 2002) | CSIROMk2, ECHAM4, and GFDL driven by high (A2) and low (B2) emissions scenarios and a stabilisation scenario at 450 ppm 2100 | 1.8 to 2.8°C global average temperature increase compared with 1961-1990 | None | Regions climatically suitable increase southwards; size of suitable area varies by scenario. Under the high-emissions scenario, regions as far south as Sydney could become climatically suitable. | Woodruff et al., 2005 |
| Lyme disease, Canada | Geographical range and abundance of Lyme disease vector Ixodes scapularis | Statistical model based on observed relationships; tick-abundance model | CGCM2 and HADCM2 driven by SRES A2 and B2 emissions scenarios 2020s, 2050s, 2080s | None | Northward expansion of approximately 200 km by 2020s under both scenarios, and approximately 1000 km by 2080s under A2. Under the A2 scenario, tick abundance increases 30 to 100% by 2020s and 2- to 4-fold by 2080s. Seasonality shifts. | Ogden et al., 2006 | |
| Tick-borne encephalitis, Europe | Geographical range | Statistical model based on present-day distribution | HadCM2 driven by low, medium-low, medium-high, and high degrees of change (not further defined) 2020s, 2050s, 2080s | 3.45°C increase in mean temperature in 2050s under high scenario, baseline not defined | None | From low to high degrees of climate change, tick-borne encephalitis is pushed further northeast of its present range, only moving westward into southern Scandinavia. Only under the low and medium-low scenarios does tick-borne encephalitis remain in central and eastern Europe by the 2050s. | Randolph and Rogers, 2000 |
| Diarrhoeal disease, global, 14 world regions | Diarrhoea incidence (mortality) | Statistical model, derived from cross-sectional study, including annual average temperature, water supply and sanitation coverage, and GDP per capita | SRES A1B, A2, B1 and B2 emissions scenarios 2025, 2055 | SRES population growth | Results vary by region and scenario. Generally, diarrhoeal disease increases with temperature increase. | Hijioka et al., 2002 | |
| Diarrhoeal disease, Aboriginal community, central Australia (Alice Springs) | Hospital admissions in children aged under 10 | Exposure–response relationship based on published studies | CSIROMk2 and ECHAM4 driven by SRES B1, A1B and A1FI emissions scenarios 2020, 2050 | 0.4 to 2.0°C annual average temperat-ure increase in the 2030s, and 1.0 to 6.0°C in the 2070s, relative to 1990 (CSIRO) | None | Compared with baseline, no significant increase by 2020 and an annual increase of 5 to 18% by 2050. | McMichael et al., 2003b |
| Food poisoning, England and Wales | Notified cases of food poisoning (non-specific) | Statistical model, based on observed relationship with temperature | UKCIP scenarios 2020s, 2050s, 2080s | 0.57 to 1.38°C in 2020s; 0.89 to 2.44°C in 2050s; 1.13 to 3.47°C in 2080s compared with 1961-1990 baseline | None | For +1, +2 and +3°C temperature increases, absolute increases of approximately 4,000, 9,000, and 14,000 notified cases of food poisoning | Department of Health and Expert Group on Climate Change and Health in the UK, 2001 |
8.4.1.3 Heat- and cold-related mortality
Evidence of the relationship between high ambient temperature and mortality has strengthened since the TAR, with increasing emphasis on the health impacts of heatwaves. Table 8.3 summarises projections of the impact of climate change on heat- and cold-related mortality. There is a lack of information on the effects of thermal stress on mortality outside the industrialised countries.
Table 8.3. Projected impacts of climate change on heat- and cold-related mortality.
| Area | Health effect | Model | Climate scenario, time slices | Temperature increase and baseline | Population projections and other assumptions | Main results | Reference |
|---|---|---|---|---|---|---|---|
| UK | Heat- and cold-related mortality | Empirical-statistical model derived from observed mortality | UKCIP scenarios 2020s, 2050s, 2080s | 0.57 to 1.38°C in 2020s; 0.89 to 2.44°C in 2050s; 1.13 to 3.47°C in 2080s compared with 1961-1990 baseline | Population held constant at 1996. No acclimatisation assumed. | Annual heat-related deaths increase from 798 in 1990s to 2,793 in 2050s and 3,519 in the 2080s under the medium-high scenario. Annual cold-related deaths decrease from 80,313 in 1990s to 60,021 in 2050s and 51,243 in 2080s under the medium-high scenario. | Donaldson et al., 2001 |
| Germany, Baden-Wuertemberg | Heat- and cold-related mortality | Thermo-physiological model combined with conceptual model for adaptation | ECHAM4-OPYC3 driven by SRES A1B emissions scenario. 2001-2055 compared with 1951-2001 | Population growth and aging and short-term adaptation and acclimatisation. | About a 20% increase in heat-related mortality. Increase not likely to be compensated by reductions in cold-related mortality. | Koppe, 2005 | |
| Lisbon, Portugal | Heat-related mortality | Empirical-statistical model derived from observed summer mortality | PROMES and HadRM2 2020s, 2050s, 2080s | 1.4 to 1.8°C in 2020s; 2.8 to 3.5°C in 2050s; 5.6 to 7.1°C in 2080s, compared with 1968-1998 baseline | SRES population scenarios. Assumes some acclimatisation. | Increase in heat-related mortality from baseline of 5.4 to 6 deaths/100,000 to 5.8 to 15.1 deaths/100,000 by the 2020s, 7.3 to 35.9 deaths/100,000 by the 2050s, 19.5 to 248.4 deaths/100,000 by the 2080s | Dessai, 2003 |
| Four cities in California, USA (Los Angeles, Sacramento, Fresno, Shasta Dam) | Annual number of heatwave days, length of heatwave season, and heat-related mortality | Empirical-statistical model derived from observed summer mortality | PCM and HadCM3 driven by SRES B1 and A1FI emissions scenarios 2030s, 2080s | 1.35 to 2.0°C in 2030s; 2.3 to 5.8°C in 2080s compared with 1961-1990 baseline | SRES population scenarios. Assumes some adaptation. | Increase in annual number of days classified as heatwave conditions. By 2080s, in Los Angeles, number of heatwave days increases 4-fold under B1 and 6 to 8-fold under A1FI. Annual number of heat-related deaths in Los Angeles increases from about 165 in the 1990s to 319 to 1,182 under different scenarios. | Hayhoe, 2004 |
| Australian capital cities (Adelaide, Brisbane, Canberra, Darwin, Hobart, Melbourne, Perth, Sydney) | Heat-related mortality in people older than 65 years | Empirical-statistical model, derived from observed daily mortality | CSIROMk2, ECHAM4, and HADCM2 driven by SRES A2 and B2 emissions scenarios and a stabilisation scenario at 450 ppm 2100 | 0.8 to 5.5°C increase in annual maximum temperature in the capital cities, compared with 1961-1990 baseline | Population growth and population aging. No acclimatisation. | Increase in temperature-attributable death rates from 82/100,000 across all cities under the current climate to 246/100,000 in 2100; death rates decreased with implementation of policies to mitigate GHG. | McMichael et al., 2003b |
Reductions in cold-related deaths due to climate change are projected to be greater than increases in heat-related deaths in the UK ( Donaldson et al., 2001 [NPR, SRC] ). However, projections of cold-related deaths, and the potential for decreasing their numbers due to warmer winters, can be overestimated unless they take into account the effects of influenza and season ( Armstrong et al., 2004 [SRC] ).
Heat-related morbidity and mortality is projected to increase. Heat exposures vary widely, and current studies do not quantify the years of life lost due to high temperatures. Estimates of the burden of heat-related mortality attributable to climate change are reduced, but not eliminated, when assumptions about acclimatisation and adaptation are included in models. On the other hand, increasing numbers of older adults in the population will increase the proportion of the population at risk because a decreased ability to thermo-regulate is a normal part of the aging process. Overall, the health burden could be relatively small for moderate heatwaves in temperate countries, because deaths occur primarily in susceptible persons. Additional research is needed to understand how the balance of heat-related and cold-related mortality could change under different socio-economic scenarios and climate projections.
8.4.1.4 Urban air quality
Background levels of ground-level ozone have risen since pre-industrial times because of increasing emissions of methane, carbon monoxide and nitrogen oxides; this trend is expected to continue over the next 50 years ( Fusco and Logan, 2003 [MoS] ; Prather et al., 2003 [JoC] ). Changes in concentrations of ground-level ozone driven by scenarios of future emissions and/or weather patterns have been projected for Europe and North America ( Stevenson et al., 2000 [JoC, MoS] ; Derwent et al., 2001 [JoC] ; Johnson et al., 2001 [JoC, MoS] ; Taha, 2001 [NPR, MoS] ; Hogrefe et al., 2004 [MoS, ARC] ). Future emissions are, of course, uncertain, and depend on assumptions of population growth, economic development, regulatory actions and energy use ( Syri et al., 2002 [MoS] ; Webster et al., 2002a [MoS] ). Assuming no change in the emissions of ozone precursors, the extent to which climate change affects the frequency of future ‘ozone episodes‘ will depend on the occurrence of the required meteorological conditions ( Jones and Davies, 2000 [MoS] ;( Sousounis et al., 2002; ) Hogrefe et al., 2004 [MoS, ARC] ;( Laurila et al., 2004; ) Mickley et al., 2004 [JoC, MoS] ). Table 8.4 summarises projections of future morbidity and mortality based on current exposure–mortality relationships applied to projected ozone concentrations. An increase in ozone concentrations will affect the ability of regions to achieve air-quality targets. There are no projections for cities in low- or middle-income countries, despite the heavier pollution burdens in these populations.
Table 8.4. Projected impacts of climate change on ozone-related health effects.
| Area | Health effect | Model | Climate scenario, time slices | Temperature increase and baseline | Population projections and other assumptions | Main results | Reference |
|---|---|---|---|---|---|---|---|
| New York metropolitan region, USA | Ozone-related deaths by county | Concentration response function from published epidemiological literature. Gridded ozone concentrations from CMAQ (Community Multiscale Air Quality model). | GISS driven by SRES A2 emissions scenario downscaled using MM5 2050s | 1.6 to 3.2°C in 2050s compared with 1990s | Population and age structure held constant at year 2000. Assumes no change from United States Environmental Protection Agency (USEPA) 1996 national emissions inventory and A2-consistent increases in NOx and VOCs by 2050s. | A2 climate only: 4.5% increase in ozone-related deaths. Ozone elevated in all counties. A2 climate and precursors: 4.4% increase in ozone-related deaths. (Ozone not elevated in all areas due to NOx interactions.) | Knowlton et al., 2004 |
| 50 cities, eastern USA | Ozone-related hospitalis-ations and deaths | Concentration response function from published epidemiological literature. Gridded ozone concentrations from CMAQ. | GISS driven by SRES A2 emissions scenario downscaled using MM5 2050s | 1.6 to 3.2°C in 2050s compared with 1990s | Population and age structure held constant at year 2000. Assumes no change from USEPA 1996 national emissions inventory and A2-consistent increases in NOx and VOCs by 2050s. | Maximum ozone concentrations increased for all cities, with the largest increases in cities with currently higher concentrations. 68% increase in average number of days/summer exceeding the 8-hour regulatory standard, resulting in 0.11 to 0.27% increase in non-accidental mortality and an average 0.31% increase in cardiovascular disease mortality. | Bell et al., 2007 |
| England and Wales | Exceedance days (ozone, particulates, NOx) | Statistical, based on meteorological factors for high-pollutant days (temperature, wind speed). | UKCIP scenarios 2020s, 2050s, 2080s | 0.57 to 1.38°C in 2020s; 0.89 to 2.44°C in 2050s; 1.13 to 3.47°C in 2080s compared with 1961-1990 baseline | Emissions held constant. | Over all time periods, large decreases in days with high particulates and SO2, small decrease in other pollutants except ozone, which may increase. | Anderson et al., 2001 |
There are few models of the impact of climate change on other pollutants. These tend to emphasise the role of local abatement strategies in determining the future levels of, primarily, particulate matter, and tend to project the probability of air-quality standards being exceeded instead of absolute concentrations ( Jensen et al., 2001 [MoS] ;( Guttikunda et al., 2003; ) Hicks, 2003 [MoS] ;( Slanina and Zhang, 2004 ) ); the results vary by region. The severity and duration of summertime regional air pollution episodes (as diagnosed by tracking combustion carbon monoxide and black carbon) are projected to increase in the north-eastern and Midwest USA by 2045 - 2052 because of climate-change-induced decreases in the frequency of surface cyclones ( Mickley et al., 2004 [JoC, MoS] ). A UK study projected that climate change will result in a large decrease in days with high particulate concentrations due to changes in meteorological conditions ( Anderson et al., 2001 [NPR] ). Because transboundary transport of pollutants plays a significant role in determining local to regional air quality ( (Holloway et al., 2003; ) ( Bergin et al., 2005 ) ), changing patterns of atmospheric circulation at the hemispheric to global level are likely to be just as important as regional patterns for future local air quality ( Takemura et al., 2001 [MoS] ; Langmann et al., 2003 [MoS] ).
8.4.2 Vulnerable populations and regions
Human health vulnerability to climate change was assessed based on a range of scientific evidence, including the current burdens of climate-sensitive health determinants and outcomes, projected climate-change-related exposures, and trends in adaptive capacity. Box 8.5 describes trends in climate-change-related exposures of importance to human health. As highlighted in the following sections, particularly vulnerable populations and regions are more likely to suffer harm, have less ability to respond to stresses imposed by climate variability and change, and have exhibited limited progress in reducing current vulnerabilities. For example, all persons living in a flood plain are at risk during a flood, but those with lowered ability to escape floodwaters and their consequences (such as children and the infirm, or those living in sub-standard housing) are at higher risk.
Box 8.5. Projected trends in climate-change-related exposures of importance to human health
Heatwaves, floods, droughts and other extreme events: IPCC 2007b [NPR, 2007] ) concludes, with high confidence, that heatwaves will increase, cold days will decrease over mid- to low-latitudes, and the proportion of heavy precipitation events will increase, with differences in the spatial distribution of the changes (although there will be a few areas with projected decreases in absolute numbers of heavy precipitation events) ( Meehl et al., 2007 [NPR, ARC, 2007] ). Water availability will be affected by changes in runoff due to alterations in the rainy and dry seasons.
Air quality: Climate change could affect tropospheric ozone by modifying precursor emissions, chemistry and transport; each could cause positive or negative feedbacks to climate change. Future climate change may cause either an increase or a decrease in background tropospheric ozone, due to the competing effects of higher water vapour and higher stratospheric input; increases in regional ozone pollution are expected, due to higher temperatures and weaker circulation. Future climate change may cause significant air-quality degradation by changing the dispersion rate of pollutants, the chemical environment for ozone and aerosol generation, and the strength of emissions from the biosphere, fires and dust. The sign and magnitude of these effects are highly uncertain and will vary regionally ( Denman et al., 2007 [NPR, 2007] ).
Crop yields: Chapter 5 concluded that crop productivity is projected to increase slightly at mid- to high latitudes for local mean temperature increases of up to 1-3°C depending on the crop, and then decrease beyond that in some regions. At lower latitudes, especially seasonally dry and tropical regions, crop productivity is projected to decrease for even small local temperature increases (1-2°C), which would increase the risk of hunger, with large negative effects on sub-Saharan Africa. Smallholder and subsistence farmers, pastoralists and artisanal fisherfolk will suffer complex, localised impacts of climate change.
8.4.2.1 Vulnerable urban populations
Urbanisation and climate change may work synergistically to increase disease burdens. Urban populations are growing faster in low-income than in high-income countries. The urban population increased from 220 million in 1900 to 732 million in 1950, and is estimated to have reached 3.2 billion in 2005 ( UN, 2006b [NPR] ). In 2005, 74% of the population in more-developed regions was urban, compared with 43% in less-developed regions. Approximately 4.9 billion people are projected to be urban dwellers in 2030, about 60% of the global population, including 81% of the population in more-developed regions and 56% of the population in less-developed regions.
Urbanisation can positively influence population health; for example, by making it easier to provide safe water and improved sanitation. However, rapid and unplanned urbanisation is often associated with adverse health outcomes. Urban slums and squatter settlements are often located in areas subject to landslides, floods and other natural hazards. Lack of water and sanitation in these settlements are not only problems in themselves, but also increase the difficulty of controlling disease reservoirs and vectors, facilitating the emergence and re-emergence of water-borne and other diseases ( (Obiri-Danso et al., 2001; ) Akhtar, 2002 [NPR, SRC] ;( Hay et al., 2005a ) ). Combined with declining economies, unplanned urbanisation may affect the burden and control of malaria, with the disease burden increasing among urban dwellers ( (Keiser et al., 2004 ) ). Currently, approximately 200 million people in Africa (24.6% of the total population) live in urban settings where they are at risk of malaria. In India, unplanned urbanisation has contributed to the spread of Plasmodium vivax malaria ( Akhtar et al., 2002 [NPR, SRC] ) and dengue ( Shah et al., 2004 [MoS] ). In addition, noise, overcrowding and other possible features of unplanned urbanisation may increase the prevalence of mental disorders, such as depression, anxiety, chronic stress, schizophrenia and suicide ( WHO, 2001 [NPR] ). Problems associated with rapid and unplanned urbanisation are expected to increase over the next few decades, especially in low-income countries.
Populations in high-density urban areas with poor housing will be at increased risk with increases in the frequency and intensity of heatwaves, partly due to the interaction between increasing temperatures and urban heat-island effects ( Wilby, 2003 [ARC] ). Adaptation will require diverse strategies which could include physical modification to the built environment and improved housing and building standards ( Koppe et al., 2004 [NPR, SRC] ).
8.4.2.2 Vulnerable rural populations
Climate change could have a range of adverse effects on some rural populations and regions, including increased food insecurity due to geographical shifts in optimum crop-growing conditions and yield changes in crops, reduced water resources for agriculture and human consumption, flood and storm damage, loss of cropping land through floods, droughts, a rise in sea level, and increased rates of climate-sensitive health outcomes. Water scarcity itself is associated with multiple adverse health outcomes, including diseases associated with water contaminated with faecal and other hazardous substances (including parasites), vector-borne diseases associated with water-storage systems, and malnutrition (see Chapter 3 ). Water scarcity constitutes a serious constraint to sustainable development particularly in savanna regions: these regions cover approximately 40% of the world land area ( (Rockstrom, 2003 ) ).
Attribution of current and future climate-change-related malnutrition burdens is problematic because the determinants of malnutrition are complex. Due to the very large number of people that may be affected, malnutrition linked to extreme climatic events may be one of the most important consequences of climate change. For example, climate change is projected to increase the percentage of the Malian population at risk of hunger from 34% to between 64% and 72% by the 2050 s, although this could be substantially reduced by the effective implementation of a range of adaptive strategies ( Butt et al., 2005 [JoC] ). Climate-change models project that those likely to be adversely affected are the regions already most vulnerable to food insecurity, notably Africa, which may lose substantial agricultural land. Overall, climate change is projected to increase the number of people at risk of hunger ( FAO, 2005 [NPR] ).
8.4.2.3 Food insecurity
Although the International Food Policy Research Institute’s International Model for Policy Analysis of Agricultural Commodities and Trade projects that global cereal production could increase by 56% between 1997 and 2050, primarily in temperate regions, and livestock production by 90% ( Rosegrant and Cline, 2003 [JoC] ), expert assessments of future food security are generally pessimistic over the medium term. There are indications that it will take approximately 35 additional years to reach the World Food Summit 2002 target of reducing world hunger by half by 2015 ( Rosegrant and Cline, 2003 [JoC] ; UN Millennium Project, 2005 ). Child malnutrition is projected to persist in regions of low-income countries, although the total global burden is expected to decline without considering the impact of climate change.
8.4.2.4 Populations in coastal and low-lying areas
One-quarter of the world’s population resides within 100 km distance and 100 m elevation of the coastline, with increases likely over the coming decades ( Small and Nicholls, 2003 [ARC] ). Climate change could affect coastal areas through an accelerated rise in sea level; a further rise in sea-surface temperatures; an intensification of tropical cyclones; changes in wave and storm surge characteristics; altered precipitation/runoff; and ocean acidification (see Chapter 6 ). These changes could affect human health through coastal flooding and damaged coastal infrastructure; saltwater intrusion into coastal freshwater resources; damage to coastal ecosystems, coral reefs and coastal fisheries; population displacement; changes in the range and prevalence of climate-sensitive health outcomes; amongst others. Although some Small Island States and other low-lying areas are at particular risk, there are few projections of the health impact of climate variability and change. Climate-sensitive health outcomes of concern in Small Island States include malaria, dengue, diarrhoeal diseases, heat stress, skin diseases, acute respiratory infections and asthma ( WHO, 2004a [NPR] ).
A model of a 4°C increase of the summer temperature maximum in the Netherlands in 2100, in combination with water column stratification, projected a doubling of the growth rates of selected species of potentially harmful phytoplankton in the North Sea, increasing the frequency and intensity of algal blooms that can negatively affect human health ( Peperzak, 2005 [MoS] ). Projections of impacts are complex because of substantial differences in the sensitivity to increasing ocean temperatures of phytoplankton harmful to human health.
The population at risk of flooding by storm surges throughout the 21st century has been projected based on a range of global mean sea-level rise and socio-economic scenarios ( Nicholls, 2004 [JoC, ARC] ). Under the baseline conditions, it was estimated that in 1990 about 200 million people lived beneath the 1-in-1,000-year storm surge height (e.g., people in the hazard zone), and about 10 million people/yr experienced flooding. Across all time slices, population growth increased the number of people living in a hazard zone under the four SRES scenarios (A1FI, A2, B1 and B2). Assuming that defences are upgraded against existing risks as countries become wealthier, but sea level rise is ignored, the number of people affected by flooding decreases by the 2080 s under the A1FI, B1 and B2 scenarios. Under the A2 scenario, a two-to-three-fold increase is projected in the number of people flooded per year in the 2080 s compared with 1990 . Island regions are especially vulnerable, particularly in the A1FI world, especially in South-East Asia, South Asia, the Indian Ocean coast of Africa, the Atlantic coast of Africa and the southern Mediterranean ( Nicholls, 2004 [JoC, ARC] ).
Densely populated regions in low-lying areas are vulnerable to climate change. In Bangladesh, it is projected that 4.8% of people living in unprotected dryland areas could face inundation by a water depth of 30 to 90 cm based on assumptions of a 2°C temperature increase, a 30 cm increase in sea level, an 18% increase in monsoon precipitation, and a 5% increase in monsoon discharge into major rivers (BCAS/RA/Approtech, 1994 ). This could increase to 57% of people based on assumptions of a 4°C temperature increase, a 100 cm increase in sea level, a 33% increase in monsoon precipitation, and a 10% increase in monsoon discharge into major rivers. Some areas could face higher levels of inundation (90 to 180 cm).
Studies in industrialised countries indicate that densely populated urban areas are at risk from sea-level rise (see Chapter 6 ). As demonstrated by Hurricane Katrina, areas of New Orleans (USA) and its vicinity are 1.5 to 3 m below sea level ( Burkett et al., 2003 [NPR, ARC] ). Considering the rate of subsidence and using the TAR mid-range estimate of 480 mm sea-level rise by 2100, it is projected that this region could be 2.5 to 4.0 m or more below mean sea level by 2100, and that a storm surge from a Category 3 hurricane (estimated at 3 to 4 m without waves) could be 6 to 7 m above areas that were heavily populated in 2004 ( (Manuel, 2006 ) ).
8.4.2.5 Populations in mountain regions
Changes in climate are affecting many mountain glaciers, with rapid glacier retreat documented in the Himalayas, Greenland, the European Alps, the Andes Cordillera and East Africa ( WWF, 2005 [NPR] ). Changes in the depth of mountain snowpacks and glaciers, and changes in their seasonal melting, can have significant impacts on the communities from mountains to plains that rely on freshwater runoff. For example, in China, 23% of the population live in the western regions where glacial melt provides the principal dry season water source ( Barnett et al., 2005 [JoC] ). A long-term reduction in annual glacier snow melt could result in water insecurity in some regions.
Little published information is available on the possible health consequences of climate change in mountain regions. However, it is likely that vector-borne pathogens could take advantage of new habitats at altitudes that were formerly unsuitable, and that diarrhoeal diseases could become more prevalent with changes in freshwater quality and availability (WHO Regional Office for South-East Asia, 2006 ). More extreme rainfall events are likely to increase the number of floods and landslides. Glacier lake outburst floods are a risk unique to mountain regions; these are associated with high morbidity and mortality and are projected to increase as the rate of glacier melting increases.
8.4.2.6 Populations in polar regions
The approximately 10% of the circumpolar population that is indigenous is particularly vulnerable to climate change ( ACIA, 2005 [NPR] ). Factors contributing to their vulnerability include their close relationship with the land, location of communities in coastal regions, reliance on the local environment for aspects of their diet and economy, and socio-economic and other factors ( Berner and Furgal, 2005 [NPR, SRC] ). The interactions of climate change with underlying social, cultural, economic and political trends are projected to have significant impacts on Arctic residents ( (Curtis et al., 2005 ) ).
Increasing winter temperatures in Arctic regions are projected to reduce excess winter mortality, primarily through a reduction in cardiovascular and respiratory deaths. A reduction in cold-related injuries is projected, assuming that cold protection, including human behavioural factors, does not change ( (Nayha, 2005 ) ). Observations in northern Canadian Aboriginal communities suggest that the number of land-based accidents and injuries associated with unpredictable environmental conditions such as thinning and earlier break-up of sea ice are likely to increase (e.g., Furgal et al., 2002a [NPR, SRC] , b). Diseases transmitted by wildlife and insects are projected to have a longer season in some regions such as the north-western North American Arctic, resulting in increased burdens of disease in key animal species (e.g., marine mammals, birds, fish and shellfish) that can be transmitted to humans ( (Bradley et al., 2005; ) ( Parkinson and Butler, 2005 ) ). The traditional diet of circumpolar residents is likely to be negatively affected by changes in animal migrations and distribution, and human access to them, partly because of the impacts of increasing temperatures on snow and ice timing and distribution. Further, increasing temperatures may indirectly influence human exposure to environmental contaminants in some foods (e.g., marine mammal fats). Temperature increases in the North Atlantic are projected to increase rates of mercury methylation in fish and marine mammals, thus increasing human exposure via consumption ( (Booth and Zeller, 2005 ) ).
8.5 Costs
Studies focusing on the welfare costs (and benefits) of climate-change impacts aggregate the ‘damage’ costs of climate change ( (Tol, 1995, ) 1996, 2002a, b; Fankhauser and Tol, 1997 [ARC] ; Fankhauser et al., 1997 [Ambiguous] ) or estimate the costs and benefits of measures to reduce climate change ( (Nordhaus, 1991; ) Cline, 1992 [NPR] , 2004; Nordhaus and Boyer, 2000 [NPR, MoS] ). The global economic value of loss of life due to climate change ranges between around US$6 billion and US$88 billion, in 1990 dollar prices ( (Tol, 1995, ) 1996, 2002a, b; Fankhauser and Tol, 1997 [ARC] ; Fankhauser et al., 1997 [Ambiguous] ). The economic methods for estimating welfare costs (and benefits) have several shortcomings; the studies include only a limited number of health outcomes, generally heat- and cold-related mortality and malaria. Some assessments of the direct costs of health impacts at the national level have been undertaken, but the evidence base for estimating the health effects is relatively weak ( IGCI, 2000 [NPR] ; Turpie et al., 2002 [NPR, ARC] ; Woodruff et al., 2005 [NPR, ARC] ). Where they have been estimated, the welfare costs of health impacts contribute substantially to the total costs of climate change ( Cline, 1992 [NPR] ; Tol, 2002a [MoS] ). Given the importance of these types of assessments, further research is needed.
Mortality attributable to climate change is projected to be greatest in low-income countries, where economists traditionally assign a lower value to life ( (van der Pligt et al., 1998; ) ( Hammitt and Graham, 1999; ) Viscusi and Aldy, 2003 [MoS] ). Some estimates suggest that replacing national values with a ‘global average value’ would increase the mortality costs by as much as five times ( Fankhauser et al., 1997 [Ambiguous] ). Climate change is also likely to have important direct effects on productivity via exposure of workers to heat stress (see Section 8.2.9 ). Estimates of economic impacts via changes in productivity ignore important health impacts in children and the elderly. Further research is needed to estimate productivity costs.
8.6 Adaptation: practices, options and constraints
Adaptation is needed now in order to reduce current vulnerability to the climate change that has already occurred and additional adaptation is needed in order to address the health risks projected to occur over the coming decades. Current levels of vulnerability are partly a function of the programmes and measures in place to reduce burdens of climate-sensitive health determinants and outcomes, and partly a result of the success of traditional public-health activities, including providing access to safe water and improved sanitation to reduce diarrhoeal diseases, and implementing surveillance programmes to identify and respond to outbreaks of malaria and other infectious diseases. Weak public-health systems and limited access to primary health care contribute to high levels of vulnerability and low adaptive capacity for hundreds of millions of people.
Current national and international programmes and measures that aim to reduce the burdens of climate-sensitive health determinants and outcomes may need to be revised, reoriented and, in some regions, expanded to address the additional pressures of climate change. The degree to which programmes will need to be augmented will depend on factors such as the current burden of climate-sensitive health outcomes, the effectiveness of current interventions, projections of where, when and how the burden could change with changes in climate and climate variability, access to the human and financial resources needed to implement activities, stressors that could increase or decrease resilience to impacts, and the social, economic and political context within which interventions are implemented ( Yohe and Ebi, 2005 [NPR, SRC] ; Ebi et al., 2006a [NPR, SRC] ). Some recent programmes and measures implemented to address climate variability and change are highlighted in the examples that follow.
The planning horizon of public-health decision-makers is short relative to the projected impacts of climate change, which will require modification of current risk-management approaches that focus only on short-term risks ( Ebi et al., 2006b [SRC] ). A two-tiered approach may be needed, with modifications to incorporate current climate change concerns into ongoing programmes and measures, along with regular evaluations to determine a programme’s likely effectiveness to cope with projected climate risks. For example, epidemic malaria is a public-health problem in most areas in Africa, with programmes in place to reduce the morbidity and mortality associated with these epidemics. Some projections suggest that climate change may facilitate the spread of malaria further up some highland areas (see Section 8.4.1.2 ). Therefore, programmes should not only continue their current focus, but should also consider where and when to implement additional surveillance to identify and prevent epidemics if the Anopheles vector changes its range.
How public health and other infrastructure will develop is a key uncertainty (see Section 8.3 ) that is not determined by GDP per capita alone. Public awareness, effective use of local resources, appropriate governance arrangements and community participation are necessary to mobilise and prepare for climate change ( McMichael, 2004 [Ambiguous] ). These present particular challenges in low-income countries. Furthermore, the status of and trends in other sectors affect public health, particularly water quantity, quality and sanitation (see Chapter 3 ), food quality and quantity (see Chapter 5 ), the urban environment (see Chapter 7 ), and ecosystems (see Chapter 4 ). These sectors will also be affected by climate change, creating feedback loops that can increase or decrease population vulnerability, particularly in low-income countries ( Figure 8.1 ).
8.6.1 Approaches at different scales
Pro-active adaptation strategies, policies and measures need to be implemented by regional and national governments, including Ministries of Health, by international organisations such as the World Health Organization, and by individuals. Because the range of possible health impacts of climate change is broad and the local situations diverse, the examples that follow are illustrative and not comprehensive.
8.6.1.1 National- and regional-level responses
Climate-based early warning systems for heatwaves and malaria outbreaks have been implemented at national and local levels to alert the population and relevant authorities that a disease outbreak can be expected based on climatic and environmental forecasts ( Abeku et al., 2004 [SRC] ; Teklehaimanot et al., 2004 [NPR, MoS] ; Thomson et al., 2005 [SRC] ; Kovats and Ebi, 2006 [SRC] ). To be effective in reducing health impacts, such systems must be coupled with a specific intervention plan and have an ongoing evaluation of the system and its components ( Woodruff et al., 2005 [NPR, ARC] ; Kovats and Ebi, 2006 [SRC] ).
Seasonal forecasts can be used to increase resilience to climate variability, including to weather disasters. For example, the Pacific ENSO Application Center (PEAC) alerted governments, when a strong El Niño was developing in 1997 / 1998, that severe droughts could occur, and that some islands were at unusually high risk of tropical cyclones ( Hamnett, 1998 [NPR] ). The interventions launched, such as public education and awareness campaigns, were effective in reducing the risk of diarrhoeal and vector-borne diseases. For example, despite the water shortage in Pohnpei, fewer children were admitted to hospital with severe diarrhoeal disease than normal because of frequent public-health messages about water safety. However, the interventions did not eliminate all negative health impacts, such as micronutrient deficiencies in pregnant women in Fiji.
Participatory approaches that include governments, researchers and community residents are increasingly being used to build awareness of climate-related health impacts and adaptation options, and to take advantage of local knowledge and perspectives (see Box 8.6 ).
Box 8.6. Cross-cutting case study: indigenous populations and adaptation
A series of workshops organised by the national Inuit organisation in Canada, Inuit Tapiriit Kantami, documented climate-related changes and impacts, and identified and developed potential adaptation measures for local response ( Furgal et al., 2002a [NPR, SRC] , b; Nickels et al., 2003 [NPR, SRC] ). The strong engagement of Inuit community residents will facilitate the successful adoption of the adaptation measures identified, such as using netting and screens on windows and house entrances to prevent bites from mosquitoes and other insects that have become more prevalent.
Another example is a study of the links between malaria and agriculture that included participation and input from a farming community in Mwea division, Kenya ( (Mutero et al., 2004 ) ). The approach facilitated identification of opportunities for long-term malaria control in irrigated rice-growing areas through the integration of agro-ecosystem practices aimed at sustaining livestock systems within a broader strategy for rural development.
8.6.1.2 Responses by international organisations and agencies
Improvements in international surveillance systems facilitate national and regional preparedness and reduce future vulnerability to epidemic-prone diseases. At present, surveillance systems in many parts of the world are incomplete and slow to respond to disease outbreaks. It is expected that this will improve through the implementation of the International Health Regulations. Improvements in the responsiveness and accuracy of current surveillance programmes, including addressing spatial and temporal limitations, are needed to account for and anticipate the increased pressures on disease-control programmes that are projected to result from climate change. Earth observations, monitoring and surveillance, such as remote sensing and biosensors, may increase the accuracy and precision of some of these activities ( Maynard, 2006 [NPR] ).
Donors, international and national aid agencies, emergency relief agencies, and a range of non-governmental organisations play key roles through direct aid, support of research and development, and other approaches developed in conjunction with national Ministries of Health to improve current public-health responses and to more effectively incorporate climate-change-related risks into the design, implementation and evaluation of disease-control policies and measures.
Two or more countries can develop international responses jointly when adverse health outcomes and their drivers cross borders. For example, flood prevention guidelines were developed through the United Nations Economic Commission for Europe for countries along the Elbe, Danube, Rhine and other transboundary rivers where floods have intensified due to human alteration of the environment ( UN, 2000 [NPR] ). The guidelines recognise that co-operation is needed both within and between riparian countries in order to reduce current impacts and increase future resilience.
8.6.1.3 Individual-level responses
The effectiveness of warning systems for extreme events depends on individuals taking appropriate actions, such as responding to heat alerts and flood warnings. Individuals can reduce their personal exposure by adjusting clothing and activity levels in response to high ambient temperatures and by modifying built environments, such as by the use of fans, to reduce the heat load ( (Davis et al., 2004; ) Kovats and Koppe, 2005 [NPR] ). Weather can partially determine cultural practices that may affect exposure.
Health systems need to plan for and respond to climate change ( Menne and Bertollini, 2005 [SRC] ). There are effective interventions for many of the most common causes of ill-health, but frequently these interventions do not reach those who could benefit most. One way of promoting adaptation and reducing vulnerability to climate change is to promote the uptake of effective clinical and public-health interventions in high-need cities and regions of the world. For example, health in Africa must be treated as a high priority investment in the international development portfolio ( Sachs, 2001 [NPR] ). Funding health programmes is a necessary step towards reducing vulnerability but will not be enough on its own ( (Brewer and Heymann, 2004; ) ( Regidor, 2004a, ) b; ( de Vogli et al., 2005; ) ( Macintyre et al., 2005 ) ). Progress depends also on strengthening public institutions; building health systems that work well, treating people fairly and providing universal primary health care; providing adequate education, generating demand for better and more accessible services; and ensuring that there are enough staff to do the required work ( (Haines and Cassels, 2004 ) ). Health-service infrastructure needs to be resilient to extreme events ( EEA, 2005 [NPR] ). Efforts are needed to train health professionals to understand the threats posed by climate change.
8.6.2 Integration of responses across scales
Adaptation responses to specific health risks will often cut across scales. For example, an integrated response to heatwaves could include, in addition to measures already discussed, consideration of climate change projections in the design and construction of new buildings and in the planning of new urban areas ( Kovats and Koppe, 2005 [NPR] ). In addition, national energy efficiency programmes and transport policies could include approaches for reducing both urban heat islands and emissions of ozone and other air pollutants.
Interventions designed to increase the adaptive capacity of a community or region could also facilitate the achievement of greenhouse gas mitigation targets. For example, measures to reduce the urban heat-island effect, such as planting trees, roof gardens, growth planned to reduce urban heat islands, and other measures, increase the resilience of communities to heatwaves while reducing energy requirements. Increasing the proportion of energy derived from solar, wind and other renewable resources would reduce emissions of greenhouse gases and other air pollutants from the burning of fossil fuels.
8.6.3 Limits to adaptation
Constraints to adaptation arise when one or more of the prerequisites for public-health prevention have not been met: an awareness that a problem exists; a sense that the problem matters; an understanding of what causes the problem; the capability to influence; and the political will to influence the problem ( Last, 1998 [NPR] ). Decision-makers will choose which adaptations to implement where, when and how, based on assessments of the balance between competing priorities ( Scheraga et al., 2003 [NPR, SRC] ). For example, different regions may make different assessments of the public-health and environmental-welfare implications of the ecological consequences of draining wetlands to reduce vector-breeding sites. Local laws and social customs may constrain adaptation options. For example, although the application of pesticides for vector control may be an effective adaptation measure, residents may object to spraying, even in communities with regulations to assure appropriate use. Increasing awareness of climate-change-related health impacts and knowledge diffusion of adaptation options are of fundamental importance to better decision-making.
Although specific limits will vary by health outcome and region, fundamental constraints exist in low-income countries where adaptation will partially depend on development pathways in the public-health, water, agriculture, transport, energy and housing sectors. Poverty is the most serious obstacle to effective adaptation. Despite economic growth, low-income countries are likely to remain poor and vulnerable over the medium term, with fewer options than high-income countries for adapting to climate change. Therefore, adaptation strategies should be designed in the context of development, environment, and health policies. Many of the options that can be used to reduce future vulnerability are of value in adapting to current climate and can be used to achieve other environmental and social objectives. However, because resources used for adaptation will be shared across other problems of concern to society, there is the potential for conflicts among stakeholders with differing priorities. Questions also will arise about equity (i.e., a decision that leads to differential health impacts among different demographic groups), efficiency (i.e., targeting those programmes that will yield the greatest improvements in public health), and political feasibility ( McMichael et al., 2003a [NPR, SRC] ).
8.6.4 Health implications of adaptation strategies, policies and measures
Because adaptation strategies, policies and measures can have inadvertent short- and long-term negative health consequences, potential risks should be evaluated before implementation. For example, a microdam and irrigation programme in Ethiopia developed to increase resilience to famine increased local malaria mortality by 7.3-fold ( (Ghebreyesus et al., 1999 ) ). Increased ambient temperatures due to climate change could further exacerbate the problem. In another example, air-conditioning of private and public spaces is a primary measure used in the USA to reduce heat-related morbidity and mortality ( (Davis et al., 2003 ) ); however, depending on the energy source used to generate electricity, an increased use of air conditioning can increase greenhouse gas emissions, air pollution and the urban heat island.
Measures to combat water scarcity, such as the re-use of wastewater for irrigation, have implications for human health (see Chapter 3 ). Irrigation is currently an important determinant of the spread of infectious diseases such as malaria and schistosomiasis ( (Sutherst, 2004 ) ). Strict water-quality guidelines for wastewater irrigation are designed to prevent health risks from pathogenic organisms and to guarantee crop quality ( Steenvoorden and Endreny, 2004 [NPR] ). However, in rural and peri-urban areas of most low-income countries, the use of sewage and wastewater for irrigation, a common practice, is a source of faecal–oral disease transmission. The use of wastewater for irrigation is likely to increase with climate change, and the treatment of wastewater remains unaffordable for low-income populations ( Buechler and Scott, 2000 [NPR] )
8.7 Conclusions: implications for sustainable development
Evidence has grown that climate change already contributes to the global burden of disease and premature deaths. Climate change plays an important role in the spatial and temporal distribution of malaria, dengue, tick-borne diseases, cholera and other diarrhoeal diseases; is affecting the seasonal distribution and concentrations of some allergenic pollen species; and has increased heat-related mortality. The effects are unequally distributed, and are particularly severe in countries with already high disease burdens, such as sub-Saharan Africa and Asia.
The projected health impacts of climate change are predominately negative, with the most severe impacts being seen in low-income countries, where the capacity to adapt is weakest. Vulnerable groups in developed countries will also be affected ( (Haines et al., 2006 ) ). Projected increases in temperature and changes in rainfall patterns can increase malnutrition; disease and injury due to heatwaves, floods, storms, fires and droughts; diarrhoeal illness; and the frequency of cardio-respiratory diseases due to higher concentrations of ground-level ozone. There are expected to be some benefits to health, including fewer deaths due to exposure to the cold and reductions in climate suitability for vector-borne diseases in some regions. Figure 8.3 summarises the relative direction and magnitude of projected health impacts, taking into account the likely numbers of people at risk and potential adaptive capacity.
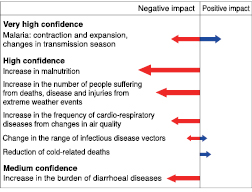
Figure 8.3. Direction and magnitude of change of selected health impacts of climate change (confidence levels are assigned based on the IPCC guidelines on uncertainty, see http://www.ipcc.ch/activity/uncertaintyguidancenote.pdf).
Health is central to the achievement of the Millennium Development Goals and to sustainable development, both directly (in the case of child mortality, maternal health, HIV/AIDS, malaria and other diseases) and indirectly (ill-health contributes to extreme poverty, hunger and lower educational achievements) ( (Haines and Cassels, 2004 ) ). Rapid and intense climate change is likely to delay progress towards achieving development targets in some regions. Recent events demonstrate that populations and health systems may be unable to cope with increases in the frequency and intensity of extreme events. These events can reduce the resilience of communities, affect vulnerable regions and localities, and overwhelm the coping capacities of most societies.
There is a need to develop and implement adaptation strategies, policies and measures at different levels and scales. Current national and international programmes and measures that aim to reduce the burdens of climate-sensitive health determinants and outcomes may need to be revised, reoriented and, in some regions, expanded to address the additional pressures of climate change. This includes the consideration of climate-change-related risks in disease monitoring and surveillance systems, health system planning, and preparedness. Many of the health outcomes are mediated through changes in the environment. Measures implemented in the water, agriculture, food, and construction sectors should be designed to benefit human health. However, adaptation is not enough.
8.7.1 Health and climate protection: clean energy
There is general agreement that health co-benefits from reduced air pollution as a result of actions to reduce GHG emissions can be substantial and may offset a substantial fraction of mitigation costs ( Barker et al., 2001 [NPR] , 2007; Cifuentes et al., 2001 [JoC] ;( West et al., 2004 ) ). In addition, actions to reduce methane emissions will decrease global concentrations of surface ozone. A portfolio of actions, including energy efficiency, renewable energy, and transport measures, is needed in order to achieve these reductions (see IPCC, 2007c [NPR, 2007] ).
In many low-income countries, access to electricity is limited. Over half of the world’s population still relies on biomass fuels and coal to meet their energy needs ( WHO, 2006 [NPR, MoS] ). These biomass fuels have low combustion efficiency and a significant, but unknown, portion is harvested non-renewably, thus contributing to net carbon emissions. The products of incomplete combustion from small-scale biomass combustion contain a number of health-damaging pollutants, including small particles, carbon monoxide, polyaromatic hydrocarbons and a range of toxic volatile organic compounds ( (Bruce et al., 2000 ) ). Human exposures to these pollutants within homes are large in comparison with outdoor air pollution exposures. Current best estimates, based on published epidemiological studies, are that biomass fuels in households are responsible annually for approximately 0.7 to 2.1 million premature deaths in low-income countries (from a combination of lower-respiratory infections, chronic obstructive pulmonary disease and lung cancer). About two-thirds occur in children under the age of five and most of the rest occur in women ( Smith et al., 2004 [NPR, SRC] ).
Clean development and other mechanisms could require calculation of the co-benefits for health when taking decisions about energy projects, including the development of alternative fuel sources ( Smith et al., 2000 [SRC] , 2005 ). Projects promoting co-benefits in low-income populations show promise to help achieve cost-effective, long-term protection from climate impacts as well as promoting immediate sustainable development goals ( Smith et al., 2000 [SRC] ).
8.8 Key uncertainties and research priorities
More empirical epidemiological research on the observed health effects of climate change have been published since the TAR, and the few national health impact assessments that have been conducted have provided valuable information on population vulnerability. However, the lack of appropriate longitudinal health data makes attribution of adverse health outcomes to observed climate trends difficult. Further, most studies have focused on middle- and high-income countries. Gaps in information persist on trends in climate, health and environment in low-income countries, where data are limited and other health priorities take precedence for research and policy development. Climate-change-related health impact assessments in low- and middle-income countries will be instrumental in guiding adaptation projects and investments.
Advances have been made in the development of climate–health impact models that project the health effects of climate change under a range of climate and socio-economic scenarios. The models are still limited to a few infectious diseases, thermal extremes and air pollution. Considerable uncertainties surround the projections, including uncertainty about how population health is likely to evolve based on changes in the level of commitment to preventing avoidable ill-health, technological developments, economic growth and other factors; the rate and intensity of future climate change; uncertainty about how the climate–health relationship might change over time; and uncertainty about the extent, rate, limiting forces and major drivers of adaptation ( McMichael et al., 2004 [Ambiguous] ). Uncertainties include not just whether the key health outcomes described in this chapter will improve, but how fast, where, when, at what cost, and whether all population groups will be able to share in these developments. Significant advances will occur by improving social and economic development, governance and resources. It is apparent that these problems will only be solved over time-frames longer than decades.
Considerable uncertainty will remain about projected climate change at geographical and temporal scales of relevance to decision-makers, increasing the importance of risk management approaches to climate risks. However, no matter what the degree of preparedness is, projections suggest that some future extreme events will be catastrophic because of the unexpected intensity of the event and the underlying vulnerability of the affected population. The European heatwave in 2003 and Hurricane Katrina are examples. The consequences of particularly severe extreme events will be greater in low-income countries. A better understanding is needed of the factors that convey vulnerability and, more importantly, the changes that need to be made in health care, emergency services, land use, urban design and settlement patterns to protect populations against heatwaves, floods, and storms.
Key research priorities include addressing the major challenges for research on climate change and health in the following ways.
- Development of methods to quantify the current impacts of climate and weather on a range of health outcomes, particularly in low- and middle-income countries.
- Development of health-impacts models for projecting climate-change-related impacts under different climate and socio-economic scenarios.
- Investigations on the costs of the projected health impacts of climate change; effectiveness of adaptation; and the limiting forces, major drivers and costs of adaptation.
Low-income countries face additional challenges, including limited capacity to identify key issues, collect and analyse data, and design, implement and monitor adaptation options. There is a need to strengthen institutions and mechanisms that can more systematically promote interactions among researchers, policy-makers and other stakeholders to facilitate the appropriate incorporation of research findings into policy decisions in order to protect population health no matter what the climate brings ( Haines et al., 2004 [Ambiguous] ).
References
Abeku, T., G. van Oortmarssen, G. Borsboom, S. de Vlas and J. Habbema, 2003: Spatial and temporal variations of malaria epidemic risk in Ethiopia: factors involved and implications. Acta Trop., 87, 331-340. [SRC]
Abeku, T.A., S.I. Hay, S. Ochola, P. Langi, B. Beard, S.J. de Vlas and J. Cox, 2004: Malaria epidemic early warning and detection in African highlands. Trends Parasitol., 20, 400-4005. [SRC]
ACIA, 2005: Arctic Climate Impact Assessment. Cambridge University Press, New York, 1042 pp. [NPR]
Adelakun, A., E. Schwartz and L. Blais, 1999: Occupational heat exposure. Appl. Occup. Environ. Hyg., 14, 153-154. Clean
Adger, W., T. Hughes, C. Folke, S. Carpenter and J. Rockstrom, 2005: Social-ecological resilience to coastal disasters. Science, 309, 1036-1039. [JoC, ARC]
Afanas’eva, R.F., N.A. Bessonova, M.A. Babaian, N.V. Lebedeva, T.K. Losik and V.V. Subbotin, 1997: Kobosnovaniiu reglamentatsii termicheskoi nagruzki sredy na rabotaiushchikh v nagrevaiushchem mikroklimate (na primere staleplavil’nogo proizvodstva) [Substantiation of the regulation of environmental heat load for workers exposed to heating microclimate (for example, steel smelting)] (in Russian). Med. Tr. Prom. Ekol., 30-34. [NPR]
Afonso, M.O., L. Campino, S. Cortes and C. Alves-Pires, 2005: The phlebotomine sandflies of Portugal. XIII. Occurrence of Phlebotomus sergenti Parrot, 1917 in the Arrabida leishmaniasis focus. Parasite, 12, 69-72. Clean
Ahasan, M.R., G. Mohiuddin, S. Vayrynen, H. Ironkannas and R. Quddus, 1999: Work-related problems in metal handling tasks in Bangladesh: obstacles to the development of safety and health measures. Ergonomics, 42, 385-396. Clean
Ahern, M.J., R.S. Kovats, P. Wilkinson, R. Few and F. Matthies, 2005: Global health impacts of floods: epidemiological evidence. Epidemiol. Rev., 27, 36-45. Clean
Akhtar, R., 2002: Urban Health in the Third World. APH Publications, New Delhi, 454 pp. [NPR, SRC]
Akhtar, R., A. Dutt and V. Wadhwa, 2002: Health planning and the resurgence of malaria in urban India. Urban Health in the Third World, R. Akhtar, Ed., AHP Publications, New Delhi, 65-92. [NPR, SRC]
Alvarez, E., F. de Pablo, C. Tomas and L. Rivas, 2000: Spatial and temporal variability of ground-level ozone in Castilla-Leon (Spain). Int. J. Biometeorol., 44, 44-51. Clean
Anand, S. and T. Barnighausen, 2004: Human resources and health outcomes: cross-country econometric study. Lancet, 364, 1603-1609. Clean
Anderson, H.R., R.G. Derwent and J. Stedman, 2001: Air pollution and climate change. Health Effects of Climate Change in the UK. Department of Health, London, 193-217. [NPR]
Anderson, K. and G. Manuel, 1994: Gender differences in reported stress response to the Loma Prieta earthquake. Sex Roles, 30, 9-10. Clean
Ando, M., S. Yamamato and S. Asanuma, 2004: Global warming and heatstroke. Japan. J. Biometeorol., 41, 45. Clean
Ansmann, A., J. Bosenberg, A. Chaikovsky, A. Comeron, S. Eckhardt, R. Eixmann, V. Freudenthaler, P. Ginoux, L. Komguem, H. Linne, M.A.L. Marquez, V. Matthias, I. Mattis, V. Mitev, D. Muller, S. Music, S. Nickovic, J. Pelon, L. Sauvage, P. Sobolewsky, M.K. Srivastava, A. Stohl, O. Torres, G. Vaughan, U. Wandinger and M. Wiegner, 2003: Long-range transport of Saharan dust to northern Europe: the 11–16 October 2001 outbreak observed with EARLINET. J. Geophys. Res. D, 108, 4783. Clean
Aramini, J., M. McLean, J. Wilson, B. Allen, W. Sears and J. Holt, 2000: Drinking Water Quality and Health Care Utilization for Gastrointestinal Illness in Greater Vancouver. Centre for Infectious Disease Prevention and Control, Foodborne, Waterborne and Zoonotic Infections Division, Health Canada, Ottawa, 79 pp. [NPR]
Aransay, A.M., J.M. Testa, F. Morillas-Marquez, J. Lucientes and P.D. Ready, 2004: Distribution of sandfly species in relation to canine leishmaniasis from the Ebro Valley to Valencia, northeastern Spain. Parasitol. Res., 94, 416-420. Clean
Ariyabandu, M. and M. Wickramasinghe, 2003: Gender Dimensions in Disaster Management: A Guide for South Asia. ITGD South Asia, Colombo, Sri Lanka, 176 pp. [NPR]
Armstrong, B., P. Mangtani, A. Fletcher, R.S. Kovats, A.J. McMichael, S. Pattenden and P. Wilkinson, 2004: Effect of influenza vaccination on excess deaths occurring during periods of high circulation of influenza: cohort study in elderly people. Brit. Med. J., 329, 660-663. [SRC]
Arnell, N.W., M.T. Livermore, R.S. Kovats, P. Levy, R.J. Nicholls, M.L. Parry and S.R. Gaffin, 2004: Climate and socio-economic scenarios for global-scale climate change impacts assessments: characterising the SRES storylines. Global Environ. Chang., 14, 3-20. [JoC, ARC]
Asero, R., 2002: Birch and ragweed pollinosis north of Milan: a model to investigate the effects of exposure to “new“ airborne allergens. Allergy, 57, 1063-1066. [MoS]
Assanarigkornchai, S., S.N. Tangboonngam and J.G. Edwards, 2004: The flooding of Hat Yai: predictors of adverse emotional responses to a natural disaster. Stress Health, 20, 81-89. [MoS]
Autoridad Nacional del Ambiente, 2000: Primera comunicacion nacional sobre cambio climatico, Panama 2000 [First National Communication on Climate Change Panama 2000]. ANAM, Panama, 136 pp. http://unfccc.int/resource/?docs/natc/pannc1/index.html. [NPR]
Aziz, K.M.A., B.A. Hoque, S. Huttly, K.M. Minnatullah, Z. Hasan, M.K. Patwary, M.M. Rahaman and S. Cairncross, 1990: Water supply, sanitation and hygiene education: Report of a health impact study in Mirzapur, Bangladesh. Water and Sanitation Report Series, No. 1, World Bank, Washington, District of Columbia, 99 pp. [NPR, ARC]
Barbraud, C. and H. Weimerskirch, 2001: Emperor penguins and climate change. Nature, 411, 183-186. [JoC]
Barker, I.K. and L.R. Lindsay, 2000: Lyme borreliosis in Ontario: determining the risks. Can. Med. Assoc. J., 162, 1573-1574. Clean
Barker, T., L. Srivastava and B. Metz, 2001: Sector costs and ancillary benefits of mitigation. Climate Change 2001: Mitigation. Contribution of Working Group III to the Third Assessment Report of the Intergovernmental Panel on Climate Change, B. Metz, O. Davidson, R. Swart and J. Pan, Eds., Cambridge University Press, Cambridge, 561-600. [NPR]
Barker, T., I. Bashmakov, A. Alharthi, M. Amann, L. Cifuentes, J. Drexhage, M. Duan, O. Edenhofer, B. Flannery, M. Grubb, M. Hoogwijk, F.I. Ibitoye, C.J. Jepma, W.A. Pizer and K. Yamaji, 2007: Mitigation from a cross-sectoral perspective. Climate Change 2007: Mitigation. Contribution of Working Group III to the Fourth Assessment Report of the Intergovernmental Panel on Climate Change, B. Metz, O. Davidson , P. Bosch, R. Dave and L. Meyer, Eds., Cambridge University Press, Cambridge, UK. [NPR, ARC, 2007]
Barnett, T.P., J.C. Adam and D.P. Lettenmaier, 2005: Potential impacts of a warming climate on water availability in snow-dominated regions. Nature, 438, 303-309. [JoC]
Barrett, R., C. Kuzawa, T. McDade and G. Armelagos, 1998: Emerging and re-emerging infectious diseases: the third epidemiologic transition. Annu. Rev. Anthropol., 27, 247-271. Clean
Basu, R. and J.M. Samet, 2002: Relation between elevated ambient temperature and mortality: a review of the epidemiologic evidence. Epidemiol. Rev., 24, 190-202. Clean
Bates, D.V., 2005: Ambient ozone and mortality. Epidemiology, 16, 427-429. Clean
Bavia, M.E., L.F. Hale, J.B. Malone, D.H. Braud and S.M. Shane, 1999: Geographic information systems and the environmental risk of schistosomiasis in Bahia, Brazil. Am. J. Trop. Med. Hyg., 60, 566-572. Clean
Bavia, M.E., J.B. Malone, L. Hale, A. Dantas, L. Marroni and R. Reis, 2001: Use of thermal and vegetation index data from earth observing satellites to evaluate the risk of schistosomiasis in Bahia, Brazil. Acta Trop., 79, 79-85. Clean
Bayard, V., E. Ortega, A. Garcia, L. Caceres, Z. Castillo, E. Quiroz, B. Armien, F. Gracia, J. Serrano, G. Guerrero, R. Kant, E. Pinifla, L. Bravo, C. Munoz, I.B. de Mosca, A. Rodriguez, C. Campos, M.A. Diaz, B. Munoz, F. Crespo, I. Villalaz, P. Rios, E. Morales, J.M.T. Sitton, L. Reneau-Vernon, M. Libel, L. Castellanos, L. Ruedas, D. Tinnin and T. Yates, 2000: Hantavirus pulmonary syndrome: Panama, 1999–2000 [Reprinted from MMWR, 49, 205-207, 2000]. JAMA–J. Am. Med. Assoc., 283, 2232. Clean
BCAS/RA/Approtech, 1994: Vulnerability of Bangladesh to climate change and sea level rise: concepts and tools for calculating risk in integrated coastal zone management. Technical Report, Bangladesh Centre for Advanced Studies (BCAS), Dhaka, 80 pp. [NPR]
Becht, M.C., M.A.L. van Tilburg, A.J.J.M. Vingerhoets, I. Nyklicek, J. de Vries, C. Kirschbaum, M.H. Antoni and G.L. van Heck, 1998: Watersnood: een verkennend onderzoek naar de gevolgen voor het welbevinden en de gezondheid van volwassenen en kinderen [Flood: a pilot study on the consequences for well-being and health of adults and children]. Tijdsch. Psychiat., 40, 277-289. Clean
Beggs, P.J., 2004: Impacts of climate change on aeroallergens: past and future. Clin. Exp. Allergy, 34, 1507-1513. [MoS, SRC]
Beggs, P.J., 2005: Admission to hospital for sunburn and drug phototoxic and photoallergic responses, New South Wales, 1993–94 to 2000–01. N.S.W. Public Health Bull., 16, 147-150. [SRC]
Beggs, P.J. and H.J. Bambrick, 2005: Is the global rise of asthma an early impact of anthropogenic climate change? Environ. Health Persp., 113, 915-919. [SRC]
Bell, M.L., F. Dominici and J.M. Samet, 2005: A meta-analysis of time-series studies of ozone and mortality with comparison to the national morbidity, mortality, and air pollution study. Epidemiology, 16, 436-445. Clean
Bell, M.L., R.D. Peng and F. Dominici, 2006: The exposure-response curve for ozone and risk of mortality and the adequacy of current ozone regulations. Environ. Health Persp., 114, 532-536. Clean
Bell, M.L., R. Goldberg, C. Hogrefe, P.L. Kinney, K. Knowlton, B. Lynn, J. Rosenthal, C. Rosenzweig and J.A. Patz, 2007: Climate change, ambient ozone, and health in 50 US cities. Climatic Change, 82, 61-76. [JoC, ARC, 2007]
Benitez, T.A., A. Rodriquez and M. Sojo, 2004: Descripcion de un brote epidemico de malaria de altura en un areas originalmente sin malaria del Estado Trujillo, Venezuela. Bol. Malariol. Salud Amb., XLIV, 999. Clean
Bennett, C.M., I.G. McKendry, S. Kelly, K. Denike and T. Koch, 2006: Impact of the 1998 Gobi dust event on hospital admissions in the Lower Fraser Valley, British Columbia. Sci. Total Environ., 366, 918-925. Clean
Bergin, M.S., J.J. West, T.J. Keating and A.G. Russell, 2005: Regional atmospheric pollution and transboundary air quality management. Annu. Rev. Env. Resour., 30, 1-37. Clean
Berner, J. and C. Furgal, 2005: Human health. Arctic Climate Impact Assessment, Arctic Climate Impact Assessment (ACIA), Cambridge University Press, Cambridge, 863-906. [NPR, SRC]
Bhattacharya, S., C. Sharma, R.C. Dhiman and A.P. Mitra, 2006: Climate change and malaria in India. Curr. Sci., 90, 369-375. Clean
Blaikie, P., T. Cannon, I. Davis and B. Wisner, 1994: At Risk: Natural Hazards, People’s Vulnerability and Disasters, 2nd ed., Routledge, New York, 320 pp. [NPR]
Bokszczanin, A., 2000: Psychologiczne konsekwencje powodzi u dzieci i mlodziezy [Psychological consequences of floods in children and youth]. Psychol. Wychowawcza, 43, 172-181. Clean
Bokszczanin, A., 2002: Long-term negative psychological effects of a flood on adolescents. Polish Psychol. Bull., 33, 55-61. Clean
Booth, S. and D. Zeller, 2005: Mercury, food webs, and marine mammals: implications of diet and climate change for human health. Environ. Health Persp., 113, 521-526. Clean
Both, C. and M.E. Visser, 2005: The effect of climate change on the correlation between avian life-history traits. Glob. Change Biol., 11, 1606-1613. [JoC]
Bouma, M. and C. Dye, 1997: Cycles of malaria associated with El Niño in Venezuela. J. Am. Med. Assoc., 278, 1772-1774. Clean
Bouma, M.J., 2003: Methodological problems and amendments to demonstrate effects of temperature on the epidemiology of malaria: a new perspective on the highland epidemics in Madagascar, 1972–1989. T. Roy. Soc. Trop. Med. H., 97, 133-139. Clean
Bouma, M.J. and M. Pascual, 2001: Seasonal and interannual cycles of endemic cholera in Bengal 1891–1940 in relation to climate and geography. Hydrobiologia, 460, 147-156. Clean
Bowman, D.M.J.S. and F.H. Johnston, 2005: Wildfire smoke, fire management, and human health. EcoHealth, 2, 76-80. Clean
Bradley, M., S.J. Kutz, E. Jenkins and T.M. O’Hara, 2005: The potential impact of climate change on infectious diseases of Arctic fauna. Int. J. Circumpolar Health, 64, 468-477. Clean
Bradshaw, W.E. and C.M. Holzapfel, 2001: Genetic shift in photoperiodic response correlated with global warming. P. Natl. Acad. Sci. USA, 98, 14509-14511. [JoC]
Braga, A., A. Zanobetti and J. Schwartz, 2002: The effect of weather on respiratory and cardiovascular deaths in 12 US cities. Environ. Health Persp., 110, 859-863. Clean
Bresser, A., 2006: The Effect of Climate Change in the Netherlands. Netherlands Environmental Assessment Agency, MNP, Bilthoven, 112 pp. [NPR]
Brewer, T.F. and S.J. Heymann, 2004: The long journey to health equity. J. Am. Med. Assoc., 292, 269-271. Clean
Briceño, S., 2002: Gender mainstreaming in disaster reduction. Commission on the Status of Women. Panel presentation. Secretariat of the International Strategy for Disaster Reduction. United Nations, International Strategy for Disaster Reduction, Geneva, 12 pp. [NPR]
Broman, T., H. Palmgren, S. Bergstrom, M. Sellin, J. Waldenstrom, M.L. Danielsson-Tham and B. Olsen, 2002: Campylobacter jejuni in black-headed gulls (Larus ridibundus): prevalence, genotypes, and influence on C. jejuni epidemiology. J. Clin. Microbiol., 40, 4594-4602. Clean
Brommer, J.E., 2004: The range margins of northern birds shift polewards. Ann. Zool. Fenn., 41, 391-397. Clean
Bruce, N., R. Perez-Padilla and R. Albalak, 2000: Indoor air pollution in developing countries: a major environmental and public health challenge. B. World Health Organ., 78, 1097-1092. Clean
Buchanan, C.M., I.J. Beverland and M.R. Heal, 2002: The influence of weather-type and long-range transport on airborne particle concentrations in Edinburgh, UK. Atmos. Environ., 36, 5343-5354. Clean
Buechler, S.J. and C.A. Scott, 2000: For Us, This is Life: Irrigating under Adverse Conditions. IWMI Latin American Series No. 20. International Water Management Institution, Bierstalpad. [NPR]
Burkett, V.R., D.B. Zilkoski and D.A. Hart, 2003: Sea level rise and subsidence: implications for flooding in New Orleans. U.S. Geological Survey Subsidence Interest Group Conference, Proceedings of the Technical Meeting, Galveston, Texas, November 27–29, 2001, 63-70. [NPR, ARC]
Burr, M.L., J.C. Emberlin, R. Treu, S. Cheng and N.E. Pearce, 2003: Pollen counts in relation to the prevalence of allergic rhinoconjunctivitis, asthma and atopic eczema in the International Study of Asthma and Allergies in Childhood (ISAAC). Clin. Exp. Allergy, 33, 1675-1680. Clean
Butt, T., B. McCarl, J. Angerer, P. Dyke and J. Stuth, 2005: The economic and flood security implications of climate change in Mali. Climatic Change, 68, 355-378. [JoC]
Cairncross, S. and M. Alvarinho, 2006: The Mozambique floods of 2000: health impact and response. Flood Hazards and Health: Responding to Present and Future Risks, R. Few and F. Matthies, Eds., Earthscan, London, 111-127. [NPR, MoS, ARC]
Calheiros, J. and E. Casimiro, 2006: Saude humana [Human health]. Alteracoes climaticas em Portugal: Cenarios, impactos e medias de adapacao – Projecto SIAM [Climate Change in Portugal: Scenarios, Impacts and Adaptation measures – SIAM Project], F. Santos and P. Miranda, Eds., Gravida, Lisbon, 451-462. [NPR]
Campbell-Lendrum, D., A. Pruss-Ustun and C. Corvalan, 2003: How much disease could climate change cause? Climate Change and Human Health: Risks and Responses, A. McMichael, D. Campbell-Lendrum, C. Corvalan, K. Ebi, A. Githeko, J. Scheraga and A. Woodward, Eds., WHO/WMO/UNEP, Geneva, 133-159. [NPR]
Carson, C., S. Hajat, B. Armstrong and P. Wilkinson, 2006: Declining vulnerability to temperature-related mortality in London over the twentieth century. Am. J. Epidemiol., 164, 77-84. Clean
Casas-Zamora, J.A. and S.A. Ibrahim, 2004: Confronting health inequity: the global dimension. Am. J. Public Health, 94, 2055. Clean
Casimiro, E. and J. Calheiros, 2002: Human health. Climate Change in Portugal: Scenarios, Impacts and Adaptation Measures – SIAM Project, F. Santos, K. Forbes and R. Moita, Eds., Gradiva, Lisbon, 241-300. [NPR]
Casimiro, E., J. Calheiros, D. Santos and S. Kovats, 2006: National assessment of human health impacts of climate change in Portugal: approach and key findings. Environ. Health Persp., 114, 1950-1956. doi:10.1289/ehp.8431. [ARC]
Cazelles, B., M. Chavez, A.J. McMichael and S. Hales, 2005: Nonstationary influence of El Niño on the synchronous dengue epidemics in Thailand. PLoS Med., 2, e106. [SRC]
CDC, 2005: Vibrio illnesses after Hurricane Katrina: multiple states, August–September 2005. MMWR–Morb. Mortal. Wkly. Rep., 54, 928-931. Clean
Cecchi, L., M. Morabito, P. Domeneghetti M., A. Crisci, M. Onorari and S. Orlandini, 2006: Long distance transport of ragweed pollen as a potential cause of allergy in central Italy. Ann. Allergy. Asthma. Im., 96, 86-91. Clean
Chan, C., L.Y. Chan, K.S. Lam, Y.S. Li, J.M. Harris and S.J. Oltmans, 2002: Effects of Asian air pollution transport and photochemistry on carbon monoxide variability and ozone production in subtropical coastal south China. J. Geophys. Res. D, 107, 4746. Clean
Chase, J.M. and T.M. Knight, 2003: Drought-induced mosquito outbreaks in wetlands. Ecol. Lett., 6, 1017-1024. Clean
Chateau-Degat, M.-L., M. Chinain, N. Cerf, S. Gingras, B. Hubert and E. Dewailly, 2005: Seawater temperature, Gambierdiscus spp. variability and incidence of ciguatera poisoning in French Polynesia. Harmful Algae, 4, 1053–1062. Clean
Chaudhury, S.K., J.M. Gore and K.C.S. Ray, 2000: Impact of heat waves in India. Curr. Sci., 79, 153-155. Clean
Checkley, W., L.D. Epstein, R.H. Gilman, D. Figueroa, R.I. Cama, J.A. Patz and R.E. Black, 2000: Effects of El Niño and ambient temperature on hospital admissions for diarrhoeal diseases in Peruvian children. Lancet, 355, 442-450. [ARC]
Checkley, W., R.H. Gilman, R.E. Black, L.D. Epstein, L. Cabrera, C.R. Sterling and L.H. Moulton, 2004: Effect of water and sanitation on childhood health in a poor Peruvian peri-urban community. Lancet, 363, 112-118. [ARC]
Chen, K., Y. Ho, C. Lai, Y. Tsai and S. Chen, 2004: Trends in concentration of ground-level ozone and meteorological conditions during high ozone episodes in the Kao-Ping Airshed, Taiwan. J. Air Waste Manage., 54, 36-48. Clean
Chen, Y. and C. Tang, 2005: Effects of Asian dust storm events on daily hospital admissions for cardiovascular disease in Taipei, Taiwan. J. Toxicol. Env. Heal. A, 68, 1457-1464. Clean
Choi, G.Y., J.N. Choi and H.J. Kwon, 2005: The impact of high apparent temperature on the increase of summertime disease-related mortality in Seoul: 1991–2000. J. Prev. Med. Pub. Health, 38, 283-290. Clean
Choudhury, A.Y. and A. Bhuiya, 1993: Effects of biosocial variable on changes in nutritional status of rural Bangladeshi children, pre- and post-monsoon flooding. J. Biosoc. Sci., 25, 351-357. Clean
Chua, K.B., W.J. Bellini, P.A. Rota, B.H. Harcourt, A. Tamin, S.K. Lam, T.G. Ksiazek, P.E. Rollin, S.R. Zaki, W. Shieh, C.S. Goldsmith, D.J. Gubler, J.T. Roehrig, B. Eaton, A.R. Gould, J. Olson, H. Field, P. Daniels, A.E. Ling, C.J. Peters, L.J. Anderson and B.W. Mahy, 2000: Nipah virus: a recently emergent deadly paramyxovirus. Science, 288, 1432-1435. [JoC]
Cifuentes, L., V.H. Borja-Aburto, N. Gouveia, G. Thurston and D.L. Davis, 2001: Climate change. Hidden health benefits of greenhouse gas mitigation. Science, 293, 1257-1259. [JoC]
Claiborn, C.S., D. Finn, T.V. Larson and J.Q. Koenig, 2000: Windblown dust contributes to high PM2.5 concentrations. J. Air Waste Manage., 50, 1440-1445. Clean
Clark, C.G., L. Price, R. Ahmed, D.L. Woodward, P.L. Melito, F.G. Rogers, D. Jamieson, B. Ciebin, A. Li and A. Ellis, 2003: Characterization of water borne disease outbreak associated Campylobacter jejuni, Walkerton, Ontario. Emerg. Infect. Dis., 9, 1232-1241. Clean
Cline, W., 1992: Economics of Global Warming. Institute for International Economics, Washington, District of Columbia, 424 pp. [NPR]
Cline, W., 2004: Meeting the challenge of global warming: reply to Manne and Mendelsohn. Copenhagen Consensus Challenge Paper, Opponents Notes Reply, 8 pp. http://www.copenhagenconsensus.com/Files/Filer/CC/Papers/Reply_-_Cline_-_Climate_Change_180504.pdf. [NPR]
Coffee, M., G. Garnett, M. Mlilo, H. Voeten, S. Chandiwana and S. Gregson, 2005: Patterns of movement and risk of HIV infection in rural Zimbabwe. J. Infect. Dis., 191, S159-S167. Clean
Cohen, J.C., 2003: Human population: the next half century. Science, 302, 1172-1175. [JoC]
Colwell, R.R., 1996: Global climate and infectious disease: the cholera paradigm. Science, 274, 2025-2031. [JoC]
Combs, D.L., L.E. Quenenmoen and R.G. Parrish, 1998: Assessing disaster attributable mortality: development and application of definition and classification matrix. Int. J. Epidemiol., 28, 1124-1129. Clean
Confalonieri, U., 2003: Climate variability, vulnerability and health in Brazil. Terra Livre, 19, 193-204. [SRC]
Conti, S., P. Meli, G. Minelli, R. Solimini, V. Toccaceli, M. Vichi, C. Beltrano and L. Perini, 2005: Epidemiologic study of mortality during the Summer 2003 heat wave in Italy. Environ. Res., 98, 390-399. Clean
Cook, A.G., P. Weinstein and J.A. Centeno, 2005: Health effects of natural dust: role of trace elements and compounds. Biol. Trace Elem. Res., 103, 1-15. Clean
Corden, J.M., W.M. Millington and J. Mullins, 2003: Long-term trends and regional variation in the aeroallergens in Cardiff and Derby UK: are differences in climate and cereal production having an effect? Aerobiologia, 19, 191. Clean
Corwin, A.L., R.P. Larasati, M.J. Bangs, S. Wuryadi, S. Arjoso, N. Sukri, E. Listyaningsih, S. Hartati, R. Namursa, Z. Anwar, S. Chandra, B. Loho, H. Ahmad, J.R. Campbell and K.R. Porter, 2001: Epidemic dengue transmission in southern Sumatra, Indonesia. T. Roy. Soc. Trop. Med. H., 95, 257-265. Clean
CPTEC, 2005: Climanálise : Boletim de Monitorimento e Análise Climática, Vol. 20, No 9, Setembro. http://www.cptec.inpe.br/products/climanalise/09?05/index.html. [NPR]
Craig, M.H., I. Kleinschmidt, J.B. Nawn, D. Le Sueur and B. Sharp, 2004: Exploring 30 years of malaria case data in KwaZulu-Natal, South Africa. Part I. The impact of climatic factors. Trop. Med. Int. Health, 9, 1247. Clean
Cummings, D.A., 2004: Travelling waves in the occurrence of dengue haemorrhagic fever in Thailand. Nature, 427, 344. [JoC]
Curriero, F., J.A. Patz, J.B. Rose and S. Lele, 2001: The association between extreme precipitation and waterborne disease outbreaks in the United States, 1948–1994. Am. J. Publ. Health, 91, 1194-1199. [ARC]
Curriero, F., K.S. Heiner, J. Samet, S. Zeger, L. Strug and J.A. Patz, 2002: Temperature and mortality in 11 cities of the Eastern United States. Am. J. Epidemiol., 155, 80-87. [ARC]
Curtis, T., S. Kvernmo and P. Bjerregaard, 2005: Changing living conditions, life style and health. Int. J. Circumpolar Health, 64, 442-450. Clean
D’Amato, G., G. Liccardi, M. D’Amato and M. Cazzola, 2002: Outdoor air pollution, climatic changes and allergic bronchial asthma. Eur. Respir. J., 20, 763-776. Clean
D’Souza, R., N. Becker, G. Hall and K. Moodie, 2004: Does ambient temperature affect foodborne disease? Epidemiology, 15, 86-92. Clean
Daniel, M., V. Danielova, B. Kriz and I. Kott, 2004: An attempt to elucidate the increased incidence of tick-borne encephalitis and its spread to higher altitudes in the Czech Republic. Int. J. Med. Microbiol., 293, 55-62. Clean
DaSilva, J., B. Garanganga, V. Teveredzi, S. Marx, S. Mason and S. Connor, 2004: Improving epidemic malaria planning, preparedness and response in Southern Africa. Malaria J., 3, 37. Clean
Davis, R., P. Knappenberger, W. Novicoff and P. Michaels, 2002: Decadal changes in heat related human mortality in the eastern United States. Climate Res., 22, 175-184. Clean
Davis, R., P. Knappenberger, P. Michaels and W. Novicoff, 2003: Changing heat-related mortality in the United States. Environ. Health Persp., 111, 1712 -1718. Clean
Davis, R., P. Knappenberger, P. Michaels and W. Novicoff, 2004: Seasonality of climate-human mortality relationships in US cities and impacts of climate change. Climate Res., 26, 61-76. Clean
Day, J.F., 2001: Predicting St. Louis encephalitis virus epidemics: lessons from recent, and not so recent, outbreaks. Annu. Rev. Entomol., 46, 111-138. [MoS]
de Graaf, R. and J. Rappole, 1995: Neotropical Migratory Birds: Natural History, Distribution and Population Change. Cornell University Press, Ithaca, New York, 676 pp. [NPR]
de Gruijl, F., J. Longstreth, C. Norval, A. Cullen, H. Slaper, M. Kripke, Y. Takizawa and J. van der Leun, 2003: Health effects from stratospheric ozone depletion and interactions with climate change. Photochem. Photobio. S., 2, 16-28. Clean
De, U.S. and R.K. Mukhopadhyay, 1998: Severe heat wave over the Indian subcontinent in 1998, in perspective of global climate. Curr. Sci., 75, 1308-1315. Clean
De, U.S., M. Khole and M. Dandekar, 2004: Natural hazards associated with meteorological extreme events. Nat. Hazards, 31, 487-497. Clean
de Vogli, R., R. Mistry, R. Gnesotto and G.A. Cornia, 2005: Has the relation between income inequality and life expectancy disappeared? Evidence from Italy and top industrialised countries. J. Epidemiol. Commun. H., 59, 158-162. Clean
de Wet, N., W. Ye, S. Hales, R.A. Warrick, A. Woodward and P. Weinstein, 2001: Use of a computer model to identify potential hotspots for dengue fever in New Zealand. New Zeal. Med. J., 11, 420-422. [MoS, SRC]
del Ninno, C. and M. Lundberg, 2005: Treading water: the long term impact of the 1998 flood on nutrition in Bangladesh. Econ. Hum. Biol., 3, 67-96. Clean
Denman, K.L., G. Brasseur, A. Chidthaisong, P. Ciais, P.M. Cox, R.E. Dickinson, D. Hauglustaine, C. Heinze, E. Holland, D. Jacob, U. Lohmann, S. Ramachandran, P.L. da Silva Dias, S.C. Wofsy and X. Zhang, 2007: Couplings between changes in the climate system and biogeochemistry. Climate Change 2007: The Physical Science Basis. Contribution of Working Group I to the Fourth Assessment Report of the Intergovernmental Panel on Climate Change, S. Solomon, D. Qin, M. Manning, Z. Chen, M. Marquis, K.B. Averyt, M. Tignor and H.L. Miller, Eds., Cambridge University Press, Cambridge, 499-588. [NPR, 2007]
Department of Health and Expert Group on Climate Change and Health in the UK, 2001: Health Effects of Climate Change in the UK. Department of Health, London, 238 pp. [NPR]
Depradine, C.A. and E.H. Lovell, 2004: Climatological variables and the incidence of dengue fever in Barbados. Int. J. Environ. Heal. R., 14, 429-441. Clean
Derwent, R.G., W.J. Collins, C.E. Johnson and D.S. Stevenson, 2001: Transient behaviour of tropospheric ozone precursors in a global 3-D CTM and their indirect greenhouse effects. Climatic Change, 49, 463-487. [JoC]
Dessai, S., 2003: Heat stress and mortality in Lisbon. Part II. An assessment of the potential impacts of climate change. Int. J. Biometeorol., 48, 37-44. Clean
Dixon, S., S. McDonald and J.A. Roberts, 2002: The impact of HIV and AIDS on Africa’s economic development. Brit. Med. J., 324, 232-234. Clean
Dominici, F., R.D. Peng, M.L. Bell, L. Pham, A. McDermott, S.L. Zeger and J.M. Samet, 2006: Fine particulate air pollution and hospital admission for cardiovascular and respiratory diseases. J. Am. Med. Assoc., 295, 1127-1134. Clean
Donaldson, G.C., R.S. Kovats, W.R. Keatinge and A. McMichael, 2001: Heat-and-cold-related mortality and morbidity and climate change. Health Effects of Climate Change in the UK, Department of Health, London, 70-80. [NPR, SRC]
Donaldson, G.C., W.R. Keatinge and S. Nayha, 2003: Changes in summer temperature and heat-related mortality since 1971 in North Carolina, South Finland, and Southeast England. Environ. Res., 91, 1-7. Clean
Durkin, M.S., N. Khan, L.L. Davidson, S.S. Zaman and Z.A. Stein, 1993: The effects of a natural disaster on child behaviour: evidence for posttraumatic stress. Am. J. Public Health, 83, 1549-1553. Clean
Ebi, K.L. and J.L. Gamble, 2005: Summary of a workshop on the development of health models and scenarios: a strategy for the future. Environ. Health Persp., 113, 335-338. [MoS, SRC]
Ebi, K.L., J. Hartman, N. Chan, J. McConnell, M. Schlesinger and J. Weyant, 2005: Climate suitability for stable malaria transmission in Zimbabwe under different climate change scenarios. Climatic Change, 73, 375-393. [JoC, SRC]
Ebi, K.L, I. Burton and B. Menne, 2006a: Policy implications for climate change related health risks. Climate Change Adaptation Strategies and Human Health, B. Menne and K. Ebi, Eds., Steinkopff, Darmstadt, 297-310. [NPR, SRC]
Ebi, K.L., J. Smith, I. Burton and J.S. Scheraga, 2006b: Some lessons learned from public health on the process of adaptation. Mitigation and Adaptation Strategies for Global Change, 11, 607-620. [SRC]
EEA, 2003: Air pollution by ozone in Europe in summer 2003: overview of exceedances of EC ozone threshold values during the summer season April–August 2003 and comparisons with previous years. Topic Report No 3/2003, European Economic Association, Copenhagen, 33 pp. http://reports.eea.europa.eu/topic_report_2003_3/en. [NPR]
EEA, 2005: Climate change and river flooding in Europe. EEA Briefing, 1, 1-4. [NPR]
Eiguren-Fernandez, A., A. Miguel, J. Froines, S. Thurairatnam and E. Avol, 2004: Seasonal and spatial variation of polycyclic aromatic hydrocarbons in vapor-phase and PM2.5 in Southern California urban and rural communities. Aerosol Sci. Tech., 38, 447 - 455. Clean
EM-DAT, 2006: The OFDA/CRED International Disaster Database. http://www.em-dat.net. [NPR]
Emberlin, J., M. Detandt, R. Gehrig, S. Jaeger, N. Nolard and A. Rantio-Lehtimaki, 2002: Responses in the start of Betula (birch) pollen seasons to recent changes in spring temperatures across Europe. Int. J. Biometeorol., 46, 159-170. Clean
Enarson, E. and B. Morrow, Eds., 1998: The Gendered Terrain of Disaster: Through Women’s Eyes. Praeger, Westport, Connecticut and London, 288 pp. [NPR]
Enscore, R., B. Biggerstaff, T. Brown, R. Fulgham, P. Reynolds, D. Engelthaler, C. Levy, R. Parmenter, J. Montenieri, J. Cheek, R. Grinnell, P. Ettestad and K. Gage, 2002: Modeling relationships between climate and the frequency of human plague cases in the southwestern United States, 1960–1997. Am. J. Trop. Med. Hyg., 66, 186-196. [MoS]
Euripidou, E. and V. Murray, 2004: Public health impacts of floods and chemical contamination. J. Public Health, 26, 376-383. Clean
Eurowinter Group, 1997: Cold exposure and winter mortality from ischaemic heart disease, cerebrovascular disease, respiratory disease, and all causes in warm and cold regions of Europe. Lancet, 349, 1341-1346. Clean
Ezzati, M., S.V. Hoorn, A. Rodgers, A.D. Lopez, C.D. Mathers and C.J. Murray, 2003: Estimates of global and regional potential health gains from reducing multiple major risk factors. Lancet, 362, 271-280. [MoS]
Ezzati, M., A. Lopez, A. Rodgers and C. Murray, Eds., 2004: Comparative Quantification of Health Risks: Global and Regional Burden of Disease due to Selected Major Risk Factors, Vols. 1 and 2. World Health Organization, Geneva, 2235 pp. [NPR]
Fallacara, D.M., C.M. Monahan, T.Y. Morishita, C.A. Bremer and R.F. Wack, 2004: Survey of parasites and bacterial pathogens from free-living waterfowl in zoological settings. Avian Dis., 48, 759-767. Clean
Fan, G.C., C.N. Chang, Y.S. Wu, S.C. Lu, P.P. Fu, S.C. Chang, C.D. Cheng and W.H. Yuen, 2002: Concentration of atmospheric particulates during a dust storm period in central Taiwan, Taichung. Sci. Total Environ., 287, 141-145. Clean
Fankhauser, S. and R.S.J. Tol, 1997: The social costs of climate change: the IPCC Second Assessment Report and beyond. Mitigation and Adaptation Strategies for Global Change, 1, 385. [ARC]
Fankhauser, S., R.S.J. Tol and D. Pearce, 1997: The aggregation of climate change damages: a welfare theoretic approach. Environ. Resour. Econ., 10, 249-266. [ARC]
FAO, 2002: The State of Food Insecurity in the World 2002. http://www.fao.org/docrep/005/y7352e/y7352e00.HTM. [NPR]
FAO, 2005: The State of Food Insecurity around the World: Eradicating Hunger – Key to Achieving the Millennium Development Goals. FAO, Rome, 40 pp. http://www.fao.org/docrep/008/a0200e/a0200e00.htm. [NPR]
Few, R. and F. Matthies, 2006: Flood Hazards and Health: Responding to Present and Future Risks. Earthscan, London, 240 pp. [NPR, MoS]
Fleury, M., D.F. Charron, J.D. Holt, O.B. Allen and A.R. Maarouf, 2006: A time series analysis of the relationship of ambient temperature and common bacterial enteric infections in two Canadian provinces. Int. J. Biometeorol., 50, 385-391. Clean
Folha, 2006: Seca nos rios da Amazônia leva animais em extinção à morte. http://www1.folha.uol.com.br/folha/ciencia/ult306u13869.shtml. [NPR]
Fothergill, A., 1998: The neglect of gender in disaster work: an overview of the literature. The Gendered Terrain of Disaster: Through Women’s Eyes, E. Enarson and B. Morrow, Eds., Praeger, Westport, Connecticut and London, 9-25. [NPR]
Franke, C.R., M. Ziller, C. Staubach and M. Latif, 2002: Impact of the El Niño/Southern Oscillation on visceral leishmaniasis, Brazil. Emerg. Infect. Dis., 8, 914-917. Clean
Frankenberg, E., D. McKee and D. Thomas, 2005: Health consequences of forest fires in Indonesia. Demography, 42, 109-129. Clean
Friend, M., R.G. McLean and F.J. Dein, 2001: Disease emergence in birds: challenges for the twenty-first century. Auk, 118, 290-303. Clean
Furgal, C., D. Martin and P. Gosselin, 2002a: Climate change in Nunavik and Labrador: lessons from Inuit knowledge. The Earth is Faster Now: Indigenous Observations on Arctic Environmental Change, I. Krupnik and D. Jolly, Eds., ARCUS, Washington, District of Columbia, 266-300. [NPR, SRC]
Furgal, C.M., D. Martin, P. Gosselin, A. Viau, Nunavik Regional Board of Health and Social Services (NRBHSS) and Labrador Inuit Association (LIA), 2002b: Climate change in Lunavik and Labrador: what we know from science and Inuit ecological knowledge. Final Report prepared for Climate Change Action Fund, WHO/PAHO Collaborating Center on Environmental and Occupational Health Impact Assessment and Surveillance, Centre Hospitalier Universitaire de Quebec (CHUQ), Beauport, Quebec, 141 pp. [NPR, SRC]
Fusco, A.C. and J.A. Logan, 2003: Analysis of 1970-1995 trends in tropospheric ozone at Northern Hemisphere midlatitudes with the GEOS-CHEM model. J. Geophys. Res. D, 108, 4449. [MoS]
Gabastou, J.M., C. Pesantes, S. Escalante, Y. Narvaez, E. Vela, L. Garcia, D. Zabala and Z.E. Yadon, 2002: Characteristics of the cholera epidemic of 1998 in Ecuador during El Niño (in Spanish). Rev. Panam. Salud Publ., 12, 157-164. Clean
Gagnon, A.S., A.B.G. Bush and K.E. Smoyer-Tomic, 2001: Dengue epidemics and the El Niño Southern Oscillation. Climate Res., 19, 35-43. Clean
Galea, S., A. Nandi and D. Vlahov, 2005: The epidemiology of post-traumatic stress disorders after disasters. Epidemiol. Rev., 27, 78-91. Clean
Gallagher, R.P. and T.K. Lee, 2006: Adverse effects of ultraviolet radiation: a brief review. Prog. Biophys. Mol. Bio., 92, 119-131. Clean
Gangoiti, G., M.M. Millan, R. Salvador and E. Mantilla, 2001: Long-range transport and re-circulation of pollutants in the western Mediterranean during the project Regional Cycles of Air Pollution in the West-Central Mediterranean Area. Atmos. Environ., 35, 6267-6276. Clean
Garrison, C.Z., E.S. Bryant, C.L. Addy, P.G. Spurrier, J.R. Freedy and D.G. Kilpatrick, 1995: Posttraumatic stress disorder in adolescents after Hurricane Andrew. J. Am. Acad. Child Psy., 34, 1193-1201. Clean
Gerolomo, M. and M.F. Penna, 1999: Os primeiros cinco anos da setima pandemia de cólera no Brasil. Informe Epid. SUS, 8, 49-58. Clean
Ghebreyesus, T.A., M. Haile, K.H. Witten, A. Getachew, A.M. Yohannes, M. Yohannes, H.D. Teklehaimanot, S.W. Lindsay and P. Byass, 1999: Incidence of malaria among children living near dams in northern Ethiopia: community based incidence survey. Brit. Med. J., 319, 663-666. Clean
Githeko, A.K. and W. Ndegwa, 2001: Predicting malaria epidemics in the Kenyan Highlands using climate data: a tool for decision makers. Global Change Human Health, 2, 54-63. [MoS, ARC]
Goklany, I., 2002: The globalization of human well-being. Policy Anal., 447, 1-20. Clean
Goulson, D., L.C. Derwent, M. Hanley, D. Dunn and S. Abolins, 2005: Predicting calyptrate fly populations from the weather, and the likely consequences of climate change. J. Appl. Ecol., 42, 784-794. [MoS]
Government of Andhra Pradesh, 2004: Report of the state level committee on heat wave conditions in Andhra Pradesh State. Revenue (Disaster Management) Department. Hyderabad, India. 67pp. [NPR]
Greenough, G., M.A. McGeehin, S.M. Bernard, J. Trtanj, J. Riad and D. Engelberg, 2001: The potential impacts of climate variability and change on health impacts of extreme weather events in the United States. Environ. Health Persp., 109, 191-198. Clean
Grize, L., A. Huss, O. Thommen, C. Schindler and C. Braun-Fahrländer, 2005: Heat wave 2003 and mortality in Switzerland. Swiss Med. Wkly., 135, 200–205. Clean
Gryparis, A., B. Forsberg, K. Katsouyanni, A. Analitis, G. Touloumi, J. Schwartz, E. Samoli, S. Medina, H.R. Anderson, E.M. Niciu, H.E. Wichmann, B. Kriz, M. Kosnik, J. Skorkovsky, J.M. Vonk and Z. Dortbudak, 2004: Acute effects of ozone on mortality from the “Air Pollution and Health: A European Approach” project. Am. J. Respir. Crit. Care Med., 170, 1080-1087. Clean
Guang, W., W. Qing and M. Ono, 2005: Investigation on Aedes aegypti and Aedes albopictus in the north-western part of Hainan Province. China Trop. Med., 5, 230-233. Clean
Guha-Sapir, P., D. Hargitt and H. Hoyois, 2004: Thirty Years of Natural Disasters 1974–2003: The Numbers. UCL, Presses Universitaires de Louvrain, Louvrain-la Neuve, 188 pp. [NPR]
Guidry, V.T. and L.H. Margolis, 2005: Unequal respiratory health risk: using GIS to explore hurricane related flooding of schools in Eastern North Carolina. Environ. Res., 98, 383-389. Clean
Guttikunda, S.K., G.R. Carmichael, G. Calori, C. Eck and J.-H. Woo, 2003: The contribution of megacities to regional sulfur pollution in Asia. Atmos. Environ., 37, 11-22. Clean
Gylfe, A., S. Bergstrom, J. Lunstrom and B. Olsen, 2000: Epidemiology: reactivation of Borrelia infection in birds. Nature, 403, 724-725. [JoC]
Haines, A. and A. Cassels, 2004: Can the Millennium Development Goals be attained? Brit. Med. J., 329, 394-397. Clean
Haines, A., S. Kuruvilla and M. Borchert, 2004: Bridging the implementation gap between knowledge and action for health. B. World Health Organ., 82, 724-732. Clean
Haines, A., R.S. Kovats, D. Campbell-Lendrum and C. Corvalan, 2006: Climate change and human health: impacts, vulnerability, and mitigation. Lancet, 367, 2101-2109. Clean
Hajat, S., 2006: Heat- and cold-related deaths in England and Wales: who is at risk? Occup. Environ. Med., 64, 93-100. Clean
Hajat, S., B. Armstrong, N. Gouveia and P. Wilkinson, 2005: Comparison of mortality displacement of heat-related deaths in Delhi, Sao Paulo and London. Epidemiology, 16, 613-620. Clean
Hajat, S., B. Armstrong, M. Baccini, A. Biggeri, L. Bisanti, A. Russo, A. Paldy, B. Menne and T. Kosatsky, 2006: Impact of high temperatures on mortality: is there an added “heat wave” effect? Epidemiology, 17, 632-638. [SRC]
Hales, J. and D. Richards, 1987: Heat stress: physical exertion and environment. Proceedings of the 1st World Conference on Heat Stress, Physical Exertion and Environment, Sydney, Australia, 27 April–1 May 1987. Excerpta Medica, Amsterdam and New York, 558 pp. [NPR]
Hales, S., P. Wienstein, Y. Souares and A. Woodward, 1999: El Niño and the dynamics of vectorborne disease transmission. Environ. Health Persp., 107, 99-102. [SRC]
Hales, S., N. de Wet, J. Maindonald and A. Woodward, 2002: Potential effect of population and climate changes on global distribution of dengue fever: an empirical model. Lancet, 360, 830-834. [MoS, SRC]
Hall, G.V., R.M. D’Souza and M.D. Kirk, 2002: Foodborne disease in the new millennium: out of the frying pan and into the fire. Med. J. Australia, 177, 614-618. Clean
Hammitt, J.K. and J.D. Graham, 1999: Willingness to pay for health protection: inadequate sensitivity to probability? J. Risk Uncertainty, 18, 33-62. Clean
Hamnett, M.P., 1998: The Pacific ENSO Applications Centre and the 1997-98 El Niño. Pacific ENSO Update, 4. [NPR]
Hari Kumar, R., K. Venkaiah, N. Arlappa, S. Kumar, G. Brahmam and K. Vijayaraghavan, 2005: Diet and nutritional status of the population in the severely drought affected areas of Gujarat. J. Hum. Ecol., 18, 319-326. Clean
Harrison, R.M., A.M. Jones, P.D. Biggins, N. Pomeroy, C.S. Cox, S.P. Kidd, J.L. Hobman, N.L. Brown and A. Beswick, 2005: Climate factors influencing bacterial count in background air samples. Int. J. Biometeorol., 49, 167-178. Clean
Hartley, S. and D.A. Robinson, 2000: A shift in winter season timing in the Northern Plains of the USA as indicated by temporal analysis of heating degree days. Int. J. Climatol., 20, 365-379. [JoC]
Hassi, J. and M. Rytkonen, 2005: Climate warming and health adaptation in Finland. FINADAPT Working Paper 7, Finnish Environment Institute Mimeographs 337, Helsinki, 28 pp. [NPR]
Hassi, J., M. Rytkonen, J. Kotaniemi and H. Rintamaki, 2005: Impacts of cold climate on human heat balance, performance and health in circumpolar areas. Int. J. Circumpolar Health, 64, 459-467. Clean
Hay, S.I., D.J. Rogers, S.E. Randolph, D.I. Stern, J. Cox, G.D. Shanks and R.W. Snow, 2002a: Hot topic or hot air? Climate change and malaria resurgence in East African highlands. Trends Parasitol., 18, 530-534. Clean
Hay, S.I., J. Cox, D.J. Rogers, S.E. Randolph, D.I. Stern, G.D. Shanks, M.F. Myers and R.W. Snow, 2002b: Climate change and the resurgence of malaria in the East African highlands. Nature, 415, 905-909. [JoC]
Hay, S.I., C.A. Guerra, A.J. Tatem, P.M. Atkinson and R.W. Snow, 2005a: Urbanization, malaria transmission and disease burden in Africa. Nat. Rev. Microbiol., 3, 81-90. Clean
Hay, S.I., G.D. Shanks, D.I. Stern, R.W. Snow, S.E. Randolph and D.J. Rogers, 2005b: Climate variability and malaria epidemics in the highlands of East Africa. Trends Parasitol., 21, 52-53. Clean
Hayhoe, K., 2004: Emissions pathways, climate change, and impacts on California. P. Natl. Acad. Sci. USA, 101, 12422. [PoC, JoC, ARC]
Hazenkamp-von Arx, M.E., T. Gotschi Fellmann, L. Oglesby, U. Ackermann-Liebrich, T. Gislason, J. Heinrich, D. Jarvis, C. Luczynska, A.J. Manzanera, L. Modig, D. Norback, A. Pfeifer, A. Poll, M. Ponzio, A. Soon, P. Vermeire and N. Kunzli, 2003: PM2.5 assessment in 21 European study centers of ECRHS II: method and first winter results. J. Air Waste Manage, 53, 617-628. Clean
He, Z., Y.J. Kim, K.O. Ogunjobi and C.S. Hong, 2003: Characteristics of PM2.5 species and long-range transport of air masses at Taean background station, South Korea. Atmos. Environ., 37, 219-230. Clean
Healy, J.D., 2003: Excess winter mortality in Europe: a cross country analysis identifying key risk factors. J. Epidemiol. Commun. H., 57, 784-789. Clean
Hegerl, G.C., F.W. Zwiers, P. Braconnot, N.P. Gillett, Y. Luo, J.A. Marengo Orsini, N. Nicholls, J.E. Penner and P.A. Stott, 2007: Understanding and attributing climate change. Climate Change 2007: The Physical Science Basis. Contribution of Working Group I to the Fourth Assessment Report of the Intergovernmental Panel on Climate Change, S. Solomon, D. Qin, M. Manning, Z. Chen, M. Marquis, K.B. Averyt, M. Tignor and H.L. Miller, Eds., Cambridge University Press, Cambridge, 663-746. [NPR, ARC, 2007]
Heller, L., E. Colosimo and C. Antunes, 2003: Environmental sanitation conditions and health impact: a case-control study. Rev. Soc. Bras. Med. Tro., 36, 41-50. Clean
Helmis, C.G., N. Moussiopoulos, H.A. Flocas, P. Sahm, V.D. Assimakopoulos, C. Naneris and P. Maheras, 2003: Estimation of transboundary air pollution on the basis of synoptic-scale weather types. Int. J. Climatol., 23, 405-416. [JoC, MoS]
Hemon, D. and E. Jougla, 2004: La canicule du mois d’aout 2003 en France [The heatwave in France in August 2003]. Rev. Epidemiol. Santé, 52, 3-5. Clean
Hicks, B.B., 2003: Planning for air quality concerns of the future. Pure Appl. Geophys., 160, 57-74. [MoS]
Hijioka, Y., K. Takahashi, Y. Matsuoka and H. Harasawa, 2002: Impact of global warming on waterborne diseases. J. Jpn. Soc. Water Environ., 25, 647-652. [ARC]
Hogrefe, C., J. Biswas, B. Lynn, K. Civerolo, J.Y. Ku, J. Rosenthal, C. Rosenzweig, R. Goldberg and P.L. Kinney, 2004: Simulating regional-scale ozone climatology over the eastern United States: model evaluation results. Atmos. Environ., 38, 2627. [MoS, ARC]
Holick, M.F., 2004: Sunlight and vitamin D for bone health and prevention of autoimmune diseases, cancers and cardiovascular disease. Am. J. Clin. Nutr., 80, 1678S-1688S. Clean
Holloway, T., A. Fiore and M.G. Hastings, 2003: Intercontinental transport of air pollution: will emerging science lead to a new hemispheric treaty? Environ Sci. Technol., 37, 4535-4542. Clean
Honda, Y., M. Ono, A. Sasaki and I. Uchiyama, 1998: Shift of the short term temperature mortality relationship by a climate factor: some evidence necessary to take account of in estimating the health effect of global warming. J. Risk Res., 1, 209-220. [MoS, ARC]
Hopp, M.J. and J.A. Foley, 2003: Worldwide fluctuations in dengue fever cases related to climate variability. Climate Res., 25, 85-94. Clean
Hoyt, K.S. and A.E. Gerhart, 2004: The San Diego County wildfires: perspectives of health care. Disaster Manage. Response, 2, 46-52. Clean
Hubalek, Z., 2004: An annotated checklist of pathogenic microorganisms associated with migratory birds. J. Wildlife Dis., 40, 639-659. Clean
Hunter, P.R., 2003: Climate change and waterborne and vectorborne disease. J. Appl. Microbiol., 94, 37-46. Clean
Huynen, M. and B. Menne, 2003: Phenology and human health: allergic disorders. Report of a WHO meeting in Rome, Italy, 16–17 January 2003. Health and Global Environmental Series, EUR/03/5036791. World Health Organization, Copenhagen, 64 pp. [NPR, SRC]
Ibald-Mulli, A., H.E. Wichmann, W. Kreyling and A. Peters, 2002: Epidemiological evidence on health effects of ultrafine particles. J. Aerosol Med., 15, 189-201. Clean
IFRC, 2002: World Disaster Report 2002. International Federation of Red Cross and Red Crescent Societies, Geneva, 240 pp. [NPR]
IGCI, 2000: Climate Change Vulnerability and Adaptation Assessment for Fiji. Pacific Islands Climate Change Assistance Programme. International Global Change Institute, University of Waikato, Hamilton. [NPR]
INVS, 2003: Impact sanitaire de la vague de chaleur d’ août 2003 en France. Bilan et perpectives [Health Impact of the Heatwave in August 2003 in France]. Institut de Veille Sanitaire, Saint-Maurice, 120 pp. [NPR]
IPCC, 2000: Emissions Scenarios: A Special Report of Working Group III of the Intergovernmental Panel on Climate Change, N. Nakićenović and R. Swart, Eds., Cambridge University Press, New York, 570 pp. [NPR]
IPCC, 2007a: Summary for Policymakers. Climate Change 2007: The Physical Science Basis. Contribution of Working Group I to the Fourth Assessment Report of the Intergovernmental Panel on Climate Change, S. Solomon, D. Qin, M. Manning, Z. Chen, M. Marquis, K.B. Averyt, M.Tignor and H.L. Miller, Eds., Cambridge University Press, Cambridge, 18 pp. [NPR, 2007]
IPCC, 2007b: Climate Change 2007: The Physical Science Basis. Contribution of Working Group I to the Fourth Assessment Report of the Intergovernmental Panel on Climate Change, S. Solomon, D. Qin, M. Manning, Z. Chen, M. Marquis, K.B. Averyt, M. Tignor and H.L. Miller, Eds., Cambridge University Press, Cambridge, 996 pp. [NPR, 2007]
IPCC, 2007c: Climate Change 2007: Mitigation. Contribution of Working Group III to the Fourth Assessment Report of the Intergovernmental Panel on Climate Change, B. Metz, O. Davidson, P. Bosch, R. Dave and L. Meyer, Eds., Cambridge University Press, Cambridge, UK. [NPR, 2007]
IPCC/TEAP, 2005: Special Report: Safeguarding the Ozone Layer and the Global Climate System: Issues Related to Hydrofluorocarbons and Perfluorocarbons, B. Metz, L. Kuijpers, S. Solomon, S.O. Andersen, O. Davidson, J. Pons, D. de Jager, T. Kestin, M. Manning and L. Meyer, Eds., Cambridge University Press, New York, 468 pp. [NPR]
Ito, K., S.F. De Leon and M. Lippmann, 2005: Associations between ozone and daily mortality: analysis and meta-analysis. Epidemiology, 16, 446-457. Clean
Izmerov, N.F., B.A. Revich and E.I. Korenberg, 2005: Climate changes and health of population in Russia in XXI century (in Russian). Med. Tr. Prom. Ekol. 1-6. [NPR, SRC]
Jaffe, D., I. McKendry, T. Anderson and H. Price, 2003: Six “new” episodes of trans-Pacific transport of air pollutants. Atmos. Environ., 37, 91-404. Clean
Jaffe, D., I. Bertschi, L. Jaegle, P. Novelli, J.S. Reid, H. Tanimoto, R. Vingarzan and D.L. Westphal, 2004: Long-range transport of Siberian biomass burning emissions and impact on surface ozone in western North America. Geophys. Res. Lett., 31, L16106. [JoC]
Jensen, S., R. Berkowicz, M. Winther, F. Palmgren and Z. Zlatev, 2001: Future air quality in Danish cities due to new emission and fuel quality directives of the European Union. Int. J. Vehicle Des., 27, 195-208. [MoS]
Johnson, C.E., D.S. Stevenson, W.J. Collins and R.G. Derwent, 2001: Role of climate feedback on methane and ozone studied with a coupled ocean-atmosphere-chemistry model. Geophys. Res. Lett., 28, 1723-1726. [JoC, MoS]
Johnson, H., R.S. Kovats, G.R. McGregor, J.R. Stedman, M. Gibbs, H. Walton, L. Cook and E. Black, 2005: The impact of the 2003 heatwave on mortality and hospital admissions in England. Health Statistics Q., 25, 6-12. [SRC]
Jones, J.M. and T.D. Davies, 2000: The influence of climate on air and precipitation chemistry over Europe and downscaling applications to future acidic deposition. Climate Res., 14, 7-24. [MoS]
Jonkman, S.N. and I. Kelman, 2005: An analysis of the causes and circumstances of flood disaster deaths. Disasters, 29, 75-97. Clean
Jonsson, P., C. Bennet, I. Eliasson and E. Selin Lindgren, 2004: Suspended particulate matter and its relations to the urban climate in Dar es Salaam, Tanzania. Atmos. Environ., 38, 4175. Clean
Julvez, J., M. Develoux, A. Mounkaila and J. Mouchet, 1992: Diversity of malaria in the Sahelo-Saharan region: a review apropos of the status in Niger, West Africa (in French). Ann. Soc. Belg. Med. Tr., 72, 163-177. Clean
Julvez, J., J. Mouchet, A. Michault, A. Fouta and M. Hamidine, 1997: The progress of malaria in Sahelian eastern Niger: an ecological disaster zone (in French). B. Soc. Pathol. Exot., 90, 101-104. Clean
Junk, J., A. Helbig and J. Luers, 2003: Urban climate and air quality in Trier, Germany. Int. J. Biometeorol., 47, 230-238. Clean
Kabuto, M., Y. Honda and H. Todoriki, 2005: A comparative study of daily maximum and personally exposed temperatures during hot summer days in three Japanese cities (in Japanese). Nippon Koshu Eisei Zasshi, 52, 775-784. [ARC]
Kang, G., B.S. Ramakrishna, J. Daniel, M. Mathan and V. Mathan, 2001: Epidemiological and laboratory investigations of outbreaks of diarrhoea in rural South India: implications for control of disease. Epidemiol. Infect., 127, 107-112. Clean
Kappos, A.D., P. Bruckmann, T. Eikmann, N. Englert, U. Heinrich, P. Hoppe, E. Koch, G.H.M. Krause, W.G. Kreyling, K. Rauchfuss, P. Rombout, V. Schulz-Klemp, W.R. Thiel and H.E. Wichmann, 2004: Health effects of particles in ambient air. Int. J. Hyg. Envir. Heal., 207, 399-407. Clean
Kassomenos, P., A. Gryparis, E. Samoli, K. Katsouyanni, S. Lykoudis and H.A. Flocas, 2001: Atmospheric circulation types and daily mortality in Athens, Greece. Environ. Health Persp., 109, 591-596. Clean
Kato, S., Y. Kajiia, R. Itokazu, J. Hirokawad, S. Kodae and Y. Kinjof, 2004: Transport of atmospheric carbon monoxide, ozone, and hydrocarbons from Chinese coast to Okinawa island in the Western Pacific during winter. Atmos. Environ., 38, 2975-2981. Clean
Katsumata, T., D. Hosea, E.B. Wasito, S. Kohno, K. Hara, P. Soeparto and I.G. Ranuh, 1998: Cryptosporidiosis in Indonesia: a hospital-based study and a community-based survey. Am. J. Trop. Med. Hyg., 59, 628-632. Clean
Kaumov, A. and B. Muchmadeliev, 2002: Climate Change and its Impacts on Human Health. Dushanbe, Avesto, 172 pp. [NPR]
Keiser, J., J. Utzinger, M.C. De Castro, T.A. Smith, M. Tanner and B.H. Singer, 2004: Urbanization in sub-Saharan Africa and implication for malaria control. Am. J. Trop. Med. Hyg., 71, 118-127. Clean
Kellogg, C.A. and D.W. Griffin, 2006: Aerobiology and the global transport of desert dust. Trends Ecol. Evol., 21, 638-644. Clean
Kerslake, D., 1972: The Stress of Hot Environments. Cambridge University Press, Cambridge, 326 pp. [NPR]
Kistemann, T., T. Classen, C. Koch, F. Dangendorf, R. Fischeder, J. Gebel, V. Vacata and M. Exner, 2002: Microbial load of drinking water reservoir tributaries during extreme rainfall and runoff. Appl. Environ. Microbiol., 68, 2188-2197. Clean
Klich, M., M.W. Lankester and K.W. Wu, 1996: Spring migratory birds (Aves) extend the northern occurrence of blacklegged tick (Acari: Ixodidae). J. Med. Entomol., 33, 581-585. Clean
Knowlton, K., J.E. Rosenthal, C. Hogrefe, B. Lynn, S. Gaffin, R. Goldberg, C. Rosenzweig, K. Civerolo, J.Y. Ku and P.L. Kinney, 2004: Assessing ozone-related health impacts under a changing climate. Environ. Health Persp., 112, 1557-1563. [ARC]
Ko, A.I., M. Galvao Reis, C.M. Ribeiro Dourado, W.D. Johnson Jr. and L.W. Riley, 1999: Urban epidemic of severe leptospirosis in Brazil. Salvador Leptospirosis Study Group. Lancet, 354, 820-825. Clean
Koe, L., A.J. Arellano and J. McGregor, 2001: Investigating the haze transport from 1997 biomass burning in Southeast Asia: its impact upon Singapore. Atmos. Environ., 35, 2723-2734. Clean
Koelle, K., X. Rodo, M. Pascal, M. Yunus and G. Mostafa, 2005: Refractory periods and climate forcing in cholera dynamics. Nature, 436, 696. [JoC, MoS, ARC]
Kohler, S. and C. Kohler, 1992: Dead bleached coral provides new surfaces for dinoflagellates implicated in ciguatera fish poisonings. J. Env. Biol. Fish., 35, 413-416. Clean
Kohn, R., I. Levav, I. Donaire, M. Machuca and R. Tamashiro, 2005: Reacciones psicologicas y psicopatologicas en Honduras despues del huracan Mitch: implicaciones para la planificacion de los servicios [Psychological and psychopathological reactions in Honduras following Hurricane Mitch: implications for service planning] (in Spanish). Rev. Panam. Salud Publ., 18, 287-295. Clean
Koike, I., 2006: State of the art findings of global warming: contributions of the Japanese researchers and perspective in 2006. Second Report of the Global Warming Initiative, Climate Change Study Group, Ministry of Environment, Tokyo, 165-173. [NPR]
Koppe, C., 2005: Gesundheitsrelevante Bewertung von thermischer Belastung unter Berücksichtigung der kurzfristigen Anpassung der Bevölkerung and die lokalen Witterungsverhältnisse [Evaluation of Health Impacts of Thermal Exposure under Consideration of Short-term Adaptation of Populations to Local Weather] (in German). Berichte des Deutschen Wetterdienstes 226, Offenbach am Main, 167 pp. [NPR]
Koppe, C., G. Jendritzky, R.S. Kovats and B. Menne, 2004: Heat-waves: Impacts and Responses. Health and Global Environmental Change Series, No. 2. World Health Organization, Copenhagen, 123 pp. [NPR, SRC]
Korenberg, E., 2004: Environmental causes for possible relationship between climate change and changes of natural foci of diseases and their epidemiologic consequences. Climate Change and Public Health in Russia in the XXI Century: Proceedings of the International Workshop, Moscow, 54-67. [NPR]
Kosek, M., C. Bern and R.L. Guerrent, 2003: The global burden of diarrhoeal disease, as estimated from studies published between 1992 and 2000. B. World Health Organ., 81, 197-204. [MoS]
Kossmann, M. and A. Sturman, 2004: The surface wind field during winter smog nights in Christchurch and coastal Canterbury, New Zealand. Int. J. Climatol., 24, 93-108. [JoC]
Kovats, R.S. and C. Koppe, 2005: Heatwaves past and future impacts on health. Integration of Public Health with Adaptation to Climate Change: Lessons Learned and New Directions, K. Ebi, J. Smith and I. Burton, Eds., Taylor and Francis, Lisse, 136-160. [NPR]
Kovats, R.S., D. Campbell-Lendrum, A. McMichael, A. Woodward and J. Cox, 2001: Early effects of climate change: do they include changes in vector-borne disease? Philos. T. Roy. Soc. Lond. B, 356, 1057-1068. [SRC]
Kovats, R.S. and K.L. Ebi, 2006: Heatwaves and public health in Europe. Eur. J. Public Health, 16, 592-599. doi:10.1093/eurpub/ckl049. [SRC]
Kovats, R.S., M.J. Bouma, S. Hajat, E. Worrall and A. Haines, 2003: El Nino and health. Lancet, 362, 1481-1489. Clean
Kovats, R.S., S. Edwards, S. Hajat, B. Armstrong, K.L. Ebi and B. Menne, 2004: The effect of temperature on food poisoning: time series analysis in 10 European countries. Epidemiol. Infect., 132, 443-453. [SRC]
Kovats, R.S., S.J. Edwards, D. Charron, J. Cowden, R.M. D’Souza, K.L. Ebi, C. Gauci, P. Gerner-Smidt, S. Hajat, S. Hales, G.H. Pezzi, B. Kriz, K. Kutsar, P. McKeown, K. Mellou, B. Menne, S. O’Brien, W. van Pelt and H. Schmid, 2005: Climate variability and campylobacter infection: an international study. Int. J. Biometeorol., 49, 207-214. [SRC]
Krake, A., J. McCullough and B. King, 2003: Health hazards to park rangers from excessive heat at Grand Canyon National Park. Appl. Occup. Environ. Hyg., 18, 295-317. Clean
Krauss, S., D. Walker, S.P. Pryor, L. Niles, C.H. Li, V.S. Hinshaw and R.G. Webster, 2004: Influenza A viruses of migrating wild aquatic birds in North America. Vector-Borne Zoonot, 4, 177-189. Clean
Kuhn, K., D. Campbell-Lendrum and C.R. Davies, 2002: A continental risk map for malaria mosquito (Diptera: Culicidae) vectors in Europe. J. Med. Entomol., 39, 621-630. Clean
Kunii, O., S. Nakamura, R. Abdur and S. Wakai, 2002: The impact on health and risk factors of the diarrhoea epidemics in the 1998 Bangladesh floods. Public Health, 116, 68-74. Clean
Kunst, A.E., C.W. Looman and J.P. Mackenbach, 1991: The decline in winter excess mortality in the Netherlands. Int. J. Epidemiol., 20, 971-977. Clean
Kwon, H.J., S.H. Cho, Y. Chun, F. Lagarde and G. Pershagen, 2002: Effects of the Asian dust events on daily mortality in Seoul, Korea. Environ. Res., 90, 1-5. Clean
Kysely, J., 2005: Mortality and displaced mortality during heat waves in the Czech Republic. Int. J. Biometeorol., 49, 91-97. Clean
Laaidi, K., M. Pascal, M. Ledrans, A. Le Tertre, S. Medina, C. Caserio, J.C. Cohen, J. Manach, P. Beaudeau and P. Empereur-Bissonnet, 2004: Le système français d’alerte canicule et santé (SACS 2004): Un dispositif intégéré au Plan National Canicule [The French Heatwave Warning System and Health: An Integrated National Heatwave Plan]. Institutde Veille Sanitaire, 35 pp. [NPR]
Lagadec, P., 2004: Understanding the French 2003 heat wave experience: beyond the heat, a multi-layered challenge. J. Contingencies Crisis Management, 12, 160-169. Clean
Lake, I., G. Bentham, R.S. Kovats and G. Nichols, 2005: Effects of weather and river flow on cryptosporidiosis. Water Health, 3, 469-474. Clean
Lama, J.R., C.R. Seas, R. León-Barúa, E. Gotuzzo and R.B. Sack, 2004: Environmental temperature, cholera, and acute diarrhoea in adults in Lima, Peru. J. Health Popul. Nutr., 22, 399-403. Clean
Langmann, B., S. Bauer and I. Bey, 2003: The influence of the global photochemical composition of the troposphere on European summer smog. Part 1. Application of a global to mesoscale model chain. J. Geophys. Res. D, 108, 4146. [MoS]
Last, J.M., 1998: Public Health and Human Ecology. Prentice Hall International, London, 464 pp. [NPR]
Laurila, T., J. Tuovinen, V. Tarvainen and D. Simpson, 2004: Trends and scenarios of ground-level ozone concentrations in Finland. Boreal Environ. Res., 9, 167-184. Clean
Le Tertre, A., A. Lefranc, D. Eilstein, C. Declercq, S. Medina, M. Blanchard, B. Chardon, P. Fabre, L. Filleul, J.F. Jusot, L. Pascal, H. Prouvost, S. Cassadou and M. Ledrans, 2006: Impact of the 2003 heatwave on all-cause mortality in 9 French cities. Epidemiology, 17, 75-79. Clean
Lehane, L. and R.J. Lewis, 2000: Ciguatera: recent advances but the risk remains. Int. J. Food Microbiol., 61, 91-125. Clean
Leithead, C. and A. Lind, 1964: Heat Stress and Heat Disorders. Cassell, London, 304 pp. [NPR]
Lennartson, G. and M. Schwartz, 1999: A synoptic climatology of surface-level ozone in Eastern Wisconsin, USA. Climate Res., 13, 207-220. Clean
Lerchl, A., 1998: Changes in the seasonality of mortality in Germany from 1946 to 1995: the role of temperature. Int. J. Biometeorol., 42, 84-88. Clean
Levy, J.I., S.M. Chemerynski and J.A. Sarnat, 2005: Ozone exposure and mortality: an empiric bayes metaregression analysis. Epidemiology, 16, 458-468. Clean
Liang, Q., L. Jaegle, D. Jaffe, P. Weiss-Penzias, A. Heckman and J. Snow, 2004: Long-range transport of Asian pollution to the northeast Pacific: seasonal variations and transport pathways of carbon monoxide. J. Geophys. Res. D, 109, D23S07. Clean
Lim, G., J. Aramini, M. Fleury, R. Ibarra and R. Meyers, 2002: Investigating the Relationship between Drinking Water and Gastro-enteritis in Edmonton, 1993–1998. Division of Enteric, Food-borne and Waterborne Diseases, Health Canada, Ottawa, 61 pp. [NPR]
Lindgren, E. and L. Talleklint, 2000: Impact of climatic change on the northern latitude limit and population density of the disease-transmitting European tick Ixodes ricinus. Environ. Health Persp., 108, 119-123. [NPR]
Lindgren, E. and R. Gustafson, 2001: Tick-borne encephalitis in Sweden and climate change. Lancet, 358, 16-18. Clean
Lindgren, E. and T. Naucke, 2006: Leishmaniasis: influences of climate and climate change epidemiology, ecology and adaptation measures. Climate Change and Adaptation Strategies for Human Health, B. Menne and K. Ebi, Eds., Steinkopff, Darmstadt, 131-156. [NPR]
Lipp, E.K., A. Huq and R.R. Colwell, 2002: Effects of global climate on infectious disease: the cholera model. Clin. Microbiol. Rev., 15, 757. [MoS]
Louis, V.R., I.A. Gillespie, S.J. O’Brien, E. Russek-Cohen, A.D. Pearson and R.R. Colwell, 2005: Temperature-driven Campylobacter seasonality in England and Wales. Appl. Environ. Microbiol., 71, 85-92. Clean
Lutz, W., W. Sanderson and S. Scherbov, 2000: Doubling of world population unlikely. Nature, 387, 803-805. [JoC]
Macintyre, S., L. McKay and A. Ellaway, 2005: Are rich people or poor people more likely to be ill? Lay perceptions, by social class and neighbourhood, of inequalities in health. Soc. Sci. Med., 60, 313-317. Clean
Maltais, D., L. Lachance, A. Brassard and M. Dubois, 2005: Social support, coping and psychological health after a flood (in French). Sci. Soc. Santé, 23, 5-38. Clean
Manuel, J., 2006: In Katrina’s wake. Environ. Health Persp., 114, A32-A39. Clean
Marmot, M., 2005: Social determinants of health inequalities. Lancet, 365, 1099-1104. Clean
Martens, P. and H.B. Hilderink, 2001: Human health in transition: towards more disease or sustained health? Transitions in a Globalising World, P. Martens and J. Rotmans, Eds., Swets and Zeitlinger, Lisse, 61-84. [NPR]
Martens, P. and M. Huynen, 2003: A future without health? Health dimension in global scenario studies. B. World Health Organ., 81, 896-901. [MoS]
Martin, B., H. Fuelberg, N. Blake, J. Crawford, L. Logan, D. Blake and G. Sachse, 2002: Long-range transport of Asian outflow to the equatorial Pacific. J. Geophys. Res. D, 108, 8322. Clean
Martinez-Navarro, F., F. Simon-Soria and G. Lopez-Abente, 2004: Valoracion del impacto de la ola de calor del verano de 2003 sobre la mortalidad [Evaluation of the impact of the heatwave in the summer of 2003 on mortality]. Gac. Sanit., 18, 250-258. Clean
Mascie-Taylor, C.G. and E. Karim, 2003: The burden of chronic disease. Science, 302, 1921-1922. [JoC]
Mason, J.B., A. Bailes, K.E. Mason, O. Yambi, U. Jonsson, C. Hudspeth, P. Hailey, A. Kendle, D. Brunet and P. Martel, 2005: AIDS, drought, and child malnutrition in southern Africa. Public Health Nutr., 8, 551-563. Clean
Maynard, N.G., 2006: Satellites, settlements and human health. Remote Sensing of Human Settlements: Manual of Remote Sensing, M. Ridd and J.D. Hipple, Eds., American Society of Photogrammetry and Remote Sensing, Bethesda, Maryland, 379-399. [NPR]
McGregor, G.R., 1999: Basic meteorology. Air Pollution and Health, S.T. Holgate, J. Samet, H. Koren and R.L. Maynard, Eds., Academic Press, San Diego, California, 21-49. [NPR, SRC]
McKee, M. and M. Suhrcke, 2005: Commentary: health and economic transition. Int. J. Epidemiol., 34, 1203-1206. Clean
McLaughlin, J.B., A. DePaola, C.A. Bopp, K.A. Martinek, N.P. Napolilli, C.G. Allison, S.L. Murray, E.C. Thompson, M.M. Bird and J.P. Middaugh, 2005: Outbreak of Vibrio parahaemolyticus gastroenteritis associated with Alaskan oysters. New Engl. J. Med., 353, 1463-1470. Clean
McMichael, A., 2004: Climate change. Comparative Quantification of Health Risks: Global and Regional Burden of Disease due to Selected Major Risk Factors, Vol. 2, M. Ezzati, A. Lopez, A. Rodgers and C. Murray, Eds., World Health Organization, Geneva, 1543-1649. [NPR, SRC]
McMichael, A., A. Githeko, R. Akhtar, R. Carcavallo, D.J. Gubler, A. Haines, R.S. Kovats, P. Martens, J. Patz, A. Sasaki, K. Ebi, D. Focks, L.S. Kalkstein, E. Lindgren, L.R. Lindsay and R. Sturrock, 2001: Human population health. Climate Change 2001: Impacts, Adaptation, and Vulnerability. Contribution of Working Group II to the Third Assessment Report of the Intergovernmental Panel on Climate Change, J.J. McCarthy, O.F. Canziani, N.A. Leary, D.J. Dokken and K.S. White, Eds., Cambridge University Press, Cambridge, 453-485. [NPR, SRC]
McMichael, A.J., D. Campbell-Lendrum, C. Corvalan, K. Ebi, A. Githeko, J. Scheraga and A. Woodward, Eds., 2003a: Climate Change and Human Health: Risk and Responses. World Health Organization, Geneva, 333 pp. [NPR, SRC]
McMichael, A.J., R. Woodruff, P. Whetton, K. Hennessy, N. Nicholls, S. Hales, A. Woodward and T. Kjellstrom, 2003b: Human Health and Climate Change in Oceania: Risk Assessment 2002. Department of Health and Ageing, Canberra, 128 pp. [NPR, SRC]
McMichael, A.J., M. McKee, V. Shkolnikov and T. Valkonen, 2004: Mortality trends and setbacks: global convergence or divergence? Lancet, 363, 1155-1159. [SRC]
McMichael, A.J., R.E. Woodruff and S. Hales, 2006: Climate change and human health: present and future risks. Lancet, 367, 859-869. [MoS, SRC]
Meehl, G.A. and C. Tebaldi, 2004: More intense, more frequent and longer lasting heat waves in the 21st century. Nature, 305, 994-997. [JoC, ARC]
Meehl, G.A., T.F. Stocker, W.D. Collins, P. Friedlingstein, A.T. Gaye, J.M. Gregory, A. Kitoh, R. Knutti, J.M. Murphy, A. Noda, S.C.B. Raper, I.G. Watterson, A.J. Weaver and Z.-C. Zhao, 2007: Global climate projections. Climate Change 2007: The Physical Science Basis. Contribution of Working Group I to the Fourth Assessment Report of the Intergovernmental Panel on Climate Change, S. Solomon, D. Qin, M. Manning, Z. Chen, M. Marquis, K.B. Averyt, M. Tignor and H.L. Miller, Eds., Cambridge University Press, Cambridge, 747-846. [NPR, ARC, 2007]
Menne, B., 2000: Floods and public health consequences, prevention and control measures. UN 2000 (MP.WAT/SEM.2/1999/22). [NPR, SRC]
Menne, B. and R. Bertollini, 2000: The health impacts of desertification and drought. Down to Earth, 14, 4-6. [SRC]
Menne, B. and R. Bertollini, 2005: Health and climate change: a call for action. Brit. Med. J., 331, 1283-1284. [SRC]
Michelon, T., P. Magne and F. Simon-Delavelle, 2005: Lessons from the 2003 heat wave in France and action taken to limit the effects of future heat wave. Extreme Weather Events and Public Health Responses, W. Kirch, B. Menne and R. Bertolllini, Eds., Springer, Berlin, 131-140. [NPR]
Michelozzi, P., F. de Donato, G. Accetta, F. Forastiere, M. D’Ovido and L.S. Kalkstein, 2004: Impact of heat waves on mortality: Rome, Italy, June–August 2003. J. Am. Med. Assoc., 291, 2537-2538. Clean
Michelozzi, P., F. de Donato, L. Bisanti, A. Russo, E. Cadum, M. Demaria, M. D’Ovidio, G. Costa and C. Perucci, 2005: The impact of the summer 2003 heat waves on mortality in four Italian cities. EuroSurveillance, 10, 161-165. Clean
Mickley, L.J., D.J. Jacob, B.D. Field and D. Rind, 2004: Effects of future climate change on regional air pollution episodes in the United States. Geophys. Res. Lett., 30, L24103. [JoC, MoS]
Miettinen, I.T., O. Zacheus, C.H. von Bonsdorff and T. Vartiainen, 2001: Waterborne epidemics in Finland in 1998-1999. Water Sci. Technol., 43, 67-71. Clean
Millennium Ecosystem Assessment, 2005: Ecosystems and Human Well-Being: Scenarios. Findings of the Scenarios Working Group Millennium Ecosystem Assessment Series, Island Press, Washington, District of Columbia, 515 pp. [NPR]
Ministry of Environment and Forest and Government of India, 2004: India’s Initial National Communication to the United National Framework Convention on Climate Change. Government of India, New Delhi, 292 pp. [NPR]
Mohan, J.E., L.H. Ziska, W.H. Schlesinger, R.B. Thomas, R.C. Sicher, K. George and J.S. Clark, 2006: Biomass and toxicity responses of poison ivy (Toxicodendron radicans) to elevated atmospheric CO2. P. Natl. Acad. Sci. USA, 103, 9086-9089. [JoC]
Mohanty, P. and U. Panda, 2003: Heatwave in Orissa: A Study Based on Heat Indices and Synoptic Features – Heatwave Conditions in Orissa. Regional Research Laboratory, Institute of Mathematics and Applications, Bubaneshwar, 15 pp. [NPR]
Molesworth, A.M., M.H. Djingary and M.C. Thomson, 2001: Seasonality in meningococcal disease in Niger, West Africa: a preliminary investigation. GEOMED 1999, Paris. Elsevier, 92-97. [NPR, SRC]
Molesworth, A.M., L.E. Cuevas, A.P. Morse, J.R. Herman and M.C. Thomson, 2002a: Dust clouds and spread of infection. Lancet, 359, 81-82. [SRC]
Molesworth, A.M., M.C. Thomson, S.J. Connor, M.P. Cresswell, A.P. Morse, P. Shears, C.A. Hart and L.E. Cuevas, 2002b: Where is the meningitis belt? Defining an area at risk of epidemic meningitis in Africa. T. Roy. Soc. Trop. Med. H., 96, 242-249. [SRC]
Molesworth, A.M., L.E. Cuevas, S.J. Connor, A.P. Morse and M.C. Thomson, 2003: Environmental risk and meningitis epidemics in Africa. Emerg. Infect. Dis., 9, 1287-1293. [SRC]
Mollica, R.F., B.L. Cardozo, H. Osofsky, B. Raphael, A. Ager and P. Salama, 2004: Mental health in complex emergencies. Lancet, 364, 2058-2067. Clean
Mondal, N., M. Biswas and A. Manna, 2001: Risk factors of diarrhoea among flood victims: a controlled epidemiological study. Indian J. Public Health, 45, 122-127. Clean
Moore, D., R. Copes, R. Fisk, R. Joy, K. Chan and M. Brauer, 2006: Population health effects of air quality changes due to forest fires in British Columbia in 2003: Estimates from physician-visit billing data. Can. J. Public Health, 97, 105-108. [MoS]
Moore, J.E., D. Gilpin, E. Crothers, A. Canney, A. Kaneko and M. Matsuda, 2002: Occurrence of Campylobacter spp. and Cryptosporidium spp. in seagulls (Larus spp.). Vector-Borne Zoonot., 2, 111-114. Clean
Moore, K., A. Clarke, V. Kapustin and S. Howell, 2003: Long-range transport of continental plumes over the Pacific Basin: aerosol physiochemistry and optical properties during PEM-Tropics A and B. J. Geophys. Res. D, 108, 8236. Clean
Moreno, J., 2005: A preliminary assessment of the impacts in Spain due to the effects of climate change. ECCE Project Final Report. Universidad de Castilla-La Mancha, Ministry of the Environment, Madrid, 741 pp. [NPR, ARC]
Morris, C.J.G. and I. Simmonds, 2000: Associations between varying magnitudes of the urban heat island and the synoptic climatology in Melbourne, Australia. Int. J. Climatol., 20, 1931-1954. [JoC]
Mott, J.A., D.M. Mannino, C.J. Alverson, A. Kiyu, J. Hashim, T. Lee, K. Falter and S.C. Redd, 2005: Cardiorespiratory hospitalizations associated with smoke exposure during the 1997 Southeast Asian forest fires. Int. J. Hyg. Envir. Heal., 208, 75-85. Clean
Mouchet, J., O. Faye, J. Juivez and S. Manguin, 1996: Drought and malaria retreat in the Sahel, West Africa. Lancet, 348, 1735-1736. Clean
Mudway, I.S. and F.J. Kelly, 2000: Ozone and the lung: a sensitive issue. Mol. Aspects Med., 21, 1-48. Clean
Murano, K., H. Mukai, S. Hatakeyama, E. Jang and I. Uno, 2000: Trans-boundary air pollution over remote islands in Japan: observed data and estimates from a numerical model. Atmos. Environ., 34, 5139-5149. [MoS]
Mutero, C.M., C. Kabutha, V. Kimani, L. Kabuage, G. Gitau, J. Ssennyonga, J. Githure, L. Muthami, A. Kaida, L. Musyoka, E. Kiarie and M. Oganda, 2004: A transdisciplinary perspective on the links between malaria and agroecosystems in Kenya. Acta Trop., 89, 171-186. Clean
Nagendra, S. and M. Khare, 2003: Diurnal and seasonal variations of carbon monoxide and nitrogen dioxide in Delhi city. Int. J. Environ. Pollut., 19, 75-96. Clean
Nakićenović, N. and R. Swart, Eds., 2000: Special Report on Emissions Scenarios: A Special Report of Working Group III of the Intergovernmental Panel on Climate Change. Cambridge University Press, Cambridge, 599 pp. [NPR]
National Environment Commission, Royal Government of Bhutan, UNDP and GEF, 2006: Bhutan National Adaptation Programme of Action. National Environment Commission, Royal Government of Bhutan, Thimphu, 95 pp. [NPR]
Nayha, S., 2005: Environmental temperature and mortality. Int. J. Circumpolar Health, 64, 451-458. Clean
Nchito, M., P. Kelly, S. Sianongo, N.P. Luo, R. Feldman, M. Farthing and K.S. Baboo, 1998: Cryptosporidiosis in urban Zambian children: an analysis of risk factors. Am. J. Trop. Med. Hyg., 59, 435-437. Clean
Ndiaye, O., J.Y. Hesran, J.F. Etard, A. Diallo, F. Simondon, M.N. Ward and V. Robert, 2001: Climate variability and number of deaths at attributable to malaria in Niakhar area, Senegal, from 1984 to 1996 (in French). Santé, 11, 25-33. Clean
Nicholls, N., C. Butler and I. Hanigan, 2005: Inter-annual rainfall variations and suicide in New South Wales, Australia, 1964 to 2001. Int. J. Biometeorol., 50, 139-143. Clean
Nicholls, R.J., 2003: An expert assessment of storm surge “hotspots”. Interim Report to Center for Hazards and Risk Research, Lamont-Doherty Observatory, Columbia University. Flood Hazard Research Centre, University of Middlesex, London, 10 pp. [NPR, ARC]
Nicholls, R.J., 2004: Coastal flooding and wetland loss in the 21st century: changes under the SRES climate and socio-economic scenarios. Global Environ. Chang., 14, 69-86. [JoC, ARC]
Nickels, S., C. Furgal and J. Castleden, 2003: Putting the human face on climate change through community workshops: Inuit knowledge, partnerships and research. The Earth is Faster Now: Indigenous Observations of Arctic Environmental Change, I. Krupnik and D. Jolly, Eds., Arctic Studies Centre, Smithsonian Institution, Washington, District of Columbia, 300-344. [NPR, SRC]
Nilsson, E., J. Paatero and M. Boy, 2001a: Effects of air masses and synoptic weather on aerosol formation in the continental boundary layer. Tellus B, 53, 462-478. Clean
Nilsson, E., U. Rannik, M. Kulmala and G. Buzorius, 2001b: Effects of continental boundary layer evolution, convection, turbulence and entrainment, on aerosol formation. Tellus B, 53, 441-461. Clean
Niskanen, T., J. Waldenstrom, M. Fredriksson-Ahomaa, B. Olsen and H. Korkeala, 2003: virF-positive Yersinia pseudotuberculosis and Yersinia enterocolitica found in migratory birds in Sweden. Appl. Environ. Microbiol., 69, 4670-4675. Clean
Nordhaus, W.D., 1991: To slow or not to slow: the economics of the greenhouse effect. Econ. J., 101, 920-937. Clean
Nordhaus, W.D. and J. Boyer, 2000: Warming the World: Economic Models of Global Warming. MIT Press, Cambridge, Massachusetts, 246 pp. [NPR, MoS]
Norris, F.H., A.D. Murphy, C.K. Baker and J.L. Perilla, 2004: Postdisaster PTSD over four waves of a panel study of Mexico’s 1999 flood. J. Trauma. Stress, 17, 283-292. Clean
North, C.S., A. Kawasaki, E.L. Spitznagel and B.A. Hong, 2004: The course of PTSD, major depression, substance abuse, and somatization after a natural disaster. J. Nerv. Ment. Dis., 192, 823-829. Clean
Obiri-Danso, K., N. Paul and K. Jones, 2001: The effects of UVB and temperature on the survival of natural populations and pure cultures of Campylobacter jejuni, Camp. coli, Camp. lari and urease-positive thermophilic campylobacters (UPTC) in surface waters. J. Appl. Microbiol., 90, 256-267. Clean
OCHA, 2003: India: Heat Wave – Occurred: 20 May 2003–5 June 2003. OCHA Situation Report No.1. http://cidi.org/disaster/03a/ixl131.html. [NPR]
Ogden, N.H., A. Maarouf, I.K. Barker, M. Bigras-Poulin, L.R. Lindsay, M.G. Morshed, C.J. O’Callaghan, F. Ramay, D. Waltner-Toews and D.F. Charron, 2006: Climate change and the potential for range expansion of the Lyme disease vector Ixodes scapularis in Canada. Int. J. Parasitol., 36, 63-70. Clean
Ohl, C.A. and S. Tapsell, 2000: Flooding and human health. Brit. Med. J., 321, 1167-1168. Clean
Olmos, S., 2001: Vulnerability and adaptation to climate change: concepts, issues, assessment methods. Climate Change Knowledge Network Foundation Paper, Oslo, 20 pp. [NPR]
Olsen, B., D.C. Duffy, T.G.T. Jaenson, A. Gylfe, J. Bonnedahl and S. Bergstrom, 1995: Transhemispheric exchange of Lyme-disease spirochetes by seabirds. J. Clin. Microbiol., 33, 3270-3274. Clean
Olshansky, S.J., B.A. Carnes and C. Cassel, 1998: The future of long life. Science, 281, 1612-3, 1613-1615. [JoC, MoS]
Pal Arya, S., 2000: Air pollution meteorology and dispersion. Bound.-Lay. Meteorol., 94, 171-172. Clean
Pardue, J., W. Moe, D. McInnis, L. Thibodeaux, K. Valsaraj, E. Maciasz, I. van Heerden, N. Korevec and Q. Yuan, 2005: Chemical and microbiological parameters in New Orleans floodwater following Hurricane Katrina. Environ. Sci. Technol., 39, 8591-8599. Clean
Parkinson, A.J. and J.C. Butler, 2005: Potential impacts of climate change on infectious diseases in the Arctic. Int. J. Circumpolar Health, 64, 478-486. Clean
Parmesan, C. and G. Yohe, 2003: A globally coherent fingerprint of climate change impacts across natural systems. Nature, 421, 37-42. [JoC, ARC]
Pascual, M., X. Rodo, S.P. Ellner, R. Colwell and M.J. Bouma, 2000: Cholera dynamics and El Niño Southern Oscillation. Science, 289, 1766-1767. [JoC, ARC]
Pascual, M., J.A. Ahumada, L.F. Chaves, X. Rodo and M. Bouma, 2006: Malaria resurgence in the East African highlands: temperature trends revisited. P. Natl. Acad. Sci. USA, 103, 5829-5834. [JoC, ARC]
Pattenden, S., B. Nikiforov and B.G. Armstrong, 2003: Mortality and temperature in Sofia and London. J. Epidemiol. Commun. H., 57, 628-633. Clean
Patz, J.A., 2002: A human disease indicator for the effects of recent global climate change. P. Natl. Acad. Sci. USA, 99, 12506-12508. [JoC, ARC]
Pejoch, M. and B. Kriz, 2006: Ecology, epidemiology and prevention of Hantavirus in Europe. Climate Change and Adaptation Strategies for Human Health, B. Menne and K.L. Ebi, Eds., Steinkopff, Darmstadt, 243-265. [NPR]
People’s Health Movement, Medact, Global Equity Gauge Alliance and Zed Books, 2005: Global Health Watch 2005–2006: An Alternative World Health Report. London and New York, 368 pp. [NPR]
Peperzak, L., 2005: Future increase in harmful algal blooms in the North Sea due to climate change. Water Sci. Technol., 51, 31. [MoS]
Pereira, L.E., A. Suzuki, T. Lisieux, M. Coimbra, R.P. de Souza and E.L.B. Chamelet, 2001: Ilheus arbovirus in wild birds (Sporophila caerulescens and Molothrus bonariensis). Rev. Saude Publ., 35, 119-123. Clean
Pitcher, H., K. Ebi and A. Brenkert, 2007: Population health model for integrated assessment models. Climatic Change. doi: 10.1007/s10584-007-9286-8. [NPR, SRC, 2007]
Pontes, R.J., J. Freeman, J.W. Oliveira-Lima, J.C. Hodgson and A. Spielman, 2000: Vector densities that potentiate dengue outbreaks in a Brazilian city. Am. J. Trop. Med. Hyg., 62, 378-383. Clean
Pope, C.A., R.T. Burnett, M.J. Thun, E.E. Calle, D. Krewski, K. Ito and G.D. Thurston, 2002: Lung cancer, cardiopulmonary mortality, and long-term exposure to fine particulate air pollution. J. Am. Med. Assoc., 287, 1132-1141. Clean
Prather, M., M. Gauss, T. Berntsen, I. Isaksen, J. Sundet, I. Bey, G. Brasseur, F. Dentener, R. Derwent, D. Stevenson, L. Grenfell, D. Hauglustaine, L. Horowitz, D. Jacob, L. Mickley, M. Lawrence, R. von Kuhlmann, J.-F. Muller, G. Pitari, H. Rogers, M. Johnson, J. Pyle, K. Law, M. van Weele and O. Wild, 2003: Fresh air in the 21st century? Geophys. Res. Lett., 30, 1100. [JoC]
Programa Nacional de Cambios Climaticos Componente Salud, Viceministerio de Medio Ambiente and Recursos Naturales y Desarrollo Forestal, 2000: Vulnerabilidad y adaptacion de al salud humana ante los efectos del cambio climatico en Bolivia [Vulnerability and Adaptation to Protect Human Health from Effects of Climate Change in Bolivia]. Programa Nacional de Cambios Climaticos Componente Salud, Viceministerio de Medio Ambiente, Recursos Naturales y Desarrollo Forestal, 111 pp. [NPR]
Prospero, J.M., E. Blades, G. Mathison and R. Naidu, 2005: Interhemispheric transport of viable fungi and bacteria from Africa to the Caribbean with soil dust. Aerobiologia, 21, 1-19. Clean
Prüss-Üstün, A., H. Zeeb, C. Mathers and M. Repacholi, Eds., 2006: Solar Ultraviolet Radiation: Global Burden of Disease from Ultraviolet Radiation. Environmental Burden of Disease Series, Vol. 13. World Health Organization, Geneva, 285 pp. [NPR]
Qiu, D., T. Tanihata, H. Aoyama, T. Fujita, Y. Inaba and M. Minowa, 2002: Relationship between a high mortality rate and extreme heat during the summer of 1999 in Hokkaido Prefecture, Japan. J. Epidemiol., 12, 254-257. Clean
Ramsey, J., 1995: Task performance in heat: a review. Ergonomics, 38, 154-165. Clean
Ramsey, J., C. Burford, M. Beshir and R. Hensen, 1983: Effects of workplace thermal conditions on safe working behavior. J. Safety Res., 14, 105-114. Clean
Randolph, S.E., 2001: The shifting landscape of tick-borne zoonoses: tick-borne encephalitis and Lyme borreliosis in Europe. Philos. T. Roy. Soc. Lond. B, 356, 1045-1056. Clean
Randolph, S.E., 2004: Evidence that climate change has caused ‘emergence’ of tick-borne diseases in Europe? Int. J. Med. Microbiol., 293, S5-S15. Clean
Randolph, S.E. and D.J. Rogers, 2000: Fragile transmission cycles of tick-borne encephalitis virus may be disrupted by predicted climate change. Philos. T. Roy. Soc. Lond. B, 267, 1741-1744. [MoS]
Ranhoff, A.H., 2000: Accidental hypothermia in the elderly. Int. J. Circumpolar Health, 59, 255-259. Clean
Rao, S., J. Ku, S. Berman, D. Zhang and H. Mao, 2003: Summertime characteristics of the atmospheric boundary layer and relationships to ozone levels over the eastern United States. Pure Appl. Geophys., 160, 21-55. Clean
Rappengluck, B., P. Oyola, I. Olaeta and P. Fabian, 2000: The evolution of photochemical smog in the Metropolitan Area of Santiago de Chile. J. Appl. Meteorol., 39, 275-290. Clean
Rappole, J.H. and Z. Hubalek, 2003: Migratory birds and West Nile virus. J. Appl. Microbiol., 94, 47S-58S. Clean
Reacher, M., K. McKenzie, C. Lane, T. Nichols, I. Kedge, A. Iverson, P. Hepple, T. Walter, C. Laxton and J. Simpson, 2004: Health impacts of flooding in Lewes: a comparison of reported gastrointestinal and other illness and mental health in flooded and non flooded households. Communicable Disease and Public Health, 7, 1-8. Clean
Reed, K.D., J.K. Meece, J.S. Henkel and S.K. Shukla, 2003: Birds, migration and emerging zoonoses: West Nile virus, Lyme disease, influenza A and enteropathogens. Clin. Med. Res., 1, 5-12. Clean
Regidor, E., 2004a: Measures of health inequalities: part 2. J. Epidemiol. Commun. H., 58, 900-903. Clean
Regidor, E., 2004b: Measures of health inequalities: part 1. J. Epidemiol. Commun. H., 58, 858-861. Clean
Reiter, P., C.J. Thomas, P. Atkinson, S.E. Randolph, D.J. Rogers, G.D. Shanks, R.W. Snow and A. Spielman, 2004: Global warming and malaria: a call for accuracy. Lancet Infect. Dis., 4, 323. Clean
Riedel, D., 2004: Human health and well-being. Climate Change: Impacts and Adaptation A – Canadian Perspective, D. Lemmen and F. Warren, Eds., Climate Change Impacts and Adaptation Directorate, Natural Resources Canada, Ottawa, 151-171. [NPR]
Rockstrom, J., 2003: Water for food and nature in drought-prone tropics: vapour shift in rain-fed agriculture. Philos. T. Roy. Soc. Lond. B, 358, 1997-2009. Clean
Rodo, X., M. Pascual, G. Fuchs and A.S.G. Faruque, 2002: ENSO and cholera: a nonstationary link related to climate change? P. Natl. Acad. Sci. USA, 99, 12901-12906. [JoC, ARC]
Rogers, C., P. Wayne, E. Macklin, M. Muilenberg, C. Wagner, P. Epstein and F. Bazzaz, 2006a: Interaction of the onset of spring and elevated atmospheric CO2 on ragweed (Ambrosia artemisiifolia L.) pollen production. Environ. Health Persp., 114, 865-869. doi:10.1289/ehp.8549. Clean
Rogers, D.J. and S.E. Randolph, 2000: The global spread of malaria in a future, warmer world. Science, 289, 1763-1765. [JoC, MoS]
Rogers, D.J. and S.E. Randolph, 2006: Climate change and vector-borne diseases. Adv. Parasitol., 62, 345-381. Clean
Rogers, D.J., A.J. Wilson, S.I. Hay and A.J. Graham, 2006b: The global distribution of yellow fever and dengue. Adv. Parasitol., 62, 181-220. Clean
Rosegrant, M.W. and S.A. Cline, 2003: Global food security: challenges and policies. Science, 302, 1917-1919. [JoC]
Ryall, D.B., R.G. Derwent, A.J. Manning, A.L. Redington, J. Corden, W. Millington, P.G. Simmonds, S. O’Doherty, N. Carslaw and G.W. Fuller, 2002: The origin of high particulate concentrations over the United Kingdom, March 2000. Atmos. Environ., 36, 1363-1378. Clean
Rybnicek, O. and S. Jaeger, 2001: Ambrosia (ragweed) in Europe. ACI International, 13, 60-66. Clean
Sachs, J., 2001: Macroeconomics and Health: Investing in Health for Economic Development. Report of the Commission on Macro Economics and Health, World Health Organization, Geneva, 208 pp. [NPR]
Samanek, A.J., E.J. Croager, P. Giesfor, E. Milne, R. Prince, A.J. McMichael, R.M. Lucas and T. Slevin, 2006: Estimates of beneficial and harmful sun exposure times during the year for major Australian population centres. Med. J. Australia, 184, 338-341. [MoS, SRC]
Samarasinghe, J., 2001: Heat stroke in young adults. Trop. Doct., 31, 217-219. Clean
Sapkota, A., J.M. Symons, J. Kleissl, L. Wang, M.B. Parlange, J. Ondov, P.N. Breysse, G.B. Diette, P.A. Eggleston and T.J. Buckley, 2005: Impact of the 2002 Canadian forest fires on particulate matter air quality in Baltimore city. Environ. Sci. Technol., 39, 24-32. Clean
Sarkar, U., S.F. Nascimento, R. Barbosa, R. Martins, H. Nuevo, I. Kalafanos, I. Grunstein, B. Flannery, J. Dias, L.W. Riley, M.G. Reis and A.I. Ko, 2002: Population-based case-control investigation of risk factors for leptospirosis during an urban epidemic. Am. J. Trop. Med. Hyg., 66, 605-610. Clean
Sastry, N., 2002: Forest fires, air pollution, and mortality in Southeast Asia. Demography, 39, 1-23. Clean
Scheraga, J.S., K.L. Ebi, J. Furlow and A.R. Moreno, 2003: From science to policy: developing responses to climate change. Climate Change and Human Health: Risks and Responses, A. McMichael, D. Campbell-Lendrum, C. Corvalan, K.L. Ebi, A.K. Githeko, J.S. Scheraga and A. Woodward, Eds., World Health Organization, Geneva, 237-266. [NPR, SRC]
Schichtel, B. and R. Husar, 2001: Eastern North American transport climatology during high- and low-ozone days. Atmos. Environ., 35, 1029-1038. Clean
Schultz, J.M., J. Russell and Z. Espine, 2005: Epidemiology of tropical cyclones: the dynamics of disaster, disease and development. Epidemiol. Rev., 27, 21-35. Clean
Schwartz, B.S., J.B. Harris, A.I. Khan, R.C. Larocque, D.A. Sack, M.A. Malek, A.S. Faruque, F. Qadri, S.B. Calderwood, S.P. Luby and E.T. Ryan, 2006: Diarrheal epidemics in Dhaka, Bangladesh, during three consecutive floods: 1988, 1998, and 2004. Am. J. Trop. Med. Hyg., 74, 1067-1073. Clean
Schwartz, J. and R. Levin, 1999: Drinking water turbidity and health. Epidemiology, 10, 86-89. Clean
Schwartz, J., R. Levin and R. Goldstein, 2000: Drinking water turbidity and gastrointestinal illness in the elderly of Philadelphia. J. Epidemiol. Commun. H., 54, 45-51. Clean
Scott, G.M. and R.D. Diab, 2000: Forecasting air pollution potential: a synoptic climatological approach. J. Air Waste Manage., 50, 1831-1842. [MoS]
Semenov, S.M., E.S. Gelver and V.V. Yasyukevich, 2002: Temperature conditions for development of two species of malaria pathogens in Russia in 20th century. Dokl. Akad. Nauk, 387, 131-136. [ARC]
Sénat, 2004: La France et les Français face a la canicule: les leçons d’une crise [France and the French facing the heat wave: lessons from a crisis]. Rapport d’Information No. 195 (2003–2004) de Mme Letard, M.M. Flandre, S. Lepeltier, fait au nom de la mission commune d’information du Senat, depose le 3 Fevrier 2004. http://www.senat.fr/rap/r03-195/r03-1951.pdf. [NPR]
Senhorst, H.A. and J.J. Zwolsman, 2005: Climate change and effects on water quality: a first impression. Water Sci. Technol., 51, 53-59. Clean
Shah, I., G.C. Deshpande and P.N. Tardeja, 2004: Outbreak of dengue in Mumbai and predictive markers for dengue shock syndrome. J. Trop. Pediatrics, 50, 301-305. [MoS]
Shanks, G.D., S.I. Hay, D.I. Stern, K. Biomndo and R.W. Snow, 2002: Meteorologic influences on Plasmodium falciparum malaria in the highland tea estates of Kericho, Western Kenya. Emerg. Infect. Dis., 8, 1404-1408. Clean
Shanks, N. and G. Papworth, 2001: Environmental factors and heatstroke. Occup. Med., 51, 45-49. Clean
Shinn, E.A., D.W. Griffin and D.B. Seba, 2003: Atmospheric transport of mold spores in clouds of desert dust. Arch. Environ. Health, 58, 498-504. Clean
Sillett, T.S., R.T. Holmes and T.W. Sherry, 2000: Impacts of a global climate cycle on population dynamics of a migratory songbird. Science, 288, 2040-2042. [JoC]
Singer, B.D., L.H. Ziska, D.A. Frenz, D.E. Gebhard and J.G. Straka, 2005: Increasing Amb a 1 content in common ragweed (Ambrosia artemisiifolia) pollen as a function of rising atmospheric CO2 concentration. Funct. Plant Biol., 32, 667-670. Clean
Singh, N. and V.P. Sharma, 2002: Patterns of rainfall and malaria in Madhya Pradesh, central India. Ann. Trop. Med. Parasit., 965, 349-359. Clean
Singh, R., S. Hales, N. de Wet, R. Raj, M. Hearnden and P. Weinstein, 2001: The influence of climate variation and change on diarrhoeal disease in the pacific islands. Environ. Health Persp., 109, 155-159. [SRC]
Skarphedinsson, S., P.M. Jensen and K. Kristiansen, 2005: Survey of tick borne infections in Denmark. Emerg. Infect. Dis., 11, 1055-1061. Clean
Slanina, S. and Y. Zhang, 2004: Aerosols: connection between regional climate change and air quality. IUPAC Technical Report. Pure Appl. Chem., 76, 1241-1253. Clean
Small, C. and R.J. Nicholls, 2003: A global analysis of human settlement in coastal zones. J. Coastal Res., 19, 584-599. [ARC]
Smith, K.R., J. Zhang, R. Uma, V.V.N. Kishore and M.A.K. Khalil, 2000: Greenhouse implications of household fuels: an analysis for India. Annu. Rev. Energ. Env., 25, 741-763. [SRC]
Smith, K.R., S. Mehta and M. Maeusezahl-Feuz, 2004: Indoor air pollution from household use of solid fuels. Comparative Quantification of Health Risks: Global and Regional Burden of Disease Attributable to Selected Major Risk Factors, M. Ezzati, A.D. Lopez, A. Rodgers and C.J.L. Murray, Eds., World Health Organisation, Geneva, 1435-1494. [NPR, SRC]
Smith, K.R., J. Rogers and S.C. Cowlin, 2005: Household Fuels and Ill-Health in Developing Countries: What Improvements can be Brought by LP Gas? World LP Gas Association and Intermediate Technology Development Group, Paris, 59 pp. [NPR, SRC]
Socioambiental, 2006: Seca na Amazônia: alguma coisa está fora da ordem. http://www.socioambiental.org/nsa/detalhe?id=2123. [NPR]
Sorogin, V.P. and Co-authors, 1993: Problemy Ohrany Zdoroviya i Socialnye Aspecty Osvoeniya Gazovyh i Neftyanyh Mestorozhdenij v Arcticheskih Regionah [Problems of Public Health and Social Aspects of Exploration of Oil and Natural Gas Deposits in Arctic Regions]. Nadym. [NPR]
Sousounis, J., C. Scott and M. Wilson, 2002: Possible climate change impacts on ozone in the Great Lakes region: some implications for respiratory illness. J. Great Lakes Res., 28, 626-642. Clean
Speelmon, E.C., W. Checkley, R.H. Gilman, J. Patz, M. Calderon and S. Manga, 2000: Cholera incidence and El Niño-related higher ambient temperature. J. Am. Med. Assoc., 283, 3072-3074. [ARC]
Stapp, P., M. Antolin and M. Ball, 2004: Patterns of extinction in prairie dog metapopulations: plague outbreaks follow El Niño events. Front. Ecol. Environ., 2, 235-240. Clean
Steenvoorden, J. and T. Endreny, 2004: Wastewater Re-use and Groundwater quality. IAHS Publication 285, Wallingford, Oxfordshire, 112 pp. [NPR]
Stenseth, N., 2006: Plague dynamics are driven by climate variations. P. Natl. Acad. Sci. USA, 1003, 13110-13115. [JoC]
Stevenson, D.S., C.E. Johnson, W.J. Collins, R.G. Derwent and J.M. Edwards, 2000: Future estimates of tropospheric ozone radiative forcing and methane turnover: the impact of climate change. Geophys. Res. Lett., 27, 2073-2076. [JoC, MoS]
Stohl, A., L. Haimberger, M. Scheele and H. Wernli, 2001: An intercomparison of results from three trajectory models. Meteorol. Appl., 8, 127-135. [MoS]
Suh, H.H., T. Bahadori, J. Vallarino and J.D. Spengler, 2000: Criteria air pollutants and toxic air pollutants. Environ. Health Persp., 108, 625-633. Clean
Sultan, B., K. Labadi, J.F. Guegan and S. Janicot, 2005: Climate drives the meningitis epidemics onset in west Africa. PLoS Med., 2, e6. doi: 10.1371/journal. pmed.0020006 Clean
Sumilo, D., A. Bormane, L. Asokliene, I. Lucenko, V. Vasilenko and S. Randolph, 2006: Tick-borne encephalitis in the Baltic States: identifying risk factors in space and time. Int. J. Med. Microbiol., 296, 76-79. Clean
Sur, D., P. Dutta, G.B. Nair and S.K. Bhattacharya, 2000: Severe cholera outbreak following floods in a northern district of West Bengal. Indian J. Med. Res., 112, 178-182. Clean
Sutherst, R.W., 2004: Global change and human vulnerability to vector-borne diseases. Clin. Microbiol. Rev., 17, 136. Clean
Syri, S., N. Karvosenoja, A. Lehtila, T. Laurila, V. Lindfors and J.P. Tuovinen, 2002: Modeling the impacts of the Finnish Climate Strategy on air pollution. Atmos. Environ., 36, 3059-3069. [MoS]
Szreter, S., 2004: Industrialization and health. Brit. Med. Bull., 69, 75-86. Clean
Taha, H., 2001: Potential Impacts of Climate Change on Tropospheric Ozone in California: A Preliminary Episodic Modeling Assessment of the Los Angeles Basin and the Sacramento Valley. Lawrence Berkeley National Laboratories, Berkeley, California, 39 pp. [NPR, MoS]
Takemura, T., T. Nakajima, T. Nozawa and K. Aoki, 2001: Simulation of future aerosol distribution, radioactive forcing, and long-range transport in East Asia. J. Meteorol. Soc. Jpn., 79, 1139-1155. [MoS]
Tam, C., L. Rodrigues, S. O’Brien and S. Hajat, 2006: Temperature dependence of reported Campylobacter infection in England, 1989–1999. Epidemiol. Infect., 134, 119-125. Clean
Tanner, P. and P. Law, 2002: Effects of synoptic weather systems upon the air quality in an Asian megacity. Water Air Soil Pollut, 136, 105-124. Clean
Tanser, F.C., B. Sharp and D. Le Sueur, 2003: Potential effect of climate change on malaria transmission in Africa. Lancet Infect. Dis., 362, 1792-1798. Clean
Tapsell, S., E. Penning-Rowsell, S. Tunstall and T. Wilson, 2002: Vulnerability to flooding: health and social dimensions. Philos. T. Roy. Soc. Lond. A, 360, 1511-1525. Clean
Taramarcaz, P., B. Lambelet, B. Clot, C. Keimer and C. Hauser, 2005: Ragweed (Ambrosia) progression and its health risks: will Switzerland resist this invasion? Swiss Med. Wkly., 135, 538-548. [SRC]
Teklehaimanot, H., J. Schwartz, A. Teklehaimanot and A. Lipsitch, 2004: Weather-based prediction of Plasmodium falciparum malaria in epidemic-prone regions of Ethiopia. Malaria J., 3. [NPR, MoS]
Thomas, C.J., G. Davies and C.E. Dunn, 2004: Mixed picture for changes in stable malaria distribution with future climate in Africa. Trends Parasitol., 20, 216-220. [MoS]
Thommen Dombois, O. and C. Braun-Fahrlaender, 2004: Gesundheitliche Auswirkungen der Klimaaenderung mit Relevanz fuer die Schweiz [Health Impacts of Climate Change with Relevance for Switzerland]. Insititut fuer Sozial- und Preventivmedizin der Universitaet Basel, Bundesamt fuer Gesundheit, Bundesamt fuer Umwelt, Wald und Landschaft, Basel, 85 pp. [NPR]
Thomson, M.C., S.J. Mason, T. Phindela and S.J. Connor, 2005: Use of rainfall and sea surface temperature monitoring for malaria early warning in Botswana. Am. J. Trop. Med. Hyg., 73, 214-221. [SRC]
Thomson, M.C., F.J. Doblas-Reyes, S.J. Mason, R. Hagedorn, S.J. Connor, T. Phindela, A.P. Morse and T.N. Palmer, 2006: Malaria early warnings based on seasonal climate forecasts from multi-model ensembles. Nature, 439, 576-579. [JoC, MoS, SRC]
Tol, R.S., 1995: The damage costs of climate change toward more comprehensive calculations. Environ. Resour. Econ., 5, 353-374. Clean
Tol, R.S., 1996: The damage costs of climate change towards a dynamic representation. Ecol. Econ., 19, 67-90. Clean
Tol, R.S., 2002a: Estimates of the damage costs of climate change. Part II. Dynamic estimates. Environ. Resour. Econ., 21, 135-160. [MoS]
Tol, R.S., 2002b: Estimates of the damage costs of climate change. Part I. Benchmark estimates. Environ. Resour. Econ., 21, 47-73. [MoS]
Tu, F., D. Thornton, A. Brandy and G. Carmichael, 2004: Long-range transport of sulphur dioxide in the central Pacific. J. Geophys. Res. D, 109, D15S08. Clean
Turpie, J., H. Winkler, R. Spalding-Fecher and G. Midgley, 2002: Economic Impacts of Climate Change in South Africa: A Preliminary Analysis of Unmitigated Costs. Southern Waters Ecological Research and Consulting, Energy and Development Research Centre, University of Cape Town, Cape Town, 64 pp. [NPR, ARC]
Tuyet, D.T., V.D. Thiem, L. Von Seidlein, A. Chowdhury, E. Park, D.G. Canh, B.T. Chien, T. Van Tung, A. Naficy, M.R. Rao, M. Ali, H. Lee, T.H. Sy, M. Nichibuchi, J. Clemens and D.D. Trach, 2002: Clinical, epidemiological, and socioeconomic analysis of an outbreak of Vibrio parahaemolyticus in Khanh Hoa Province, Vietnam. J. Infect. Dis., 186, 1615-1620. Clean
UN, 2000: Convention on the Protection and Use of Transboundary Watercourses and International Lakes. 32 pp. http://www.unece.org/env?/water/pdf/ watercon.pdf. [NPR]
UN, 2006a: The Millennium Development Goals Report 2006. United Nations Department of Economic and Social Affairs, DESA, New York, 32 pp. [NPR]
UN, 2006b: Executive summary, fact sheets, data tables. World Urbanization Prospects: The 2005 Revision. United Nations, New York, 210 pp. [NPR]
UN Millennium Project, 2005: Investing in Development: A Practical Plan to Achieve the Millennium Development Goals. Earthscan, London, 329 pp. [NPR]
UNDP, 2005: World Population Prospects: The 2004 Revision. III. UNDP, New York, 105 pp. [NPR]
UNEP, 2002: Synthesis GEO-3: Global Environmental Outlook 3. United Nations Environment Programme. Earthscan, London, 20 pp. [NPR]
UNEP and WCMC, 2002: Human Development Report 2002: Deepening Democracy in a Fragmented World. Oxford University Press, New York and Oxford, 276 pp. [NPR]
United Nations World Water Assessment Programme, 2003: Water for People: Water for Life. United Nations World Water Development Report. United Nations Educational Scientific and Cultural Organization (UNESCO), Berghan Books, Barcelona, 529 pp. [NPR]
Unsworth, J., R. Wauchope, A. Klein, E. Dorn, B. Zeeh, S. Yeh, M. Akerblom, K. Racke and B. Rubin, 2003: Significance of the long range transport of pesticides in the atmosphere. Pest. Manag. Sci., 58, 314. Clean
van der Pligt, J., E.C.M. van Schie and R. Hoevenagel, 1998: Understanding and valuing environmental issues: the effects of availability and anchoring on judgment. Z. Exp. Psychol., 45, 286-302. Clean
van Lieshout, M., R.S. Kovats, M.T.J. Livermore and P. Martens, 2004: Climate change and malaria: analysis of the SRES climate and socio-economic scenarios. Global Environ. Chang., 14, 87-99. [JoC]
Vanasco, N.B., S. Fusco, J.C. Zanuttini, S. Manattini, M.L. Dalla Fontana, J. Prez, D. Cerrano and M.D. Sequeira, 2002: Human leptospirosis outbreak after an inundation at Reconquista (Santa Fe), 1998 (in Spanish). Rev. Argent. Microbiol., 34, 124. Clean
Vandentorren, S. and P. Empereur-Bissonnet, 2005: Health impact of the 2003 heat-wave in France. Extreme Weather Events and Public Health Responses, W. Kirch, B. Menne and R. Bertollini, Eds., Springer, 81-88. [NPR]
Vandentorren, S., F. Suzan, S. Medina, M. Pascal, A. Maulpoix, J.-C. Cohen and M. Ledrans, 2004: Mortality in 13 French cities during the August 2003 heatwave. Am. J. Public Health, 94, 1518-1520. Clean
Vapalahti, O., J. Mustonen, A. Lundkvist, H. Henttonen, A. Plyusnin and A. Vaheri, 2003: Hantavirus infections in Europe. Lancet Infect. Dis., 3, 653-661. Clean
Vasilev, V., 2003: Variability of Shigella flexneri serotypes during a period in Israel, 2000–2001. Epidemiol. Infect., 132, 51-56. Clean
Viscusi, W.K. and J.E. Aldy, 2003: The value of a statistical life: a critical review of market estimates throughout the world. J. Risk Uncertainty, 27, 5-76. [MoS]
Visser, M.E., C. Both and M.M. Lambrechts, 2004: Global climate change leads to mistimed avian reproduction. Adv. Ecol. Res., 35, 89-110. Clean
Vollaard, A.M., S. Ali, H.A.G.H. van Asten, S. Widjaja, L.G. Visser, C. Surjadi and J.T. van Dissel, 2004: Risk factors for typhoid and paratyphoid fever in Jakarta, Indonesia. J. Am. Med. Assoc., 291, 2607-2615. Clean
Voltolini, S., P. Minale, C. Troise, D. Bignardi, P. Modena, D. Arobba and A. Negrini, 2000: Trend of herbaceous pollen diffusion and allergic sensitisation in Genoa, Italy. Aerobiologia, 16, 245-249. Clean
Wade, T.J., S.K. Sandhu, D. Levy, S. Lee, M.W. LeChevallier, L. Katz and J.M. Colford, 2004: Did a severe flood in the Midwest cause an increase in the incidence of gastrointestinal symptoms? Am. J. Epidemiol., 159, 398-405. Clean
Wan, S.Q., T. Yuan, S. Bowdish, L. Wallace, S.D. Russell and Y.Q. Luo, 2002: Response of an allergenic species Ambrosia psilostachya (Asteraceae), to experimental warming and clipping: implications for public health. Am. J. Bot. 89, 1843-1846. Clean
Wayne, P., S. Foster, J. Connolly, F. Bazzaz and P. Epstein, 2002: Production of allergenic pollen by ragweed (Ambrosia artemisiifolia L.) is increased in CO2-enriched atmospheres. Ann. Allergy. Asthma Im., 88, 279-282. Clean
Weber, R.W., 2002: Mother Nature strikes back: global warming, homeostasis, and implications for allergy. Ann. Allergy. Asthma Im., 88, 251-252. Clean
Webster, M.D., M. Babiker, M. Mayer, J.M. Reilly, J. Harnisch, R. Hyman, M.C. Sarofim and C. Wang, 2002a: Uncertainty in emissions projections for climate models. Atmos. Environ., 36, 3659-3670. [MoS]
Webster, M.S., P.P. Marra, S.M. Haig, S. Bensch and R.T. Holmes, 2002b: Links between worlds: unravelling migratory connectivity. Trends Ecol. Evol., 17, 76-83. Clean
West, J.J., P. Osnaya, I. Laguna, J. Martinez and A. Fernandez, 2004: Co-control of urban air pollutants and greenhouse gases in Mexico City. Environ. Sci. Technol., 38, 3474-3481. Clean
White, R., 2003: Commentary: What can we make of an association between human immunodeficiency virus prevalence and population mobility? Int. J. Epidemiol., 32, 753-754. Clean
WHO, 2001: World Health Report 2001: Mental Health – New Understanding, New Hope. World Health Organization, Geneva, 178 pp. [NPR]
WHO, 2002a: Injury Chart Book: Graphical Overview of the Burden of Injuries. World Health Organization, Geneva, 81 pp. [NPR]
WHO, 2002b: World Health Report 2002: Reducing Risks, Promoting Healthy Life. World Health Organization, Geneva, 268 pp. [NPR]
WHO, 2003a: Global Defence against the Infectious Disease Threat: Progress Report, Communicable Diseases 2002. World Health Organization, Geneva, 233 pp. [NPR]
WHO, 2003b: The World Health Report 2003: Shaping the Future. World Health Organization, Geneva, 210 pp. [NPR, MoS]
WHO, 2004a: Synthesis Workshop on Climate Variability, Climate Change and Health in Small Island States. WHO, WMO, UNEP, WHO/SDE/OEH/04.02, 95 pp. [NPR]
WHO, 2004b: Malaria epidemics: forecasting, prevention, early warning and control – from policy to practice. Report of an informal consultation, Leysin, Switzerland, 8–10 December 2003. World Health Organization, Geneva, 52 pp. [NPR, MoS]
WHO, 2005: Ecosystems and human well-being: health synthesis. A report of the Millennium Ecosystem Assessment, World Health Organization, Geneva, 54 pp. [NPR]
WHO, 2006: Preventing Disease through Healthy Environments: Towards an Estimate of the Environmental Burden of Disease. World Health Organization, Geneva, 106 pp. [NPR, MoS]
WHO Regional Office for Europe, 2006: 1st meeting of the project “Improving Public Health Responses to Extreme Weather/Heat-waves”. EuroHEAT Report on a WHO Meeting in Rome, Italy, 20–22 June 2005. WHO Regional Office for Europe, Copenhagen, 52 pp. [NPR]
WHO Regional Office for South-East Asia, 2006: Human health impacts from climate variability and climate change in the Hindu Kush-Himalaya region. Report of an Inter-Regional Workshop, Mukteshwar, India, October 2005. WHO, 49 pp. [NPR]
Wilby, R., 2003: Past and projected trends in London’s urban heat island. Weather, 58, 251-260. [ARC]
Wilby, R., M. Hedger and H.G. Orr, 2005: Climate change impacts and adaptation: a science agenda for the Environment Agency of England and Wales. Weather, 60, 206-211. [ARC]
Wilson, J., B. Philips and D. Neal, 1998: Domestic violence after disaster. The Gendered Terrain of Disaster: Through Women’s Eyes, E. Enearson and B.H. Morrow, Eds., International Hurricane Center, Florida International University, Miami, Florida, 115-122. [NPR]
Wittmann, R. and G. Flick, 1995: Microbial contamination of shellfish: prevalence, risk to human health and control strategies. Annu. Rev. Publ. Health, 16, 123-140. Clean
Woodruff, R.E., 2005: Epidemic early warning systems: Ross River virus disease in Australia. Integration of Public Health with Adaptation to Climate Change: Lessons Learned and New Directions, K. Ebi, J. Smith and I. Burton, Eds., Taylor and Francis, Leiden, 91-113. [NPR, ARC]
Woodruff, R.E., C.S. Guest, M.G. Garner, N. Becker, J. Lindesay, T. Carvan and K. Ebi, 2002: Predicting Ross River virus epidemics from regional weather data. Epidemiology, 13, 384-393. [MoS, SRC]
Woodruff, R.E., S. Hales, C. Butler and A. McMichael, 2005: Climate change and health impacts in Australia: effects of dramatic CO2 emission reductions. Report for the Australia Conservation Foundation and the Australian Medical Association. Australian National University, Canberra, 45 pp. [NPR, SRC]
Woodward, A., S. Hales and N. de Wet, 2001: Climate Change: Potential Effects on Human Health in New Zealand. Ministry for the Environment, Wellington, New Zealand, 27 pp. [NPR, SRC]
World Bank, 2004: World Development Report 2004: Making Services Work for Poor People. World Bank, New York, 32 pp. [NPR]
World Bank, 2005: Drought in the Amazon: scientific and social aspects. Report of a World Bank Seminar, December 12, 2005. Brasília, Brazil, 14 pp. [NPR]
World Bank, African Development Bank, Asian Development Bank, DFID, Directorate-Generale for Development European Commission, Federal Ministry for Economic Cooperation and Development Germany, Ministry of Foreign Affairs Netherlands, UNDP and UNEP, 2004: Poverty and Climate Change: Reducing the Vulnerability of the Poor through Adaptation. World Bank, New York, 43 pp. [NPR]
Wu, H. and L. Chan, 2001: Surface ozone trends in Hong Kong in 1985–1995. Environ. Int., 26, 213-222. Clean
WWF, 2005: An overview of glaciers, glacier retreat, and subsequent impacts in Nepal, India and China. World Wildlife Fund Nepal Program, 79 pp. http://assets.panda.org/downloads/himalayaglaciersreport2005.pdf. [NPR]
Wyndham, C., 1965: A survey of causal factors in heat stroke and of their prevention in gold mining industry. J. S. Afr. I. Min. Metall., 66, 125-155. Clean
Xie, S.D., T. Yu, Y.H. Zhang, L.M. Zeng, L. Qi and X.Y. Tang, 2005: Characteristics of PM10, SO2, NOx and O3 in ambient air during the dust storm period in Beijing. Sci. Total Environ., 345, 153-164. Clean
Yang, C.Y., Y.S. Chen, H.F. Chiu and W.B. Goggins, 2005a: Effects of Asian dust storm events on daily stroke admissions in Taipei, Taiwan. Environ. Res., 99, 79-84. Clean
Yang, G.J., P. Vounatsou, X.N. Zhou, M. Tanner and J. Utzinger, 2005b: A potential impact of climate change and water resource development on the transmission of Schistosoma japonicum in China. Parassitologia, 47, 127-134. Clean
Yarnal, B., A.C. Comrie, B. Frakes and D.P. Brown, 2001: Developments and prospects in synoptic climatology. Int. J. Climatol., 21, 1923-1950. [JoC]
Yohe, G. and K. Ebi, 2005: Approaching adaptation: parallels and contrasts between the climate and health communities. A Public Health Perspective on Adaptation to Climate Change, K. Ebi and I. Burton, Eds., Taylor and Francis, Leiden, 18-43. [NPR, SRC]
Young, S., L. Balluz and J. Malilay, 2004: Natural and technologic hazardous material releases during and after natural disasters: a review. Sci. Total Environ., 322, 3-20. Clean
Zebisch, M., T. Grothmann, D. Schroeter, C. Hasse, U. Fritsch and W. Cramer, 2005: Climate Change in Germany. Vulnerability and Adaptation of Climate Sensitive Sectors. Federal Environmental Agency (Umweltbundesamt), Dessau, 205 pp. [NPR, ARC]
Zhou, G., N. Minakawa, A.K. Githeko and G. Yan, 2004: Association between climate variability and malaria epidemics in the East African highlands. P. Natl. Acad. Sci. USA, 101, 2375. [JoC, ARC]
Zhou, G., N. Minakawa, A.K. Githeko and G. Yan, 2005: Climate variability and malaria epidemics in the highlands of East Africa. Trends Parasitol., 21, 54-56. [ARC]
Ziska, L.H., S.D. Emche, E.L. Johnson, K. George, D.R. Reed and R.C. Sicher, 2005: Alterations in the production and concentration of selected alkaloids as a function of rising atmospheric carbon dioxide and air temperature: implications for ethno-pharmacology. Glob. Change Biol., 11, 1798-1807. [JoC]
Zwander, H., 2002: Der Pollenflug im Klagenfurter Becken (Kaernten) 1980–2000. Carinthia II, 192, 197-214.Clean
| Tag | Explanation | Occurrences | Percentages |
|---|---|---|---|
| PoC |
Person of Concern Key individual involved in CRU emails as defined in this spreadsheet. |
1 | 0.1% |
| JoC |
Journal of Concern A Journal which has published articles by one or more PoCs (Person of Concern) |
48 | 8% |
| MoS |
Model or Simulation Reference appears to be a model or simulation, not observation or experiment. |
54 | 9% |
| NPR |
Non Peer Reviewed Reference has no Journal or no Volume or no Pages or it has Editors. |
141 | 25% |
| SRC |
Self Reference Concern Author of a chapter containing references to own work. |
59 | 10% |
| ARC |
Paper authored or co-authored by person who is also in list of Authors of another chapter. |
43 | 7% |
| 2007 |
Paper dated 2007, when IPCC policy stated cutoff was December 2005 |
9 | 1% |
| Clean |
The reference was probably peer reviewed. |
289 | 51% |
NOTE: In the Summary of Reviewer Comments,
Accepted includes only those responses that were unambiguously Accepted.
There are other categories of responses that we have not yet quantified
due to inconsistencies of usage.
| Reviewer | Total Comments | Accepted | IPCC Roles | Papers |
|---|---|---|---|---|
| Government of Argentina | 93 | 0 | 0 | 0 |
| Canziani, OF | 90 | 0 | 2 | 4 |
| Hanson, CE | 59 | 0 | 1 | 2 |
| Goklany, IM | 56 | 0 | 0 | 15 |
| Haines, A | 48 | 0 | 0 | 9 |
| Berry, PM | 44 | 0 | 0 | 8 |
| Government of Australia | 42 | 0 | 0 | 0 |
| Reiter, P | 33 | 0 | 0 | 4 |
| Government of USA | 32 | 0 | 0 | 0 |
| Government of Canada | 27 | 0 | 0 | 0 |
| Morse, AP | 27 | 0 | 0 | 6 |
| Hildebrand, Von | 22 | 0 | 0 | 0 |
| Krupnick, Alan | 20 | 0 | 0 | 0 |
| Knowlton, K | 19 | 0 | 0 | 4 |
| Government of Sweden | 19 | 0 | 0 | 0 |
| Harvey, D | 18 | 0 | 0 | 1 |
| Verhasselt, Yola | 17 | 0 | 0 | 0 |
| Epstein, PR | 16 | 1 | 0 | 11 |
| Jendritzky, G | 14 | 0 | 0 | 5 |
| Xiao, Fengjin | 13 | 0 | 0 | 0 |
| Dhiman, Ramesh | 13 | 0 | 0 | 0 |
| Bartram, Jamie | 13 | 0 | 0 | 0 |
| Sauerborn, Rainer | 12 | 0 | 0 | 0 |
| Tanser, Frank | 11 | 0 | 0 | 0 |
| Government of Ireland | 10 | 0 | 0 | 0 |
| Government of India | 9 | 0 | 0 | 2 |
| van der Linden, Paul | 9 | 0 | 0 | 0 |
| Ogawa, Hisashi | 7 | 0 | 0 | 0 |
| Government of France | 7 | 0 | 0 | 0 |
| Government of Switzerland | 6 | 0 | 0 | 0 |
| Casimiro, E | 6 | 0 | 0 | 3 |
| Smith, JB | 6 | 0 | 4 | 25 |
| Government of China | 6 | 0 | 0 | 0 |
| Moore, TG | 5 | 0 | 0 | 0 |
| Nicholls, N | 4 | 0 | 0 | 18 |
| Republic of Korea | 4 | 0 | 0 | 0 |
| Githeko, AK | 4 | 0 | 1 | 14 |
| Government of Finland | 4 | 0 | 0 | 0 |
| Few, R | 4 | 0 | 0 | 6 |
| Rodo, X | 4 | 0 | 1 | 4 |
| Wang, C | 4 | 0 | 0 | 6 |
| Ando, M | 3 | 0 | 0 | 2 |
| Government of Germany | 3 | 0 | 0 | 0 |
| Fobil, Julius | 2 | 0 | 0 | 0 |
| Bernstein, Lenny | 2 | 0 | 0 | 0 |
| von Hildebrand, Alex | 1 | 0 | 0 | 0 |
| Totals | 868 | 1 | 9 | 149 |
| Reviewer Type | Total Comments | Accepted | % Accepted |
|---|---|---|---|
| Govt | 249 | 0 | 0% |
| IPCC | 468 | 1 | 0% |
| Indep | 151 | 0 | 0% |
| Total | 868 | 1 | 0% |
Main AR4 Index | Working Group WG2 Index | Table of Contents | Authors | Executive Summary | Annotated Text | References | Reviewer Comments